
A randomized clinical study of the treatment of white lesions of the vulva with a fractional ultrapulsed CO2 laser
Introduction
White lesions of the vulva are a group of chronic diseases that clinically manifest as severe pruritus vulvae along with depigmentation and roughening of the vulvar skin. Pathological studies have shown that white lesions of the vulva, which are also referred to as leukoplakia of the vulva, primarily occur due to secondary degeneration in the epidermis caused by microvascular lesions in the dermis (1), or as a result of growth disorders and epidermal cell degeneration caused by insufficient nutrient supply after nerves and blood vessels degenerate locally (2). White lesions of the vulva are an intractable gynecological disease with a long disease course.
Owing to the unclear etiology of the disease, there is currently no effective radical treatment. Drugs and surgery are popular treatment methods in clinical practice, and acupuncture and traditional Chinese medicine have also been reported to have a therapeutic effect on the disease (3,4). However, despite the short-term effectiveness of these methods, the rate of recurrence is high. Treatment with a traditional carbon dioxide (CO2) laser, an ablative laser, leaves the patient with a large wound with scabs. Massive laser treatment can easily cause pigmentation, discoloration, and scarring. Moreover, controlling the energy density can prove difficult: a low-powered laser cannot obtain the desired effect, while laser therapy with deeper penetration may cause complications such as bleeding. Fractional CO2 lasers are a minimally invasive treatment method based on multifocal laser technology. To achieve the therapeutic effect, a high-energy laser beam is generated and delivered onto the skin. The precise fractioning of the laser beam allows high-density laser energy to be directed at a specific area, avoiding injury to the surrounding normal skin. Tissue swelling is therefore reduced, which accelerates the recovery of the epithelial tissue at the treated area and lowers the risk of scars and infection. Additionally, laser micro-ablation and heating can have a lightening effect on pigment spots and freckles, promote the absorption of pigment cells, and accelerate pigment metabolism. The pigment of the partially leukoplakic skin in particular can be remarkably lightened and even return to normal.
Current research has focused on reducing recurrence of the disease and developing more effective methods that can be safely used in repeated treatments. High-intensity focused ultrasound (HIFU) has proved effective in treating white lesions of the vulva. HIFU does not cause scabbing or shedding and, as there is no scarring, the epidermis remains intact. However, HIFU uses high-frequency ultrasound, which means its operation must be standardized. The skin in the treatment area must be closely observed for any morphological changes, and the ultrasound treatment dose should be adjusted timely to avoid skin burns caused by improper dosage. Furthermore, transient edema may occur in the local tissue following ultrasound treatment. Skin damage can be reduced by applying ice to physically cool the area, thereby ensuring the safety of the treatment. Although super pulse CO2 laser technology has only been applied in clinical settings for a short time, its therapeutic effect is comparable to that of focused ultrasound. Its advantages include small wound stimulation and having a definite therapeutic effect, short treatment duration, and few complications. Moreover, it can be used for repeated treatments, quick repair, and has a fast recovery time; thus, patients’ daily and working lives are largely unaffected.
In this study, we used a fractional ultrapulsed CO2 laser to treat patients with white lesions of the vulva and compared their treatment outcomes with those of patients who received high-intensity focused ultrasound, with the aim of investigating the effectiveness, safety, and feasibility of fractional ultrapulsed CO2 lasers in treatment of white lesions of the vulva. We present the following article in accordance with the CONSORT reporting checklist (available at http://dx.doi.org/10.21037/apm-20-1085).
