
COVID-19 with pleural effusion as the initial symptom: a case study analysis
Introduction
In December 2019, a new pneumonia caused by SARS-CoV-2 reported in Wuhan, China (1,2). The World Health Organization officially named it the 2019 coronavirus disease (COVID-19). COVID-19 is not only swift, but also deadly, and human-to-human transmission is the primary way to cause infection (3). It has become a global epidemic, killing hundreds of thousands of people. The main clinical symptoms of COVID-19 patients are fever, cough, shortness of breath, diarrhea, and vomiting (4). Although some drugs have been used clinically, including remdesivir, chloroquine phosphate, arbidol, lopinavir, and ritonavir, and certain drugs have antiviral effects in patients, there is no definite effective drug (5). However, the antiviral effects of these drugs still require large-scale studies to verify. Here, we report a case of COVID-19. She suffered trauma in a car accident in late January 2020 and described her medical history, clinical diagnosis, changes in clinical parameters, and outcome. Compared with previous studies, there were two innovations in this study: (I) the first symptom of pleural effusion was reported in this case, but there were few reports on such symptoms in the past; (II) this case was reported combined with traffic accident injuries. No such reports were found in relevant literatures.
Case presentation
This study was conducted on a 31-year-old woman born in Pingyao, Shanxi Province, and lived in Wuhan. She was initially admitted to the hospital because of persistent coughing for four days and later for a traumatic experience of a car accident. The patient was healthy before, and no history of hypertension, diabetes, infectious diseases, surgery, trauma, coronary heart disease, cerebrovascular disease, blood transfusion, or food allergy was reported, except for allergies to cephalosporins. On 20 January 2020, at 6:00 p.m., the patient developed dry coughs without mucus or fever. Later, at 8:00 p.m., she visited the Wuhan People’s Hospital for a physical examination, upon which the symptoms of bilateral pleural effusion (BPE) were identified, and the patient was advised to get enough rest and receive anti-infective therapy. The next morning at 6:00 a.m., the patient was discharged and picked up by her friends (a male and a female) to leave for Taiyuan. On 22 January 2020, at around 4:00 a.m., the patient had a car accident and lost consciousness, and at 10:00 a.m., she was sent to the Emergency Department of the Wuxiang People’s Hospital. When the patient gained her consciousness, she complained of pains in her abdomen, chest, and left arm, but reported no sensation of dizziness or vomiting. The head CT scan showed a left orbital rim fracture. Then, the patient was transferred to the First Hospital of Shanxi Medical University, and proper treatment was provided (without exact details). On 24 January 2020, the patient gave the nasopharyngeal/oropharyngeal swab test, and positive SARS-CoV-2 results were reported, showing that the patient was suspected of having COVID-19. At 11:00 p.m., the same day, the patient was transferred to our hospital.
Admission physical examination: T: 36.9 °C, P: 80 bmp, R: 20 bmp, BP: 124/72 mmHg. The patient was clear-headed and utterly sane, but appeared to be less sharp in thought and action. She could answer to the point and cooperate during the physical examination. Her eyelids were swollen and bruised, but her eyesight was not impaired. A laceration, approximately 1 cm, was observed on the arbidol, and the margins were sharp and clear. Bilateral pupils were equal and round, 3 mm in diameter, and reactive to light. Transudates could be seen coming out from behind the right ear. A black scab was found in the left nostril. The neck was soft without resistance.
No superficial lymph nodes were palpable on the body, the tonsil was not unusually large, and there was light congestion seen in the pharynx. The trachea was centered and weakened respiratory sounds with moist rales were detected in both lungs. The heart rate was regular (HR =80 bpm). The abdomen was soft, with tenderness, but no rebound tenderness in the left costal cartilage. The liver and spleen were not palpable under the abdominal ribs. No shifting dullness was heard, and the gurgling sound became less active. The left-arm had a limited range of motion and was held in place using a plaster cast. The right arm showed normal movements. The toes of the right foot were swollen and in pain. The muscle strength of the limbs was grade IV+, while the muscle tension was normal. No pathologic reflex was detected. No edema was found in the lower limbs.
