
Metabolomics study on the therapeutic effect of the Chinese herb pair Fructus Aurantii Immaturus and Rhizoma Atractylodis Macrocephalae in constipated rats based on UPLC-Q/TOF-MS analysis
Introduction
Constipation is a widespread functional gastrointestinal disorder among humans in modern society and seriously influences people’s health and quality of life (1,2). According to the current pathophysiology mechanism, constipation caused by functional diseases can be divided into various types, such as defecatory disorder, mixed constipation, normal transit constipation and slow transit constipation (STC) (3). Among them, STC is the most usual type of chronic constipation and is characterized by slow proximal colonic transit and obviously increased total bowel transit time (4). According to previous study, several reasons may cause STC, including structures, machinery, metabolism, or functional factors (5). Despite its high morbidity, the precise pathogenesis of STC remains unknown (6,7).
In China, Zhishi (Aurantii Fructus Immaturus) and Baizhu (Atractylodis Macrocephalae Rhizoma) are a traditional herb pair utilized to regulate qi, harmonize the stomach, promote digestion, resolve lumps and release distension which was first described by the renowned Chinese physician Zhang Zhongjing (150–219 A.D. in the Eastern Han Dynasty) in Essentials from the Golden Cabinet (Jin Gui Yao Lue), a medical classic. This herb pair combination therapy was widely used to treat gastrointestinal motility disorders for thousands of years, especially showing a definite advantage in the treatment of STC. Previous clinical studies have shown that the Zhishi-Baizhu (ZSBZ) herb pair can effectively enhance gastrointestinal motility, increase the frequency of bowel movements, shorten the transit time of the colon, reduce the symptoms and physical signs of constipation patients, improve the anorectal dynamics index, and improve the living quality of patients (8). However, because its clinical effect is the result of various components targeting multiple metabolic pathways, the mechanism of ZSBZ in the treatment of STC remains unclear.
Metabolomics, a branch of systems biology, is a holistic analytical method for characterizing small molecular endogenous metabolites in various biological samples (9). In recent years, metabolomics has been widely used in TCM research, including the compatibility mechanism exploration of active constituents in Chinese medicine (CM), processing mechanism of CM and toxicity mechanism of CM, because its research mode is similar to the mechanism of TCM and it provides a new paradigm to discover the complicated mechanisms in TCM (10). Ultra-performance liquid chromatography equipped with electrospray ionization quadrupole time-of-flight mass spectrometry detection (UPLC-Q/TOF-MS) combined with multivariate statistical analysis is the most common method in metabolomics research due to the extensive availability of the technology and compatibility with the extensive separation of biological samples (11-13). In this study, plasma metabolomics combined with metabolic pathway analysis has been used to elucidate the therapeutic mechanism of ZSBZ in STC from a metabolic perspective.
We present the following article in accordance with the ARRIVE reporting checklist (available at http://dx.doi.org/10.21037/apm-20-280).
Methods
Chemicals and reagents
The HPLC grade methanol, MS grade acetonitrile and formic acid were purchased from Merck (Darmstadt, Germany). Pure water was obtained from Jilin Wahaha Food Co. Ltd. (Jilin, China). Ultrapure water was prepared from a Milli-Q water purification system (Millipore, Bedford, MA, USA). Loperamide Capsules were from Xian Janssen Pharmaceutical Ltd. Mosapride Citrate Capsules were from Jiangsu Hengrui Pharmaceutical Co., Ltd. Chloral hydrate was obtained from China National Pharmaceutical Group Co., Ltd. Rabbit monoclonal antibody against MLCK was supplied by Sigma (USA). Acacia gum was purchased from Guangzhou Nanfang Chemical Glass Co., Ltd. Activated carbon was from Hangzhou Wood General Factory. The super centrifuge was from Eppendorf (Germany). The microplate reader was from Thermo Fisher Scientific (USA). An Olympus light microscope was employed (BX41, Japan). The slicer was the RM 2235 from Leica Instruments (Germany). The electric constant temperature air blower dryer was from Shanghai Botai Experimental Equipment Co., Ltd.
Sample preparation
Zhishi (Lot: 170910) was purchased from Suzhou Tianling Traditional Chinese Medicine Decoction Pieces Co., Ltd. (Suzhou, China). Baizhu (Lot: 17C821) was obtained from Suzhou Boyuan Pharmaceutical Co., Ltd. (Suzhou, China). The aqueous extract of ZSBZ was prepared as follows: 2 kg of Zhishi and 1 kg Baizhu were mixed with 10 times the amount of distilled water and soaked for 0.5 h. Second, the mixture was boiled with mild heat for 40 min and afterwards filtered through 4 layers of carbasus. This method was repeated to extract the residue with 6 times the amount of distilled water. Afterwards, two aqueous extracts were merged and vacuum-concentrated to 1 g/mL of crude drug by a rotary evaporator. The samples were stored at 4 °C for future use.
