
The role of respiratory therapists in fighting the COVID-19 crisis: unsung heroes in Wuhan
The occupation of respiratory therapy has been an independent medical profession in the United States for more than 70 years, and respiratory therapists (RTs) have a demonstrated effectiveness in caring for critically ill patients. In other regards, respiratory care is a relatively new specialty, being less than 25 years old, when compared with other medical occupations in mainland China (1). Indeed, it was not until 2020 that it became acknowledged as a formal occupation in China, a fact which has limited the development of respiratory care.
During the 2019 novel coronavirus (COVID-19) crisis, the importance of RTs, who have traditionally been neglected in China, has come to the fore. Between February 7 and April 1, 2020, a rescue team from Zhongshan Hospital, Fudan University, assumed control of two COVID-19 wards in the Hubei General Hospital. The team included 130 healthcare personnel from 12 disciplines, including intensivists, emergency physicians, respiratory physicians, nurses, and two RTs. Herein, we review the experience of these RTs from the frontline in Wuhan.
Patient assessment and triage
With the dramatic increase in confirmed cases of COVID-19 in Wuhan, the Chinese government has realized the severity of the this outbreak and has mandated that all suspected and confirmed patients be admitted to hospital to reduce community transmission (2). Consequently, all healthcare institutions endured enormous pressure due to the lack of critical care resources in the face of the COVID-19 epidemic. The rational allocation of limited medical resources is essential to avoid the collapse of the public health system. Therefore, patients with mild symptoms were scheduled to mobile cabin hospitals, and those with severe and critical illness were admitted to the intensive care unit (ICU) (3). Firstline RTs assessed the patients using vital signs, chest computed tomography (CT) scans, lung ultrasound, and blood gas analysis. They also collected the patients’ medical history and helped physicians classify the patients.
Respiratory support
Most COVID-19 patients require respiratory support, including nasal cannula (NC), face mask, high flow nasal cannula (HFNC), non-invasive ventilation (NIV), invasive ventilation and extracorporeal membrane oxygenation (ECMO) support, mainly depending on the arterial oxygen saturation and respiratory rate (4-6). RTs closely monitored these bedside parameters, and appropriate oxygen therapy was recommended or delivered accordingly. During the early period of the COVID-19 epidemic in Wuhan, critical patients were not treated in time due to a lack of intensive care resources (personal protective equipment, ventilators, and trained physicians). Moreover, most physicians were not familiar with the ventilators supplied by other provinces in China. Therefore, RTs with a respiratory support background were regarded as the “giant panda” in Wuhan’s frontline. Not only were they skilled in using the ventilators, but also trained other non-ICU medical staff to cope with critically ill patients supported by mechanical ventilation.
Airway management
Airway management is essential for patients with COVID-19. However, operations such as aerosolization, intubation, extubation, suctioning, and bronchoscopy, involve a particularly high risk of infection (7,8). Consequently, an emergency airway management team was established in Wuhan, which consisted of intensivists, anesthesiologists, and RTs. They are responsible for providing standardized training for nurses and non-ICU physicians, and detailed risk assessment for COVID-19 patients. In clinical treatment, RTs assessed the risk of upper airway dysfunction, sputum volume and nature, cough efficacy, and ventilatory function. Furthermore, they optimized nebulizer to reduce aerosol diffusion, assisted anesthesiologists in pre-oxygenation and intubation, assisted in fiberoptic bronchoscopy and sputum culture, and used closed endotracheal suction for patients with invasive mechanical ventilation.
Patient transportation
Patients with COVID-19 frequently need to be reassessed by chest CT scan based on the development of the disease (9). Some patients supported by mechanical ventilation or even ECMO might also require repeated imaging assessments. The transport of critically ill patients out of the ICU may result in unpredictable risks. Therefore, staff should be familiar with all kinds of oxygen therapies and be able to handle troubleshooting outside of the ICU. In our rescue team, two RTs were responsible for the transport of critically ill patients with mechanical ventilation (Figure 1). They developed transport checklists for patients with different degrees of severity. The respiratory parameters were continuously monitored throughout patient transport.

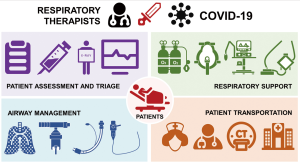
In summary, RTs played a crucial role in the fight against the COVID-19 crisis in Wuhan (Figure 2). However, their impact and sacrifice did not attract public attention. Fortunately, “respiratory therapist” has recently been officially listed as a new occupation, according to the Chinese Ministry of Human Resources and Social Security. Undoubtedly, these medical professionals will play an increasingly important role in the future management of critically ill patients and public health crises.
Acknowledgments
We would like to thank all our colleagues who participated in the Wuhan COVID-19 epidemic task force.
Funding: This study was supported by grants from the Research Funds of Xiamen Branch, Zhongshan Hospital (2019ZSXMYS04), Shanghai Municipal Health Commission (2019ZB0105), Natural Science Foundation of Shanghai (20ZR1411100), Program of Shanghai Academic/Technology Research Leader (20XD1421000) and National Natural Science Foundation of China (82070085).
Footnote
Provenance and Peer Review: This article was a free submission to the journal. The article did not undergo external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/apm-20-1856). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Li J, Ni Y, Tu M, et al. Respiratory Care Education and Clinical Practice in Mainland China. Respir Care 2018;63:1239-45. [Crossref] [PubMed]
- Li Q, Guan X, Wu P, et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia. N Engl J Med 2020;382:1199-207. [Crossref] [PubMed]
- Wu Z, McGoogan JM. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72314 Cases From the Chinese Center for Disease Control and Prevention. JAMA 2020;323:1239-42. [Crossref] [PubMed]
- Phua J, Weng L, Ling L, et al. Intensive care management of coronavirus disease 2019 (COVID-19): challenges and recommendations. Lancet Respir Med 2020;8:506-17. [Crossref] [PubMed]
- Shang Y, Pan C, Yang X, et al. Management of critically ill patients with COVID-19 in ICU: statement from front-line intensive care experts in Wuhan, China. Ann Intensive Care 2020;10:73. [Crossref] [PubMed]
- Tu GW, Liao YX, Li QY, et al. Prone positioning in high-flow nasal cannula for COVID-19 patients with severe hypoxemia: a pilot study. Ann Transl Med 2020;8:598. [Crossref] [PubMed]
- Sullivan EH, Gibson LE, Berra L, et al. In-hospital airway management of COVID-19 patients. Crit Care 2020;24:292. [Crossref] [PubMed]
- Li L, Li R, Wu Z, et al. Therapeutic strategies for critically ill patients with COVID-19. Ann Intensive Care 2020;10:45. [Crossref] [PubMed]
- Su Y, Han Y, Liu J, et al. Tailoring steroids in the treatment of COVID-19 pneumonia assisted by CT scans: three case reports. J Xray Sci Technol 2020;28:885-92. [Crossref] [PubMed]