Auxiliary examinations of the head, chest, and abdomen CT (by the First Hospital of Shanxi Medical University, 22/01/2020) were performed. (I) Multiple fractures were observed in the superior wall of the right orbit, the medial and lateral walls of the left orbit, and the peripheral wall of the maxillary sinus; the surrounding muscular soft tissue was swollen, and effusion was found in the left maxillary sinus and the bilateral sphenoidal sinuses. (II) Ethmoidal sinusitis was detected in the bilateral ethmoid sinuses. (III) Hypostatic pneumonia was observed in the lower lobes of the lungs. (IV) A plaque-like hyperintense shadow was noted in the upper lobe of the left lung, and inflammation or contusion was considered. (V) A small nodule was found in the left lobe of the thyroid gland. (VI) A hypointense nodule was observed in the lateral segment of the left hepatic lobe. (VII) No apparent abnormalities were observed in the head CT.
Routine blood test (by the First Hospital of Shanxi Medical University, 22/01/2020): #WBC 12.5×109/L, ALC 0.94×109/L. The electrolyte levels and the liver and kidney functions are normal.
Diagnosis: COVID-19 (severe) and traumatic injuries caused by a car accident, including a basal skull fracture. The individual has multiple fractures in the superior wall of the right orbit, the medial and lateral walls of the left orbit, and the peripheral wall of the maxillary sinus. There was effusion in the left maxillary sinus and the bilateral sphenoidal sinuses and bilateral ethmoidal sinusitis. Further, the patient was observed to have cerebrospinal fluid (CSF) otorrhea, fractures in the ribs, ulnar shaft, and toes of the right foot. They also had skin contusion, hypostatic pneumonia in the lower lobes of the lungs, contusion of the lungs, consider the possibility of pancreatic contusion, concussion, a small thyroid nodule, and a hypointense nodule in the lateral segment of the left hepatic lobe.
The patient was isolated and treated upon admission. Nasal catheter oxygen inhalation was given during necessary laboratory tests.
Live blood analysis: #RBC: 4.43×1012/L; Hb: 114 g/L; #WBC: 4.43×1012/L; NEU%: 71.0%; ALC: 0.95×109/L; #BPC: normal; CRP: 6.24 mg/L.
Liver function: AMS: 36.6U/L; coagulation function: normal. The following medications were administrated: antiviral medicines [lopinavir/ritonavir (LPV/r), II tab PO bid; rHu IFN-alpha 1b, 500 IU inh bid], hormonotherapy (methylprednisolone hemisuccinate, 40 mg injection bid), immune support (Ig, 50 mL IV injection QD) and traditional Chinese medicine (Lianhua Qingwen capsules, 4 cap PO tid; Xuebijing injection, 100 mL injection bid).
Chest CT (25/01/2020): Hazy ground-glass opacity (GGO) was observed in the lingular segment of the left upper lobe; streak shadows were seen in the lower lobes of the bilateral lungs near the pleurae; arc, fluid-filled, dense shadows were noted in the bilateral thoracic cavities, and increased pleural effusion was detected (Figure 1A).
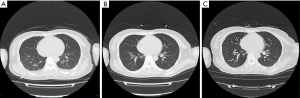
BG analysis: PH: 7.375; OPP: 104.4 mmHg; SPO: 297.9%. On 25 January 2020, the patient was additionally administrated with Ulinastatin (200,000 IU, IV injection tid). On 26 January 2020, the patient complained of hearing loss of the right ear and discharge of some clear liquid mixed with blood from the nostrils, which were likely sequelae of the traumatic injuries. On 28 January 2020, the methylprednisolone hemisuccinate for injection was reduced to 20 mg, twice per day.
