
Influence of high-intensity intermittent training on glycolipid metabolism in obese male college students
Introduction
In recent years, China has undergone a period of rapid economic development. Along with rising living standards, the population has also experienced significant changes in diet, which have given way to an annually increasing incidence of obesity among college students (1,2). Obesity, a chronic metabolic disease, can be attributed to various environmental, genetic, and other factors. Obesity occurs when the body takes in more energy than it consumes; over time, the energy balance in the body breaks, resulting in the accumulation of fat in the body (3). Clinical studies have confirmed (4,5) obesity to be an important risk factor for respiratory diseases and various other conditions such as hypertension, hyperlipidemia, diabetes, and coronary heart disease. In male college students, obesity not only impacts the individual’s physical state, but also their psychological state, and even their job or career. Aerobic exercise is an effective way to lose weight. However, a large number of college students struggle to maintain such a regimen over the long term. Therefore, it is crucial that scientific and reasonable intervention measures that will encourage obese male college students to effectively lose weight and ensure the healthy development of their bodies and minds are put into practice. In our college, obese mainly occurs in male individuals. This study analyzed the effects of high-intensity interval training on the metabolism of glucose and lipid in obese male college students. The results are reported as follows.
We present the following article in accordance with the STROBE reporting checklist (available at http://dx.doi.org/10.21037/apm-20-1105).
Methods
The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013) and was approved by the Qufu Normal University.
Study population
Between April 2019 and July 2019, 300 male college students from Qufu Normal University were enrolled in the study. The eligibility criteria were as follows: (I) male college students; (II) over 18 years old; (III) had maintained a stable weight during the 3 months before enrolment; (IV) no existing exercise habits at the time of enrolment; and (V) body mass index (BMI) above 28.0 kg/m2 and over 25% body fat. Individuals with any of the following conditions were excluded: (I) diabetes, angina pectoris, or hypertension; or (II) sports contraindications such as bone and joint disease, heart disease. All participants signed informed consent.
Quality control
First, we investigated the diets of the 300 enrolled students before the exercise intervention, including the type of food, intake amount, and food ingredients, and the total energy intake per day was analyzed. The students were asked to stick to their previous energy intake and eating patterns during this study. Except for the intervention exercise, the students were also instructed to keep their daily physical activity at the same level as before the study throughout the whole study period, to reduce the influence of dietary, exercise, and other factors on the study results.
Sports
To determine the maximum oxygen uptake (VO2max), all the participants were tested on the Pusar cosmos 4.0 running platform by AEGER Oxygen Analyzer for incremental load test. First, they performed a 3-day adaptive exercise, and RPE and heart rate were measured at 60% VO2 max and 85% VO2 max, respectively. All of the study participants exercised 5 days per week for 12 weeks. Each participant performed 50% VO2 max preparation activities for 10 minutes before exercise intervention and then 5 minutes of relaxation activities. The study group undertook high-intensity interval training as follows. The participants exercised for 4 minutes at an intensity of 85% VO2 max with the heart rate controlled at 174 beats/minutes, then exercised at 50% VO2 max for 2 minutes, followed by 5 minutes of relaxation. These steps were repeated five times. The control group undertook aerobic exercise intervention as follows. The participants exercised at an intensity of 60% VO2max for 40 minutes without a break, with the heart rate controlled at 140 beats/minutes. The two groups had similar levels of energy consumption. The total energy consumption was calculated for each exercise. The exercise intervention time of the study group was obtained by dividing the total energy consumption by the average energy consumption at the target heart rate of the control group.
Parameters
The body shape, blood sugar level, and blood lipid level the two groups were recorded before and after intervention. Body shape includes body weight, hip circumference, body fat ratio, waist circumference, and BMI. The BFR was measured by Inbody3.0 body composition analyzer (Biospace, Soul, Korea). On the first morning of this trial, 5 mL of fasting venous blood was collected from all participants, and fasting blood glucose, high-density lipoprotein cholesterol (HDL-C), and low-density lipoprotein cholesterol (LDL-C) were measured by Hitachi 7600 automatic biochemical analyzer. Total cholesterol (TC), triglyceride (triglyceride, TG) levels, and insulin levels were measured by the Bayer ADVIA Centaur automatic immunoassay analyzer.
Statistical analysis
Data analysis was performed using SPSS17.0 software. Continuous data were expressed as mean ± standard deviation (SD), and compared by Student’s t-test. A P value of <0.05 was considered to be statistically significant.
Results
Baseline characteristics of the study group and the control group
Using the random number table method, 300 obese male college students were equally divided into a study group and a control group. The students had an average age of 21.71±1.44 (range, 19–22) years old. There were no significant differences in age, height, weight, BMI, or BFR between the two groups (P>0.05). The baseline characteristics of the participants are listed in Table 1.