Methods
Research subjects
A total of 60 patients with white lesions of the vulva who were treated in the Center for Diagnosis and Treatment of Cervical Diseases of Changzhou Maternal and Child Health Care Hospital between December, 2017, and December, 2018, were enrolled as the study subjects and the patients were randomly divided into two groups. The patients ranged in age from 38 to 67 years old, with a median age of 43.3 years. The median disease duration was 4.6 years (range, 5 months to 11 years). The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Inclusion criteria were as follows: patients with no acute vulvar or vaginal inflammation, patients who were not pregnant or breastfeeding, and patients with no comorbidities such as cardiovascular or psychiatric diseases. This study was approved by the Ethics Review Committee of Changzhou Maternal and Child Health Care Hospital. All of the patients enrolled participated in this study voluntarily, and a signed informed consent form was obtained from each patient before colposcopic biopsy or treatment was performed.
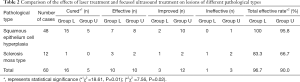
The pathological diagnosis of all 60 patients before treatment was nonmalignant lesions: 48 patients were diagnosed with squamous-cell hyperplasia, and 12 patients were diagnosed with lichen sclerosis. Table 1 shows the patient age distribution and histopathological types. The histopathological changes were determined according to the standard in Blaustein’s Pathology of the Female Genital Tract (Robert J. Kurman, et al. Ronnert. 2019 Springer).
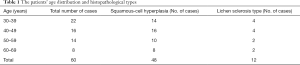

Full table
Therapeutic equipment
Laser treatment group (group L)
A fractional ultrapulsed CO2 laser treatment system (Femilift, Alma Lasers, Israel) was used. The handpieces had a 7×7 or 9×9 pixel array, and during treatment, a frequency of between 60 and 120 Hz was used.
Ultrasound treatment group (group U)
The CZF-1 focused ultrasound treatment system (Chongqing Haifu Medical Technology Co., Ltd., Chongqing, China) was used. The system had an operating frequency of 5–8 MHz and a treatment head 12 mm in diameter.
Therapeutic methods
Group L
Preoperative preparation: After being fully informed of their conditions, the refractoriness of the disease, and the uncertainty of treatment outcome due to individual differences, the patients signed the informed consent form. Women of childbearing age were treated 3–7 days after the end of their menstrual period, while menopausal women could be treated at any time. All patients were required to be free of lower-genital-tract infections before the operation. Cases of vulvitis or vaginitis were treated before the operation. Before the operation, colposcopy was performed to collect preoperative images for documentation. Surgical nurses cleaned and prepared the vulvar skin of the patient, fully exposed the treatment site, and applied a 1-cm-thick layer of lidocaine cream to the lesions before massaging the cream into the skin. Then, the vulva was covered with plastic wrap for approximately 40 minutes to maximize the anesthetic effect of the lidocaine.
Operative procedure: With the patient in the lithotomy position, the remaining lidocaine cream was wiped from the surface of the skin, and routine disinfection and draping were performed. Depending on the area and degree of depigmentation of the white lesions on the vulvar skin, a 7×7 or 9×9 handpiece was selected. The energy density was set at 40–50 mJ/pixel; the power was set to low, medium, or high, according to the patient’s condition; and the pulse mode was set to ‘repeat’. The treatment parameters were adjusted according to the patient’s level of pain tolerance. The front end of the laser handpiece was held perpendicular to and approximately 1 cm away from the skin surface, and the laser scanning was performed from the inside outwards. In most cases, the lesions were scanned by the laser 3–4 times in one treatment until the skin turned slightly red.
Postoperative treatment: No special treatment was needed after treatment, but the treatment site needed to be kept dry. The patients were also instructed to avoid spicy foods and to get adequate rest. The patients were re-examined every 2 weeks so that any changes in signs and symptoms could be monitored. According to the severity of a patient’s condition, the frequency of treatments was adjusted. In general, the patients received one treatment per month.
Group U
The vulvar skin was routinely disinfected and prepared before the treatment. After local anesthesia with 1% lidocaine, a special coupling agent was applied as a medium. With the treatment head in close contact with the white lesions of the vulva through the medium, linear and uniform scanning was performed at a speed of 2–3 mm/sec to 3–5 mm beyond the diseased tissue. When the skin at the scanning site reddened slightly, showed edema, and a warm sensation lasting over 30 seconds, the scanning was stopped. A burn ointment was applied within 24 hours after the treatment, and an ice pack was applied to the treated site every 5 minutes until the patient went to bed to reduce local tissue edema. For patients whose conditions were severe, the treatment could be repeated after 2–3 months.