Chest CT (30/01/2020): streak shadows were detected in the lower lobes of the bilateral lungs near the pleurae; arc, fluid-filled, dense shadows were observed in the bilateral thoracic cavities (Figure 1B). On 1 February 2020, the patient underwent a live blood analysis and liver and kidney function tests, and the results were all normal. On 5 February 2020, the patient took the nasopharyngeal/oropharyngeal swab test again and was retested positive for SARS-CoV-2. On 8 February 2020, the test result was positive again, and Arbidol tablet (0.2 gr PO tid) was added to the treatment regimen. On 12 February 2020, she retook the test and was still positive for SARS-CoV-2. Finally, on 14 February 2020, the test result eventually turned negative, and so did the results of the following nasopharyngeal/oropharyngeal swab tests on 16 and 18 February 2020.
Chest CT (16/02/2020): the pleural effusion in the bilateral thoracic cavities was at the same level, as shown in the chest CT scan on 30 January 2020 (Figure 1C). On 18 February 2020, the patient was discharged. After discharge, the patient continued to be isolated for 28 days, taking acetylcysteine effervescent tablets 0.6 g/time, twice/day. During the isolation period, vital signs were stable, body temperature was normal and there was no discomfort. Chest CT was reexamined one month after the end of isolation: no effusion was found in both pleural cavity and pleural effusion was completely absorbed. At present (August 26), the patient has no symptoms such as cough, sputum, fatigue and tightness of gas, and is in good condition. During the course, patient is optimistic and actively accepts treatment, and no severe side reaction. All procedures performed in studies involving human participants are following the ethical standards of the institutional and national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
Discussion
On 20 January 2020, at 6:00 p.m., the patient developed dry coughs without mucus or fever and visited the Wuhan People’s Hospital to seek medical attention. After a series of physical examinations, BPE was considered. On 22 January 2020, the patient had a car accident at around 4:00 a.m. and lost consciousness in the accident. On 24 January 2020, the patient tested positive for SARS-CoV-2 infection. The patient underwent chest CT when she developed a dry cough on 20 January 2020 and was suspected of having BPE because no visible lesion was found in her lungs, and both the white blood cells and neutrophils in the bloodstream appeared to be normal. Here, pleural effusion is the first symptom is uncommon for patients infected with SARS-CoV-2. Most COVID-19 patients first symptom is given priority to with symptoms of respiratory system, such as Fever, Cough, Tiredness, Shortness of breath or difficulty breathing, Muscle aches, Chills, Sore throat, Runny nose, Headache, Chest pain, but there are a few cases is starting symptoms with other symptoms, such as have to digestive tract symptoms such as nausea, vomiting, abdominal pain, diarrhea,Or New loss of taste or smell, olfactory dysfunction and other neurological symptoms were the first symptoms. However, these are mostly case reports and no larger data epidemiological investigation has been conducted. More data are needed to answer the question of the significance and impact of these symptoms on COVID-19. Therefore, COVID-19 was not taken into consideration, and the patient was not recommended for home isolation. Zeng et al. (6) found GGO became consolidation in the rapidly progressive period of H7N9 infection and quickly spread to the lobes of the lungs, where multiple, diffuse pulmonary nodules would develop in the lungs; meanwhile, pleural effusion was present in the thoracic cavities; sometimes, pericardial effusion and even peritoneum might occur. In a study that involved 16 severe H7N9 infection cases, nine patients showed a low level of pleural effusion. Five suffered from moderate pleural effusion, four had mild seroperitoneum, and seven experienced mild pericardial effusion (7). In critical cases of influenza A virus subtype H1N1 (A/H1N1) infection, the imaging features include GGO, plaque-like shadows, massive consolidation of the lungs, pleural effusion, and pneumothorax (for patients who require mechanical ventilation) (8). To date, our hospital has admitted 86 patients with COVID-19. Among those, only three patients had pleural effusion. None of the three coVID-19 patients with pleural effusion in our hospital had recurrence as of August 26. With pleural effusion being a less common symptom of COVID-19, doctors might not make a correct diagnosis as the patient’s initial chest CT scan shows no lesions in the lungs.