Full table
Comparison of body shape before and after intervention between the two groups
After 12 weeks of intervention, the weight, waist circumference, waist-to-hip ratio, BMI, and body fat percentage of the two groups were significantly lower than before the intervention, and the difference was statistically significant (P<0.05). However, there were no statistically significant differences in body weight, waist circumference, waist-to-hip ratio, BMI, or body fat percentage between the two groups (P>0.05). Table 2 compares the body size of the two groups before and after intervention.
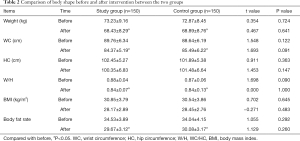

Full table
Comparison of lipid levels between the study group and the control group
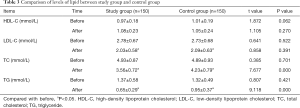
After 12 weeks of intervention, the serum levels of LDL-C, TC, and TG of the students in the two groups were significantly lower than before the intervention, and the difference was statistically significant (P<0.05). The TC and TG levels of the study group were significantly lower than those in the control group, and the difference was statistically significant (P<0.05). The difference in the serum level of LDL-C between the two groups was not statistically significant (P>0.05). Table 3 compares the lipid levels of the two groups before and after the intervention.
Full table
Comparison of blood sugar and insulin between study group and control group
After 12 weeks of intervention, the insulin levels of the two groups of subjects were significantly lower than before the intervention, and the difference was statistically significant (P<0.05). The insulin level of the study group was significantly lower than that of the control group, and the difference was statistically significant (P<0.05). The fasting blood glucose level was not significantly different between the two groups before and after the intervention (P>0.05). Table 4 compares the blood sugar and insulin levels between the two groups before and after the intervention.
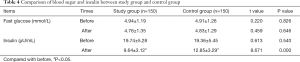

Full table
Discussion
Many studies to date have focused on exercise intervention for obese people, and most of them have achieved a satisfactory fat-reducing effect. Previous studies have revealed that long-term low-intensity aerobic exercise can promote fat consumption in people with obesity. Tremblay et al. (6) found that, at a certain level of energy consumption, high-intensity intermittent exercise can promote the body’s energy metabolism and lipid balance more than low-to-medium-intensity exercise. In recent years, high-intensity interval training, both in China and abroad, has been used, to manage with metabolic syndrome (7), essential hypertension (8), type 2 diabetes (9), and chronic obstructive pulmonary disease (10). While achieving satisfactory results, its safety has also been initially confirmed.
The effect of high-intensity interval training on the lipid metabolism of obese male college students
After 12 weeks of intervention, the serum levels of LDL-C, TC, and TG in the two groups in this study were significantly lower than before the intervention. These results indicate that aerobic exercise and high-intensity interval training could both significantly improve blood lipid metabolism in obese male college students. Moreover, the levels of TC and TG in the study group were significantly lower than those of the control group, which suggests that high-intensity interval training improved the blood lipid metabolism of obese male college students to a greater degree than aerobic exercise did. The reasons for this may include: (I) high-intensity interval training can increase the activity of related lipid metabolism enzymes, or promote the expression of related lipid metabolism enzymes, which in turn promotes blood lipid metabolism. Some scholars have found that the activity of lipoproteinase, which plays an important role in the TG hydrolysis process, is significantly improved by high-intensity interval training (11,12). Meanwhile, high-intensity interval training also promotes the expression of lipid metabolism-related receptors, thus accelerating lipid metabolism. (II) High-intensity interval training accelerates the body’s calorie consumption, which in turn promotes blood lipid metabolism. Matsuo et al. found that with high-intensity interval training, energy is not only consumed by the body during exercise but also during post-exercise rest (13,14). Energy consumption increased by 10% 24–48 hours after high-intensity training, which indicates that the body is in a state of excessive oxygen consumption for a long time after high-intensity interval training, therefore improving the body’s basic metabolic rate. As the main energy source of excess oxygen consumption is fat, high-intensity training can therefore promote blood lipid metabolism. Kraemer et al. found that high-intensity exercise patterns can significantly increase the level of β-endorphin in the body, which is conducive to improving lipid metabolism (15). However, in our study, the difference in LDL-C levels between the two groups of subjects before and after intervention was not statistically significant, which may be explained by the short intervention time and the small sample size.
The effect of high-intensity interval training on blood glucose metabolism and body shape of obese male college students
The results of this study showed that after 12 weeks of intervention, the weight, waist circumference, waist-to-hip ratio, BMI, and BFR of the two groups of study subjects were significantly lower than before the intervention. These results show that obese male college students can achieve a significant reduction in body size through both aerobic exercise and high-intensity interval training. However, no statistically significant differences were found in weight, waist circumference, waist-to-hip ratio, BMI, or BFR between the two groups after 12 weeks of intervention, which may be attributed to the short duration of the intervention. Obese college students are mostly affected by central obesity, which is an important risk factor for type 2 diabetes and ischemic heart disease (16). Obese people generally consume foods with higher fat and sugar content and lack physical exercise; these factors cause blood glucose levels in the body to rise, which can develop into insulin resistance or diabetes. Human blood glucose is regulated by glucagon and insulin. The results of this study showed that there was no significant change in the morning fasting blood glucose levels of the two groups of subjects after 12 weeks of intervention; however, after the intervention, the insulin levels of the two groups were significantly lower, and the insulin level of the study group was significantly lower than that of the control group. These results indicate that high-intensity interval training further improved the glucose metabolism of the obese male college students in this study. Therefore, for obese male college students, high-intensity interval training holds great health benefits.