Animal study design and induction of constipation
The study was approved by ethics board of Suzhou TCM Hospital Affiliated to Nanjing University of Chinese Medicine (NO. 2018-03-216), in compliance with national and institutional guidelines for the care and use of animals. Forty healthy, specific pathogen-free (SPF), 5-week-old, male Sprague-Dawley rats (170–180 g) were purchased from the Jiangsu Laboratory Animal Centre in Suzhou, China [license approval number: SCXK (Su) 2017-0007]. All rats were maintained in an animal house (SPF degree) with a barrier system assisted with a clean laminar flow chamber in the Experimental Animal Center of Nanjing University of Chinese Medicine and used for experimentation after 1 week. Feeding environment parameters were as follows: room temperature, 26 °C; relative humidity, 45–55%; light condition, 12 h light/dark cycles; noise level, <60 dB; clean and quiet, well-ventilated. All experimental operations in this study were carried out in accordance with the Provision and General Recommendation of the Chinese Laboratory Association. The protocol was approved by the Medical Research Committee on Animal Care and Use, Nanjing University of Chinese Medicine. Animals were randomly divided into four groups: control group, Lop group, mosapride group and ZSBZ group (ZSBZ water extract). Except for the control group, the other three groups were induced as the STC models by oral administration of 3 mg/kg loperamide suspension twice per day (09:00 and 17:00) for 14 days, while the control group rats were administered normal saline only (14). ZSBZ group rats were intragastric administered ZSBZ water extract (81 mg/kg) twice a day for 14 days. Mosapride group rats were intragastric administered with 1.58 mg/kg mosapride suspension twice per day for 14 days. On day 14, all rats were intraperitoneally injected with 3% chloral hydrate 0.5 h after the last portion. Blood samples were collected by the abdominal aortic method.
Analysis of body weight, feeding conditions and fecal excretion
The body weight, food intake, and water consumption of rats in each group was measured daily during the experimental period. We collected fecal pellets from individual rats 24 h after the treatment administration. The total number, wet weight, and water content of the fecal pellets were detected. All measurements were performed in triplicate to ensure accuracy.
Measurement of intestinal transit ratio
On day 14, all rats were fasted for 12 h and allowed free access to water, then fed charcoal in 10% acacia gum. After 0.5 h, the rats’ abdomens were opened and the intestines were removed from the pylorus to the ileocecal junction. The total length of the truncated intestine and the charcoal transport distance were measured, and then the intestinal motility rate was calculated by the following formula: charcoal transit ratio (%) = distance traversed by the charcoal (cm)/total length of small intestine (cm) × 100%.
Histological observation
The experimental rats were euthanized and sacrificed, and the transverse colons were removed and cut into 8- to 10-mm sections. The transverse colons were gently shaken in PBS to remove the contents of the intestine, then fixed with 10% neutral-buffered formalin for more than 24 h. After fixation, the tissues were embedded in paraffin, and embedded tissues were cut into 5-µm thick sections. All of the sections were then stained with hematoxylin-eosin (H&E). The colon tissue was then embedded, sectioned, and HE stained. The thickness of the transverse colonic mucosa and the morphology of the cells in the colon were observed under binocular light microscopy (Carl Zeiss, Germany).
Measurement of neurotransmitter serum concentration
First, 5–10 mL of blood from the abdominal aorta was injected into the EDTA anticoagulant tube. Next, 2 mL of serum was separated by centrifugation (3,000 r/min, 10 min), and the motilin (MTL) and substance P (SP) indexes were detected by commercial ELISA kits (Biolegend, San Diego, USA). The procedure was conducted strictly in accordance with the kit instructions.
Determination of ATP in jejunal tissue by colorimetry
A 0.5 cm × 0.5 cm section of rat jejunal tissue was taken and washed with physiological saline. The ATP content of rat jejunal epithelial cells were determined by a colorimetric method according to the kit instructions.
Immunohistochemistry
Myosin light chain kinase (MLCK) expression level was analyzed by immunohistochemistry. Rat paraffin colon sections were routinely fixed with 4% paraformaldehyde for 10 min: after rinsing 3 times (3 min/time) by phosphate buffered saline, 50 µL of peroxidase blocking solution was added dropwise and incubated for 10 min at room temperature. Slides were then incubated with anti-MLCK primary antibody (Proteintech, IL, USA) overnight at 4 °C, followed by HRP-conjugated anti-rabbit IgG incubation at room temperature for 30 min, and diaminobenzidine (DAB) was used for staining. Image-Pro Plus 6 graphic processing software analysis and high-power microscopy (×200) observed the expression of MLCK per unit area of colon tissue, and 5 fields of each section were randomly observed. The respective optical density values of MLCK expression in each group of rats were statistically determined.