Determination of efficacy
All of the patients were evaluated 1 month after the end of the first treatment, and the clinical therapeutic effects and side effects were observed. The area algorithm in the textbook for the 8-year obstetrics and gynecology program was used to evaluate the clinical outcomes based on the degree to which the pruritus symptoms had been reduced, as well as the change in skin color and the recovery of skin elasticity. Clinical outcomes were categorized as follows:
Cure: The symptoms of pruritus had disappeared, and the color and elasticity of 80% or more of the lesioned skin had returned to normal. Effective: the symptoms of pruritus had basically disappeared, and the color and elasticity of 60–79% of the lesioned skin were close to normal. Improved: the pruritus had been relieved, and the color and elasticity had improved in 20–59% of the lesioned skin. Ineffective: the pruritus had not been relieved, and no improvements were seen in the color or elasticity of the skin. Overall effective rate = number of cured, effective, and improved cases/total number of cases × 100%.
Observation of side effects: During surgery, patients were required to report their symptoms, especially pain or a burning sensation. All of the patients were regularly followed up once every 2 weeks. During follow-up, changes in local signs, symptoms, and complications were recorded.
Statistical methods
IBM SPSS Statistics 13.0 was used for data analysis. Count data were analyzed with the χ2 test, and the t-test was used to analyze measurement data. A P-value of <0.05 indicated a significant difference.
Results
General information
The average age of the patients was 42.15±3.06 years old in group L and 44.02±1.35 years old in group U. The average disease duration in group L was 4.53±0.58 years compared with 4.68±0.32 years in group U. There were no significant differences in age or disease duration between the groups (P>0.05).
Intraoperative and postoperative reactions
No abnormal vital signs or obvious adverse reactions were observed among the 30 patients in group L during or after the operation. The skin in the treatment area was reddish and slightly swollen, and the symptoms generally disappeared the day after the surgery without special treatment.
In group U, 10 patients had a long bleeding time from the site where local anesthesia was injected. Five patients developed mild burns and painful blisters in the treated area but recovered after anti-inflammatory and symptomatic treatment. In all patients, the treated skin became red and swollen within half an hour after the operation and apparent local edema and locally hardened subcutaneous tissue developed in the following 1–2 days. After 1 week, the local edema was completely resolved, but the subcutaneous tissue was still slightly hard, and 7 patients had subcutaneous nodules.
Therapeutic effects
Group U
The enrolled patients came to the hospital for monthly follow-up examinations for 1 year. Among the 30 patients in group U, treatment cured 5 cases (all squamous-cell hyperplasia), was effective in 10 cases (8 squamous-cell hyperplasia and 2 lichen sclerosis), improved 12 cases (10 squamous-cell hyperplasia and 2 lichen sclerosis), and was ineffective in 3 cases (1 squamous-cell hyperplasia and 2 lichen sclerosis). The total effective rate was 90.0%. Six months after the discontinuation of treatment, there were three cases of recurrence (with the patients showing obvious symptoms of pruritus vulvae), constituting a recurrence rate of 10.0%. For these three patients with recurrence, good therapeutic effects were achieved after retreatment with focused ultrasound, and no deformity or scarring was observed in the vulva.