In summary, aerobic exercise and high-intensity interval training can both significantly improve the body shape of obese male college students. However, high-intensity interval training had a greater effect in improving the glucose and lipid metabolism of obese male college students than aerobic exercise did, and this is deserving of more clinical attention. However, this study had a relatively small sample size and a short study duration. To further clarify the impact of different intensity training methods on the health of obese people, future study will involve larger sample sizes and longer observation times.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at http://dx.doi.org/10.21037/apm-20-1105
Data Sharing Statement: Available at http://dx.doi.org/10.21037/apm-20-1105
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/apm-20-1105). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013) and was approved by the Qufu Normal University. Written informed consent was obtained from all students.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Feng HC. Visualization analysis of exercise intervention for obese college students from 2001 to 2016 in China. Chinese School Health 2018;39:439-41.
- Lv Y, Qin X, Jia H, et al. The Association between Gut Microbiota Composition and Body Mass Index in Chinese Male College Students, as Analyzed by Next-generation Sequencing. Br J Nutr 2019;122:986-95. [PubMed]
- Lim H, Wang Y. Socioeconomic disparities in obesity among children and future actions to fight obesity in China. Ann Transl Med 2019;7:S377. [Crossref] [PubMed]
- Montan PD, Sourlas A, Olivero J, et al. Pharmacologic therapy of obesity: mechanisms of action and cardiometabolic effects. Ann Transl Med 2019;7:393. [Crossref] [PubMed]
- Hamjane N, Benyahya F, Mechita MB, et al. The complications of overweight and obesity according to obesity indicators (body mass index and waist circumference values) in a population of Tangier (northern Morocco): A cross-sectional study. Diabetes Metab Syndr 2019;13:2619-24. [Crossref] [PubMed]
- Tremblay A, Simoneau JA, Bouchard C. Impact of exercise intensity on body fatness and skeletal muscle metabolism. Metabolism 1994;43:814-8. [Crossref] [PubMed]
- Stensvold D, Tjønna AE, Skaug EA, et al. Strength training versus aerobic interval training to modify risk factors of metabolic syndrome. J Appl Physiol 2010;108:804-10. [Crossref] [PubMed]
- Xu SZ, Zhu R. Effects of Short-term High-intensity Interval Training on Sympathetic Vasoconstriction Response at Rest and during Handgrip Exercise of Middle and Elderly Male Patients with Essential Hypertension. Chin J Sports Med 2018;37:468-78.
- Terada T, Friesen A, Chahal BS, et al. Feasibility and preliminary efficacy of high intensity interval training in type 2 diabetes. Diabetes Res Clin Pract 2013;99:120-9. [Crossref] [PubMed]
- Liu JX, Liu XD, Wu WB, et al. Rehabilitation effect and mechanism of high-intensity intermittent training on COPD patients. Chin J Rehab Med 2017;32:1441-4.
- Yang TJ, Wu CL, Chiu CH. High-Intensity Intermittent Exercise Increases Fat Oxidation Rate and Reduces Postprandial Triglyceride Concentrations. Nutrients 2018;10:492. [Crossref] [PubMed]
- Torabi F, Farahani A, Safakish S, et al. Evaluation of motor proficiency and adiponectin in adolescent students with attention deficit hyperactivity disorder after high-intensity intermittent training. Psychiatry Res 2018;261:40-4. [Crossref] [PubMed]
- Matsuo T, Ohkawara K, Seino S, et al. Cardiorespiratory fitness level correlates inversely with excess post-exercise oxygen consumption after aerobic-type interval training. BMC Res Notes 2012;5:646. [Crossref] [PubMed]
- Selected Physiological, Perceptual, and Physical Performance Changes During Two Bouts of Prolonged High-Intensity Intermittent Running Separated by 72 Hours. J Strength Cond Res 2017;31:3474-81. [Crossref] [PubMed]
- Kraemer WJ, Fleck SJ, Callister R, et al. Training responses of plasma beta-endorphin, adrenocorticotropin, and cortisol. Med Sci Sports Exerc 1989;21:146-53. [Crossref] [PubMed]
- Tian Y, Yang SC, Yu CQ, et al. Association between central obesity and risk for heart disease in adults in China: a prospective study. Zhonghua Liu Xing Bing Xue Za Zhi 2018;39:1172-8. [PubMed]