Plasma sample preparation for UPLC-Q/TOF-MS analysis
The rat plasma samples stored in the freezer at −80 °C were thawed at 4 °C. Each 200 µL plasma sample was treated with 8 volumes of methanol (chromatography grade). The samples were mixed by vortex for 30 s. Then, the mixture was centrifuged at 12,000 r/min at 4 °C for 10 min. The supernatant was absorbed with a 1 mL disposable syringe and passed through the 0.22 µm microporous filter membrane, which was the spare sample for further UPLC-Q/TOF-MS analysis. The quality control (QC) sample was prepared by mixing 10 µL of each spare sample to be tested.
Mass spectrum analysis and verification of methodology
To guarantee system repeatability and stability, QC samples were used for method validation. The QC specimen was continuously analyzed 6 times. Chromatographic separation was performed on a Shimadzu UPLC system (Kyoto, Japan) combined with an LC-30AD binary liquid pump, SIL-30SD autosampler, DGU-20A5R on-line solvent degasser, CTO-30A column oven, AB SCIEX Triple TOF 5600+ system, and ESI source. An Agilent C18 reversed-phase column (2.1×100 mm, 1.8 µm, Palo Alto, CA, USA) was applied for all analyses at 35 °C. The mobile phase was composed of 0.1% formic acid aqueous solution (solvent A, Merck, USA) and acetonitrile (solvent B, Merck, USA) at a flow rate of 0.3 mL/min. The injection volume was set as 1 µL. The solvent gradient was as follows: 0–3 min, 5–60% B; 3–12 min, 60–65% B; 12–13 min, 65–95% B; 13–15 min, 95-5% B. Mass spectrometry experiments were conducted using the Q-TOF MS system equipped with an electrospray ionization (ESI) source in both positive and negative modes. Specific conditions were as follows: ion spray voltage, +4,500/−4,500; source temperature, 550 °C; desolvation gas flow rate, 50 mL/min; collision energy, +35/−35 eV; and decluster voltage, +60/−60 V. All reagents were of HPLC grade.
Data processing and statistical analysis
For metabolomics data processing, raw data files were identified and extracted, graded and corrected by Analyst TF 1.6 software (AB SCIEX, Boston, MA, USA). Raw mass spectrometric data were preliminarily managed by Marker View 1.2.1 (AB SCIEX, Boston, MA, USA), the peak area of the chromatographic peak of the compound was standardized by MetaboAnalyst 4.0 software, and the compounds with significant differences were screened out (P<0.05 and multiple change P<0.05). The resulting data matrices were then introduced into SIMCA (version 14.1, Umetrics, Sweden) for principal component analysis (PCA), and partial least square discriminant analysis (PLS-DA). Orthogonal Projections to Latent Structures Discriminant Analysis (OPLS-DA) was engaged to filter endogenous biomarkers between different groups (15). MassLynx (Waters Technologies, United States) combined with the HMDB database identified the potential biomarkers. Variable importance in projection (VIP) represents the contribution degree of variables in different groups (16). Those with the VIP value >1.0 and P value <0.05 among the three groups were estimated by t-test or the Mann-Whitney U test. One-way analysis of variance (ANOVA) was engaged by Prism software (GraphPad Software 8.0, San Diego, CA, USA) for assessment of the related pharmacological indicators. The results were considered significant with P<0.05.
Results
Effect of ZSBZ on feeding behavior and fecal excretion of loperamide-induced constipation rats
To investigate whether treatment with the mixture of ZS and BZ could affect body weight, feeding behavior and fecal excretion in constipated rats, changes in body weight, food intake, water consumption, fecal water content and stool number were measured during the experimental period. As shown in Figure 1, body weight steadily increased in all groups (Figure 1A). However, no significant differences in body weight, food intake and water consumption were observed among any groups after administration of loperamide, mosapride and the ZS and BZ mixture (Figure 1A,B,C). Fecal water content was significantly decreased after treatment with loperamide compared with that in the control group (P<0.01). Otherwise, the ZS and BZ mixture treatment increased the fecal water content compared with the Lop treatment (Figure 1D). Moreover, rats with constipation exhibited a decreased stool number, while those in the mosapride- and ZS and BZ mixture-treated groups showed improved differences (Figure 1E). Collectively, these results indicate that the ZS and BZ mixture treatment did not induce any alteration of body weight or feeding behavior and exerted effects on fecal water content and stool number.
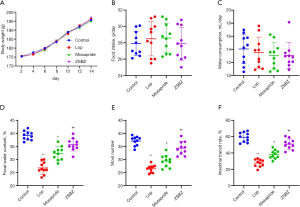
Effect of ZSBZ treatment on gastrointestinal motility
As shown in Figure 1F, significant decreases in the intestinal transit ratio of charcoal were observed in the Lop group compared with the control group. After 2 weeks, the intestinal transit rate in the ZS and BZ mixture group was significantly higher than that in the Lop group and lower than that in the control group. Similar results were found for mosapride treatment.