Group L
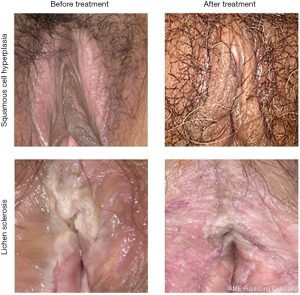
Among the 30 patients in group L, treatment cured 16 cases (15 squamous-cell hyperplasia and 1 lichen sclerosis), was effective in 10 cases (7 squamous-cell hyperplasia and 3 lichen sclerosis), improved 3 cases (2 squamous-cell hyperplasia and 1 lichen sclerosis), and was ineffective in 1 case of lichen sclerosis. The total effective rate was 96.7%. Six months after the treatment was stopped, one patient reported mild symptoms of pruritus vulvae, and good therapeutic effects were achieved after laser treatment was performed again (Table 2). Figure 1 shows the appearances of these lesion types before and after treatment.
Full table
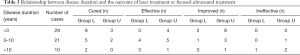
Relationship between therapeutic effect and onset time in groups L and U
The therapeutic effect was closely related to the onset time in both groups. The shorter the disease duration, the better the therapeutic effect (Table 3).
Full table
Discussion
White lesions of the vulva are an intractable gynecological disease with a long disease course. Severe pruritus, which is an unpleasant condition that impedes the patient’s ability to live and work normally, is one of the typical symptoms. Currently, the commonly used drug-based methods used to treat this disease include the topical application of hormones (androgens and glucocorticoids), sitz baths, and the topical application of Chinese herbal medicines. Although drug-based treatments can, to a degree, alleviate the symptoms of white vulvar lesions, the outcome is often unsatisfactory. Patients with severe symptoms may be treated with surgery. However, the resection of a large area of vulvar skin leads to skin contractures and hypertrophic scarring. Postoperative recurrence is also common. In this study, the control group was treated with high-intensity focused ultrasound. Although this achieved good efficacy compared with conventional treatment methods, the patients experienced a considerable number of intraoperative and postoperative complications, intraoperative burns, and painful blisters in the area of treated skin. Localized edema lasted for a long time after the operation, which affected the patients’ daily life and work. Some patients also developed subcutaneous nodules.
The mechanism through which ultrasound treats white lesions of the vulva may be as follows: since ultrasound can easily penetrate and locate tissues, high-frequency ultrasound can be applied in tissues and focused into the dermal layer of the skin to exert its biological effects (e.g., thermal and cavitation effects). The energy is absorbed by the tissue, which rapidly heats up, generating biochemical reactions that eventually denature the diseased tissue. Consequently, the tissue is reconstructed, which increases the number of microvessels in the dermis and returns the blood vessel cavity to normal. Finally, microcirculation in the dermis as well as the nutrition of the local tissue are improved, and the epithelial cells return to normal, thus achieving the desired therapeutic effects. The core of the fractional ultrapulsed CO2 laser technology used in this study is the CO2 laser. It is a minimally invasive technology that through multi-point focusing laser technology, generates uniformly arranged micro-laser pixels through nearly 100 micro lenses, producing high-energy laser beam. The laser is delivered onto the skin, achieving a therapeutic effect. Meanwhile, HP thermal imaging beam technology uses beam separation to deliver a matrix of tiny laser beams onto the skin surface, forming thousands of micropores of a depth sufficient for causing thermal damage. Heating the cells instantly disintegrates, kills, and removes the diseased tissue and promotes tissue regeneration. It has anti-inflammatory and analgesic effects, relieves itching, and can also improve the nutritional status of local tissues. Super pulse matrix CO2 laser is highly efficient. The precise fractioning of the laser beams supports the generation of high-density local laser energy, which can reduce heat conduction and carbonization in the surrounding tissues and avoid damaging the normal surrounding skin. There is less swelling in the tissue, which accelerates the recovery of epithelium at the laser treatment area and lowers the risk of scarring and infection. Moreover, laser micro-ablation and heating can lighten the pigment spots and freckles, promote the absorption of pigment cells, and accelerate pigment metabolism. In particular, the pigment of the partially leukoplakic skin can be remarkably lightened and even return to normal. The CO2 laser has a very small divergence angle and a high energy density, which can rapidly increase the temperature of the skin in the