In this case, the trauma occurred after coVID-19 infection. During the course of coVID-19, such accident trauma may have a certain influence on the outcome and prognosis of the patient. In particular, carefully identify pulmonary contusions following car accident injuries from COVID-19. Fever and cough (mostly dry cough) are relatively high in the early stage of COVID-19. Normal or reduced white blood cell count and reduced lymphocyte count in peripheral blood are typical changes of COVID-19. Patients with pulmonary contusion have cough in the early stage, but most of them have blood sputum and yellow sputum. The total number of white blood cells in peripheral blood is normal or increased, and lymphocytes are normal. In the later stage, secondary infection may lead to fever and other conditions. Severe pulmonary contusion worsens with acute respiratory distress syndrome (ARDS) 12–48 h after injury. Both have their own characteristics in chest CT imaging. The CT imaging manifestations of COVID-19 are mostly multiple small plaques and interstitial changes in the early stage, most of which are subpleural distribution and obvious peripheral pulmonary bands, and then develop into multiple ground glass shadows and infiltrates of both lungs. In severe cases, lung consolidation may occur, and pleural effusion is rare. CT imaging manifestations of lung contusion mainly include increased lung texture, thickened lung, blurred lung outline, accompanied by blotchy shadows or blurred edges, which are related to the injured site. Most of them are distributed across the lobes and segments, mainly in the injured side lung. Due to the distant effect, contusion of the contralateral lung can also be seen, and pleural effusion is more common. The symptoms and imaging manifestations of patients with pulmonary contusion appeared early and progressed rapidly. After effective treatment, they recovered quickly. Lesions began to be absorbed on CT images 2 days after injury, and most of them could be completely absorbed on 14 days after injury. It is important to be aware of the possibility of pulmonary contusion with COVID-19.
The patient was appropriately treated according to the Guidelines for the Diagnosis and Treatment of Novel Coronavirus (2019-nCoV) Infection (Trial Version 3) issued by the National Health Commission on 22 January 2020. To be specific, the patient was given a continuous supply of oxygen, LPV/r (II tab PO bid), rHu IFN-alpha 1b (500 IU injection bid), and methylprednisolone hemisuccinate (40 mg injection bid). Considering that the patient had traumatic injuries, other medicines were added to the treatment regimen, including Xuebijing and Ulinastatin. Animal experiments and clinical evidence have shown Xuebijing injection helps clear toxins in blood serum, inhibits the uncontrollable release of tumor necrosis factors (TNFs), eliminate mediators of inflammation, promote recovery of the healthy immune response, prevent an extreme inflammatory response, reduce free radicals and restore histiocytes (9). Further, studies show that Xuebijing can improve the flow of blood to alveolar capillaries (perfusion), reduce the serum levels of TNF-α and IL, prevent excessive elevation of plasma HGF and KGF-7 levels, and promote the healthy inflammatory response of the pulmonary tissue (10,11). Ulinastatin, as a protease inhibitor derived from human urine, is found to inhibit the activity of a range of enzymes, including trypsin, phospholipase A2 (PLA2), hyaluronidase (HAase) and elastase (12).
Ulinastatin has a stable lysosomal membrane that helps inhibit the release of the lysosome, eliminate free radicals, reduce mediators of inflammation, improve microcirculation, and enhance the immune system (13). On 25 January 2020, the patient’s chest CT scan showed increased pleural effusion in her thoracic cavity, associated with the injury in her chest. The administration of Xuebijing and Ulinastatin helped enhance the patient's natural defense system, prevent an excessive inflammatory response, improve microcirculation, and promote absorption of pleural fluid and relieve COVID-19.