Histological alteration of colon
To investigate the effect of the ZSBZ herb pair on structural alteration of the colon tissue, the smooth muscle cell, neuronal cell, and mucous layer in the colon were detected by H&E staining. In the Lop group, the colonic smooth muscle cells of the rats were atrophied and arranged in a disorderly fashion, the neuronal cells in the colon tissue were reduced, and the inflammatory cells infiltrated the mucosa. However, the colonic smooth muscle cells and neuronal cells of the ZSBZ group gradually recovered to the same level as those in the control group, and the infiltration of inflammatory cells in the colon tissue was reduced (Figure 2).
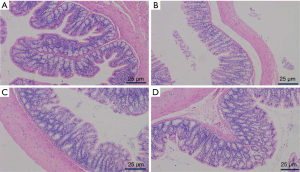
Effects of ZSBZ on serum motilin (MTL), substance P (SP) and adenosine triphosphate (ATP) in rats
The effects of ZSBZ on relieving constipation were further evaluated by measuring serum neurotransmitters (MTL and SP) and ATP in jejunal tissue. As shown in Figure 3, the levels of MTL, SP and ATP were significantly lower in constipated rats than in control rats (P<0.05). In comparison to the Lop group, the ZSBZ group showed significant increases in the levels of MTL, SP and ATP (P<0.01). These results demonstrate that ZS and BZ mixture treatment effectively increased the levels of the excitatory neurotransmitters (MTL and SP) and adenosine triphosphate to speed the motility of the gastrointestinal tract.

Effect on MLCK expression in colon tissues in rats
It can be observed in Figure 4 that brownish yellow granules in the cytoplasm of smooth muscle cells were found in the mucosa, submucosa and muscular layer of colon tissue of rats in each group, and brownish yellow granules with different shades and densities can be seen. Compared with that in the control group, the cytoplasmic staining of the smooth muscle cells in the muscular layer of the colon of the Lop group was light yellow, and the optical density of MLCK was significantly reduced (P<0.01). Compared with that in the Lop group, the optical density of MLCK in the ZSBZ group was significantly increased (P<0.05).
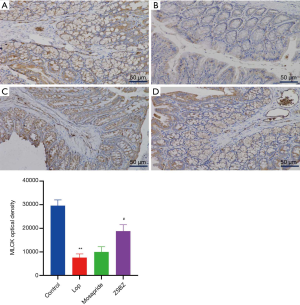
Visual inspection of QC overlapping total ion chromatography
The overlapping total ion chromatograms (TIC) are presented in Figure 5A,B. In the common modes of positive and negative ions, the QC samples gather near the middle of the projection of the score matrix, and the significantly overlapping chromatogram indicated that the UPLC-Q/TOF-MS system was repeatable and stable throughout the entire analysis process.
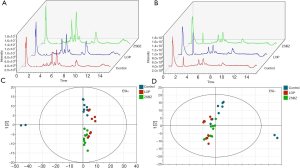
Multivariate statistical analysis of UPLC-Q/TOF-MS
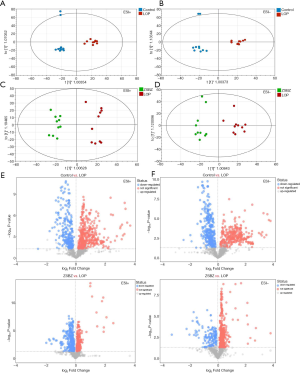
The UPLC-Q/TOF-MS data were analyzed using PCA to determine the differences between the principal components of the control group, Lop group and ZSBZ group. PCA score plots are shown in Figure 5C,D. The PCA model was estimated by cross-validation in the positive mode (R2X=0.685, Q2=0.534) and in the negative mode (R2X=0.698 and Q2=0.468), respectively. Orthogonal projections to latent structures discriminant analysis (OPLS-DA) was applied to screen the potential markers formed by the metabolic differences among the groups. Figure 6A,B,C,D shows a certain extent of separation tendency among the control, Lop and ZSBZ groups, indicating that the physiological and metabolic environments of metabolites in the plasma of constipated rats were changed after ZSBZ treatment. Since the values of both R2X and Q2 approach 1.0 (Table 1), we conclude that the accuracy and predictive capability of the models were excellent.