treatment area, causing vaporization and exfoliation of local tissue (5). After irradiation with a CO2 laser, hyperproliferative fibroblasts can produce collagen and extracellular matrix to promote healing of the skin mucosa (6). With the advances in technology, fractional ultrapulsed CO2 lasers have become a focus of attention in the medical field. Fractional ultrapulsed CO2 lasers provide a minimally invasive treatment method and can achieve therapeutic effects quickly. Furthermore, the treatment is associated with only minor side effects and has a short recovery time (7). In fractional ultrapulsed CO2 laser treatment, the beams are separated with a heating pixel (8,9), which forms a matrix of small laser beams on the skin surface and causes thermal damage to thousands of micropores at a certain depth. The cell temperature increases instantaneously, the diseased tissue is quickly disintegrated and cleared, and tissue regeneration is promoted, achieving anti-inflammatory, antipruritic, and pain-relieving effects, thereby improving the nutritional status of local tissues (10). Furthermore, precise treatment positioning and the high laser energy density reduce the heat transfer to the surrounding tissues, avoid burns, reduce tissue edema, accelerate the healing of epithelial tissues, reduce the risk of scarring and infection (11,12), and avoid damage to the surrounding normal skin tissue. The thermal effect of micro ablation with a fractional ultrapulsed CO2 laser can also promote the absorption of pigment cells and accelerate metabolism (13,14), which means the skin can return to a normal or nearly normal color. So far, this technology has mostly been used by dermatologists and plastic surgeons for its excellent cosmetic effects, such as removing freckles (15-17).
In this study, treatment with the fractional ultrapulsed CO2 laser was shown to have good efficacy compared with focused ultrasound. Fractional ultrapulsed CO2 laser treatment showed high clinical efficacy, with a total effective rate of 96.7% and a cure rate significantly higher than that of the control group treated with focused ultrasound. During treatment with the fractional CO2 laser, the surgeon can adjust the parameters according to the patient's condition and level of pain tolerance (18). Therefore, none of the patients reported discomfort. After the operation, local redness only lasted for a short time, there was generally no scarring, and the epidermis remained intact. Except for daily cleaning of the skin, no special treatment was required. After treatment, the numbers of micro vessels, fibroblasts, and nerve endings in the dermis increased, the mitochondria and pigment particles in the cytoplasm increased significantly, and melanocytes were observed in the basal layer (19,20). During 1-year follow-up, 3 patients from group U relapsed within 6 months after the first treatment session, showing obvious pruritus symptoms; however, these symptoms improved after a second ultrasound treatment session. One patient in group L experienced mild itching symptoms, which completely disappeared after a second laser treatment session.
In summary, fractional ultrapulsed CO2 laser treatment has definite efficacy in treating white lesions of the vulva. It causes little damage to the lesioned tissue, has a good safety profile, leads to few complications, and can be used for repeated treatments. Furthermore, patients treated with fractional ultrapulsed CO2 lasers make a fast recovery, and the treatment has little impact on their daily life or work. It is currently the most ideal treatment method for white lesions of the vulva and is worthy of popularization and application in clinical practice.
Acknowledgments
Funding: Jiangsu Provincial Youth Medical Key Talent Project (QNRC2016303); Key project of Science and Technology Development Fund of Nanjing Medical University (2017NJMUZD045); General scientific research project of Jiangsu Provincial Health Commission (H2018018).
Footnote
Reporting Checklist: The authors have completed the CONSORT reporting checklist. Available at http://dx.doi.org/10.21037/apm-20-1085
Data Sharing Statement: Available at http://dx.doi.org/10.21037/apm-20-1085
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/apm-20-1085). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). This study was approved by the Ethics Review Committee of Changzhou Maternal and Child Health Care Hospital (No. 201730). All enrolled patients voluntarily participated in this study and signed an informed consent form before colposcopic biopsy or treatment.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Qiu S, Li Y. Advancements in the traditional Chinese medicine treatment of vulvar dystrophy. Diet Health 2016;3:244-5.