To sum up, this report analyzes a case of COVID-19 with pleural effusion as the first symptom where the patient experienced a car accident and had traumatic injuries. COVID-19 is a novel infectious disease that requires considerable effort to design effective measures for prevention, control, and treatment. Here, the patient was diagnosed with COVID-19 after a car accident and was cured without exacerbation during the course. The patient was discharged once she met the criteria for discharge provided in the Guidelines for the Diagnosis and Treatment of Novel Coronavirus (2019-nCoV) Infection (Trial Version 4), a normal temperature lasting >3 days, resolves respiratory symptoms and two consecutively negative RT-PCR test results are at least one day apart. Although this case has its limitations in terms of the diagnosis and treatment regimen, it can still be considered a valuable experience as the medical team managed to help the patient who recently had a car accident recover from COVID-19 within 26 days without exacerbation. Hopefully, this case study may supply some insights how to diagnose and treat COVID-19.
Acknowledgments
We thank Shanghai Tongshu Biotechnology Co., Ltd. for technical support.
Funding: The study was supported by the Emergency Scientific Research Project for the Prevention and Control of the Novel Coronavirus Outbreak in Shanxi Province (Project No.: 202003D32003/GZ).
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at http://dx.doi.org/10.21037/apm-20-1720
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/apm-20-1720). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants are following the ethical standards of the institutional and national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Hui DS, I, Azhar E, Madani TA, et al. The continuing 2019-nCoV epidemic threat of novel coronaviruses to global health - The latest 2019 novel coronavirus outbreak in Wuhan, China. Int J Infect Dis 2020;91:264-6. [Crossref] [PubMed]
- Jin YH, Cai L, Cheng ZS, et al. A rapid advice guideline for the diagnosis and treatment of 2019 novel coronavirus (2019-nCoV) infected pneumonia (standard version). Mil Med Res 2020;7:4. [Crossref] [PubMed]
- Li Q, Guan X, Wu P, et al. Early Transmission Dynamics in Wuhan, China, of Novel Coronavirus-Infected Pneumonia. N Engl J Med 2020;382:1199-207. [Crossref] [PubMed]
- Wang D, Hu B, Hu C, et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA 2020;323:1061-9. [Crossref] [PubMed]
- Lu H. Drug treatment options for the 2019-new coronavirus (2019-nCoV). Biosci Trends 2020;14:69-71. [Crossref] [PubMed]
- Zeng Z, Huang XR, Lu PX, et al. Imaging manifestations and pathological analysis of severe pneumonia caused by human infected avian influenza (H7N9). Radiol Infect Dis 2015;1:64-9. [Crossref] [PubMed]
- Lin ZQ, Xu XQ, Zhang KB, et al. Chest X-ray and CT findings of early H7N9 avian influenza cases. Acta Radiol 2015;56:552-6. [Crossref] [PubMed]
- Lee N, Hui D, Wu A, et al. A major outbreak of severe acute respiratory syndrome in Hong Kong. N Engl J Med 2003;348:1986-94. [Crossref] [PubMed]
- Shi H, Hong Y, Qian J, et al. Xuebijing in the treatment of patients with sepsis. Am J Emerg Med 2017;35:285-91. [Crossref] [PubMed]
- Editorial Board of Chinese Critical Care Medicine. Xuebijing injection versus placebo for critically ill patients with severe community-acquired pneumonia: a randomized controlled trial: research results and clinical value. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue 2019;31:1199-203. [PubMed]
- Li A, Li J, Bao Y, et al. Xuebijing injection alleviates cytokine-induced inflammatory liver injury in CLP-induced septic rats through induction of suppressor of cytokine signaling 1. Exp Ther Med 2016;12:1531-6. [Crossref] [PubMed]
- Shu H, Liu K, He Q, et al. Ulinastatin, a protease inhibitor, may inhibit allogeneic blood transfusion-associated pro-inflammatory cytokines and systemic inflammatory response syndrome and improve postoperative recovery. Blood Transfus 2014;12 Suppl 1:s109-18. [PubMed]
- Sapan HB, Paturusi I, Jusuf I, et al. Pattern of cytokine (IL-6 and IL-10) level as inflammation and anti-inflammation mediator of multiple organ dysfunction syndrome (MODS) in polytrauma. Int J Burns Trauma 2016;6:37-43. [PubMed]
(English Language Editor: J. Chapnick)