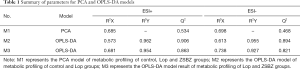
Full table
Identification of the different metabolites in the plasma samples among different groups
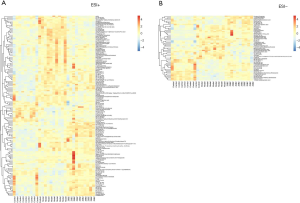
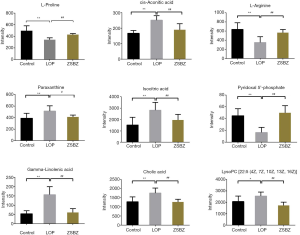
Based on the establishment of the OPLS-DA model, the differences among variables between control group and Lop group, and Lop group and ZSBZ group, were screened by volcano plot analysis index (Figure 6E,F,G,H). The complete data set was imported into MetaboAnalyst 4.0 to generate a heatmap to identify group differences (Figure 7). According to the variable projection importance index (VIP) of each OPLS-DA model, the VIP value was positively correlated with the grouping contribution rate. The variables (m/z-Rt pairs) that contributed to the distinction were filtered according to variable importance in projection (VIP) value >1.0 of the OPLS-DA model and t-test P value <0.05. The secondary mass spectra of different substances were extracted by PeakView software provided by AB SCIEX company, then compared with the standard secondary mass spectrometry data from MassBank, Chemspider, HMDB, METLIN and other compound databases and related literature. Finally, 9 differential metabolites of each group, including L-proline, cis-aconitic acid, L-arginine, paraxanthine, isocitric acid, pyridoxal 5’-phosphate, gamma-linolenic acid, cholic acid and LysoPC [22:5 (4Z, 7Z, 10Z, 13Z, 16Z)], were identified by comprehensive analysis: the results are shown in Table 2. Furthermore, the relative contents of 9 differential metabolites in rats in each group were tested by nonpaired t-test, and the results are shown in Figure 8. The results showed that the administration of ZSBZ could significantly improve the abnormal changes in 9 differential metabolites in the Lop group.
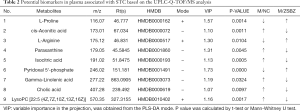
Full table
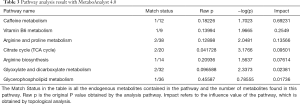
Metabolomics pathway analysis
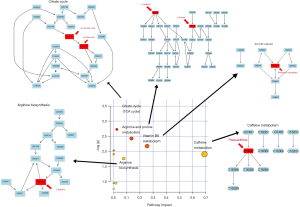
We input the above identified endogenous differential metabolites into the MetaboAnalyst4.0 metabonomics online analysis platform (https://www.metaboanalyst.ca/faces/home.xhtml), selected the Rattus norvegicus (rat) pathway library as the metabolic pathway database, set the hypergeometric test as pathway enrichment analysis, with relative-betweenness centrality pathway analysis topology, carried out pathway enrichment, and screened out metabolic pathways with a metabolic pathway influence value (Impact) greater than 0.10 (Table 3). Plots were described by pathway impact scores (x-axis) and P values (y-axis). The values of pathway impact and –logP were larger, the correlation of the metabolic differences between different groups was higher, and the circle in Figure 9 became larger and redder. Plots were described by pathway impact scores (x-axis) and P values (y-axis). In this study, the pathway impact-value was set to 0.10 according to reference (17). The results of pathway analysis are shown in Figure 9. The results showed that the main metabolic pathways involving differential metabolites in plasma samples of each group included caffeine metabolism, vitamin B6 metabolism, arginine and proline metabolism and the citrate cycle (TCA cycle). It is suggested that the metabolic abnormality of rats with slow transit constipation and the therapeutic effects of Fructus Aurantii and Atractylodes macrocephala on slow transit constipation are closely related to the above metabolic pathways.
Full table
Discussion
In this study, a UPLC-Q/TOF-MS-based metabolomics approach was implemented to explore the potential mechanisms of ZSBZ in the treatment of constipation. The method used in this experiment is not to extract a single chemical component but to highlight the integrity of Chinese medicine, which is more in line with the synergistic mechanism of Chinese medicine compound prescription as a whole. We found that ZSBZ treatment decreased the intestinal propulsion rate in constipated rats. To support our result, previous findings have shown that ZSBZ improved the intestinal motility in constipated rats by using the charcoal transit ratio (18).
MTL is a very important gastrointestinal hormone that can promote gastrointestinal motility and enhance gastrointestinal contractility and tension (19). SP is a neurotransmitter that has the function of stimulating gastrointestinal motility, is widely distributed throughout the entire gastrointestinal tract and intestinal nervous system, and can stimulate the contraction of almost all digestive tract smooth muscle (20). Both of them can effectively reflect the changes in gastrointestinal function.
After treatment with ZSBZ, the colonic motility disorder and the expression of related gastrointestinal hormones in STC rats were significantly improved. The results show that ZSBZ may regulate two aspects of gastrointestinal function: the gastrointestinal-neuromuscular regulation system and gastrointestinal hormones.