- Wu AH. Effects of focused ultrasound treatment plus Chinese medicine on nerve growth factors and substance P in patients with white lesions of the vulva. Modern Journal of Integrated Traditional Chinese and Western Medicine 2017;26:2577-9.
- Liu HY, Li Y. Clinical experience of Professor Yan Li in the treatment of white lesions of the vulva. Journal of Practical Gynecologic Endocrinology 2019;6:195-7. (Electronic Edition).
- Li L. Acupuncture combined with auricular-plaster therapy in the treatment of 20 cases of white lesions of the vulva. Zhongguo Zhen Jiu 2012;32:394. [PubMed]
- Ma JB. Therapeutic effect of ultrapulsed carbon dioxide fractional laser for treating hypertrophic scar after burn. International Journal of Biomedical Engineering 2018;41:296-300.
- Zhang ZY. Working principle, characteristics, and application of lasers in gynecological surgery. Chinese Journal of Practical Gynecology and Obstetrics 2016;32:607-8.
- Song Y, Dai F, Sui L, et al. Clinical analysis of 191 cases of vaginal and vulvar intraepithelial neoplasia treated with CO2 laser vaporization. Fudan University Journal of Medical Sciences 2015;42:511-6.
- Ma L, Wen HC, Jian XP, et al. Pixel TM2940Er: YAG laser therapy of superficial scars. Chinese Journal of Aesthetic and Plastic Surgery 2016;27:410-2.
- Cheng H, Zhang ZJ, Li YF. Study on Laser Beam Homogenization in Temperature Sensor Calibration. Laser Journal 2017;38:44-7.
- Guo ZX. Observation of the efficacy of fractional ultrapulsed CO2 laser in the treatment of chronic eczema. Journal of Dermatology and Venereology 2018;40:591-2.
- Xue YN, Xu P, Li F, et al. Fractional CO2 laser combined with a collagen dressing for the treatment of atrophic facial acne scars: a clinical observational study. Chinese Journal of Dermatology 2015;48:193-4.
- Han F. The efficacy of fractional ultrapulsed CO2 laser in the treatment of scars on the body surface. Chinese Journal of Medical Aesthetics and Cosmetology 2014;20:471-2.
- Pagano I, Gieri S, Nocera F, et al. Evaluation of the CO2 Laser Therapy on Vulvo-Vaginal Atrophy (VVA) in Oncological Patients: Preliminary Results. Journal of Cancer Therapy 2017;19:452-63. [Crossref]
- Zhu CL, Liu XZ, Zhang Q. Application effect of laser treatment in patients with vitiligo. Nursing Practice and Research 2019;16:140-2.
- Liu Y. Analysis of the Clinical Effect of Carbon Dioxide Lattice Laser Cosmetology in the Treatment of Skin Diseases. Systems Medicine 2018;3:95-7.
- Hu WY. Ultrapulsed CO2 Fractional Laser Skin Resurfacing in Application. Medical Information 2015;(18):72-3.
- Xia J, Hu D. Clinical application and progress of non-ablative fractional laser in dermatology. Chinese Journal of Aesthetic Medicine 2015;25:73-7.
- Pagano T, De Rosa P, Vallone R, et al. Fractional microablative CO2 laser for vulvovaginal atrophy in women treated with chemotherapy and/or hormonal therapy for breast cancer: a retrospective study. Menopause 2016;23:1108-13. [Crossref] [PubMed]
- Salvatore S, Nappi RE, Zerbinati N, et al. A 12-week treatment with fractional CO2 laser for vulvovaginal atrophy: a pilot study. Climacteric 2014;17:363-9. [Crossref] [PubMed]
- Salvatore S, Leone Roberti Maggiore U, Athanasiou S, et al. Histological study on the effects of microablative fractional CO2 laser on atrophic vaginal tissue: an ex vivo study. Menopause 2015;22:845-9. [Crossref] [PubMed]