Intestinal movement and nutrition absorption are closely related to adenosine triphosphate (ATP). ATP is the most basic carrier of energy for conversion in organisms, and the change in ATP content is directly related to the energy metabolism of various organs (21). As the most important energy molecule, ATP plays important roles in various physiological and pathological processes of cells. The results showed that the colonic motor function of STC rats decreased significantly, which led to the decrease in ATP production. After the treatment with ZSBZ, the colonic motor function of STC model rats was significantly enhanced, which was reflected in the significant increase in ATP content.
Studies have shown that smooth muscle contraction plays an important role in regulating the changes in gastrointestinal motility, and the decrease in contractility will lead to the decrease in intestinal peristalsis, which in turn leads to constipation (22).
MLCK is the key protein for smooth muscle contraction: when smooth muscle cells are stimulated by electrical signals, endoplasmic reticulum and extracellular calcium ions are released into the cytoplasm, intracellular calcium concentration increases, and Ca2+ forms a complex with CaM, which further activates MLCK to further phosphorylate myosin light chain (MLC), thus causing myosin and actin to slide relative to each other, and ultimately causing smooth muscle cells to contract (23). Immunohistochemical analysis demonstrated that the expression of MLCK in colonic smooth muscle cells of STC rats was significantly lower than that of normal rats, while ZSBZ could significantly increase the expression of MLCK in colonic smooth muscle cells of STC rats, suggesting that the regulation of the signal transduction mechanism of Ca2+-CaM-MLCK in colonic smooth muscle cells may be one of the most important mechanisms of ZSBZ with respect to the regulation of colonic motility.
Metabonomic results showed that slow transit constipation could lead to an abnormal increase in p-xanthine, which could be decreased after administration of ZSBZ. Paraxanthine is a very weak polar compound which participates in a variety of enzymatic reactions in vivo: in particular, p-xanthine and formaldehyde can be biosynthesized from caffeine, which is catalyzed by the cytochrome P450 1A2 enzyme. In addition, paraxanthine and acetyl-CoA can be converted into 5-acetylamino-6-formylamino-3-methyluracil through interaction with the arylamine N-acetyltransferase 2 enzyme. In humans, paraxanthine is involved in caffeine metabolism. The effect of p-xanthine on constipation has not been reported. Studies on caffeine and colorectal cancer are more common. Some studies have shown that caffeine can reduce the inflammatory process by changing the balance between proinflammatory and anti-inflammatory cytokines, thus inhibiting the progression of colorectal cancer (24).
Pyridoxal 5’-phosphate participates in vitamin B6 metabolism. Studies have shown that abnormal levels of vitamin B6 are closely related to constipation (25). In addition, vitamin B6 is involved in the formation of serotonin, which increases the concentration of serotonin. In addition, vitamin B6, as a coenzyme, is involved in various metabolic reactions, such as those of amino acids and proteins. Lack of vitamin B6 can cause protein hydrolysis to stagnate and result in conversion into fat, which prevents growth. Administration of ZSBZ can increase the content of pyridoxal 5’-phosphate, thus increasing the synthesis of vitamin B6, increasing the content of serotonin and promoting the metabolism of protein (26).
Cis-aconitic acid and isocitric acid participate in the tricarboxylic acid cycle. The tricarboxylic acid cycle is a common metabolic pathway for three major classes of nutrients (sugars, lipids and amino acids) in the human body and other aerobic organisms. In the tricarboxylic acid cycle, isocitrate can be catalyzed by isocitrate dehydrogenase, which is irreversible and is also the rate-limiting step in the tricarboxylic acid cycle (27). Compared with the model group, ZSBZ significantly decreased the contents of cis-aconitic acid and isocitric acid in the blood of rats, indicating that ZSBZ may promote tricarboxylic acid circulation, which is conducive to the processes of glycolysis and fat mobilization, so that it can quickly provide a portion of the energy for the contraction of large intestinal smooth muscle and promote the movement of the large intestine. Therefore, regulating tricarboxylic acid cycle metabolism is probably associated with the therapeutic effect of ZSBZ in constipation. Additionally, evidence has indicated that the tricarboxylic acid cycle was involved in the abnormal metabolism of colitis (28).
L-Arginine and L-proline participate in the metabolic pathways of proline and arginine. L-arginine (Arg) is a semiessential amino acid with many physiological functions. Studies have shown that arginine and its downstream metabolite proline can increase the diversity of intestinal flora in mice, thus fulfilling a protective role in intestinal inflammation (29). In this study, levels of L-arginine and L-proline were remarkably upregulated after ZSBZ treatment in constipated rats, making L-arginine and L-proline possible targets for the treatment of constipation. In addition to the above metabolic pathways, the ameliorative effect of ZSBZ on slow transit constipation is also related to arginine biosynthesis, glyoxylate and dicarboxylate metabolism and glycerophospholipid metabolism. These findings further indicate that the metabolic markers could be considered potential candidates for the treatment of constipation, although more clinical samples and pharmacological experiments are required to confirm the mechanism of ZSBZ.
Conclusions
In conclusion, we demonstrated that ZSBZ treatment exhibited a motivating effect on loperamide-induced constipation in rats, the effects of which might be due to the regulation of caffeine and vitamin B6 metabolism. A major challenge for the future is characterizing the individual functions of the altered metabolites circulating in blood to elucidate the underlying mechanisms of ZSBZ on constipation. Based on these metabolomics results, we are able to obtain a broad understanding of the therapeutic effects of ZSBZ. Therefore, the present study will provide additional insight into clinical applications and pharmacological research, as well as the identification of metabolites of ZSBZ in the treatment of constipation patients.
Acknowledgments
Funding: Supported by China Postdoctoral Science Foundation (2017M620220), the technology project of Jiangsu Provincial Administration of Traditional Chinese Medicine (YB2017061), Scientific Foundation of Integrated traditional Chinese and Western Medicine of Suzhou (SYSD2018212), Young Elite Scientists Sponsorship Program by China Association of Chinese Medicine (CACM-2018-QNRC2-C13), the Open Project Program of Jiangsu Key Laboratory for Pharmacology and Safety Evaluation of Chinese Materia Medica (No. JKLPSE201819), the Project of the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD), the fifth batch of Gusu health personnel training project in Suzhou (GSWS2019065) and Suzhou Science and Technology Development Plan people's livelihood Science and Technology - Research on the Application of key Technologies (SS2019073).
Footnote
Reporting Checklist: The authors have completed the ARRIVE reporting checklist. Available at http://dx.doi.org/10.21037/apm-20-280
Data Sharing Statement: Available at http://dx.doi.org/10.21037/apm-20-280
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/apm-20-280). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was approved by ethics board of Suzhou TCM Hospital Affiliated to Nanjing University of Chinese Medicine (NO.2018-03-216) in compliance with national and institutional guidelines for the care and use of animals.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the noncommercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Polymeros D, Beintaris I, Gaglia A, et al. Partially hydrolyzed guar gum accelerates colonic transit time and improves symptoms in adults with chronic constipation. Dig Dis Sci 2014;59:2207-14. [Crossref] [PubMed]
- Leung L, Riutta T, Kotecha J, et al. Chronic constipation: an evidence-based review. J Am Board Fam Med 2011;24:436-51. [Crossref] [PubMed]
- Shahid S, Ramzan Z, Maurer AH, et al. Chronic idiopathic constipation: more than a simple colonic transit disorder. J Clin Gastroenterol 2012;46:150-4. [Crossref] [PubMed]
- Chen Z, Lin S, Jiang Y, et al. Effects of Bread Yeast Cell Wall Beta-Glucans on Mice with Loperamide-Induced Constipation. J Med Food 2019;22:1009-21. [Crossref] [PubMed]
- Ouyang A, Locke GR. Overview of neurogastroenterology-gastrointestinal motility and functional GI disorders: Classification, prevalence, and epidemiology. Gastroenterol Clin North Am 2007;36:485-98. [Crossref] [PubMed]
- Bharucha AE, Wald A. Chronic Constipation. Mayo Clin Proc 2019;94:2340-57. [Crossref] [PubMed]
- Emmanuel A, Cools M, Vandeplassche L, et al. Prucalopride improves bowel function and colonic transit time in patients with chronic constipation: an integrated analysis. Am J Gastroenterol 2014;109:887-94. [Crossref] [PubMed]
- Wang C, Ren Q, Chen XT, et al. System Pharmacology-Based Strategy to Decode the Synergistic Mechanism of Zhi-zhu Wan for Functional Dyspepsia. Front Pharmacol 2018;9:841. [Crossref] [PubMed]
- Zhang X, Li P, Hua Y, et al. Urinary metabolomics study the mechanism of Taohong Siwu Decoction intervention in acute blood stasis model rats based on liquid chromatography coupled to quadrupole time-of-flight mass spectrometry. J Chromatogr B Analyt Technol Biomed Life Sci 2018;1074-1075:51-60. [Crossref] [PubMed]
- Zhuang Y, Qin K, Yu B, et al. A metabolomics research based on UHPLC-ESI-Q-TOF-MS coupled with metabolic pathway analysis: Treatment effects of stir-frying Xanthii Fructus on allergic rhinitis in mice model. Biomed Chromatogr 2018;32:e4352. [Crossref] [PubMed]
- Liu K, Song Y, Liu Y, et al. An integrated strategy using UPLC-QTOF-MSE and UPLC-QTOF-MRM (enhanced target) for pharmacokinetics study of wine processed Schisandra Chinensis fructus in rats. J Pharm Biomed Anal 2017;139:165-78. [Crossref] [PubMed]
- Song Y, Su D, Lu T, et al. Differential pharmacokinetics and the brain distribution of morphine and ephedrine constitutional isomers in rats after oral administration with Keke capsule using rapid-resolution LC-MS/MS. J Sep Sci 2014;37:352-9. [Crossref] [PubMed]
- Su D, Li W, Xu Q, et al. New metabolites of acteoside identified by ultra-performance liquid chromatography/quadrupole-time-of-flight MS(E) in rat plasma, urine, and feces. Fitoterapia 2016;112:45-55. [Crossref] [PubMed]
- Jabri MA, Wannes D, Hajji N, et al. Role of laxative and antioxidant properties of Malva sylvestris leaves in constipation treatment. Biomed Pharmacother 2017;89:29-35. [Crossref] [PubMed]
- Worley B, Powers R. PCA as a practical indicator of OPLS-DA model reliability. Curr Metabolomics 2016;4:97-103. [Crossref] [PubMed]
- Wan JB, Bai X, Cai XJ, et al. Chemical differentiation of Da-Cheng-Qi-Tang, a Chinese medicine formula, prepared by traditional and modern decoction methods using UPLC/Q-TOFMS-based metabolomics approach. J Pharm Biomed Anal 2013;83:34-42. [Crossref] [PubMed]
- Ma N, Karam I, Liu XW, et al. UPLC-Q-TOF/MS-based urine and plasma metabonomics study on the ameliorative effects of aspirin eugenol ester in hyperlipidemia rats. Toxicol Appl Pharmacol 2017;332:40-51. [Crossref] [PubMed]
- Gong YX, Wang H, Hou Y, et al. Effects of High-dose Raw Rhizoma Atractylodis Macrocephala Combined with Fructus Aurantii Immaturus on the Expression of 5-HT3R and 5-HT4R in Colon of Rats with Slow Transit Constipation. Chin J Integr Tradit West Med (Chin) 2019;39:988-92.
- Deloose E, Verbeure W, Depoortere I, et al. Motilin: from gastric motility stimulation to hunger signalling. Nat Rev Endocrinol 2019;15:238-50. [Crossref] [PubMed]
- Meng XM, Liu XT. Effect of application of herbal medicine paste to "Tianshu" (ST25) on intestinal mobility and expression of vasoactive intestinal peptide and substance P in colonic myenteric plexus in rats with functional constipation. Zhen Ci Yan Jiu 2019;44:906-10. [PubMed]
- El Moussawi L, Chakkour M, Kreydiyyeh SI. Epinephrine modulates Na+/K+ ATPase activity in Caco-2 cells via Src, p38MAPK, ERK and PGE2. PLoS One 2018;13:e0193139. [Crossref] [PubMed]
- Graham HK, Maina I, Goldstein AM, et al. Intestinal smooth muscle is required for patterning the enteric nervous system. J Anat 2017;230:567-74. [Crossref] [PubMed]
- Yu T, Wang Y, Qian D, et al. Advanced Glycation End Products Impair Ca2+ Mobilization and Sensitization in Colonic Smooth Muscle Cells via the CAMP/PKA Pathway. Cell Physiol Biochem 2017;43:1571-87. [Crossref] [PubMed]
- Bessler H, Salman H, Bergman M, et al. Caffeine alters cytokine secretion by PBMC induced by colon cancer cells. Cancer Invest 2012;30:87-91. [Crossref] [PubMed]
- Sturtzel B, Dietrich A, Wagner KH, et al. The status of vitamins B6, B12, folate, and of homocysteine in geriatric home residents receiving laxatives or dietary fiber. J Nutr Health Aging 2010;14:219-23. [Crossref] [PubMed]
- Zhao XY, Wang JW, Yin Y, et al. Effect of Tong Xie Yao Fang on endogenous metabolites in urine of irritable bowel syndrome model rats. World J Gastroenterol 2019;25:5134-51. [Crossref] [PubMed]
- Chen YF, Yu XJ, Liu XH, et al. Discussion on Biological Basis of Constipated Mice Cured by Optimal Prescription of Da Chengqitang with Differential Proteomics. Chin J Exp Med Formul 2017;23:93-9.
- Gu X, Song Y, Chai Y, et al. GC-MS metabolomics on PPARα-dependent exacerbation of colitis. Mol Biosyst 2015;11:1329-37. [Crossref] [PubMed]
- Singh K, Gobert AP, Coburn LA, et al. Dietary Arginine Regulates Severity of Experimental Colitis and Affects the Colonic Microbiome. Front Cell Infect Microbiol 2019;9:66. [Crossref] [PubMed]


