
Variations in vital signs at the end of life in non-cancer patients: a retrospective study
Introduction
End-of-life care, particularly within 3 days of death, is important for patients and their families (1,2). The findings of a nationwide survey of the bereaved families of terminal cancer patients in palliative care units in Japan revealed that more than 90% of family members wanted to be present at the moment of death (3). Furthermore, previous studies suggested that care in the dying phase may affect the psychological prognosis of bereaved families (4,5). Medical professionals have to make many important decisions for patients and their families in the last days of life, including the discontinuation of invasive treatments and informing family members and close friends in time (6,7).
A detailed understanding of the clinical course of non-cancer patients in the dying phase is critical for the provision of appropriate care in the last days of life (7). A number of symptoms, signs, and changes in vital signs occur in the last three days of life of cancer patients (8), based on which many prognostic models have been developed (9,10). Routine measurements of vital signs are conducted in daily clinical settings, and previous studies reported changes in these signs in cancer patients immediately before death (11-15). Although non-cancer patients appear to have a similar clinical course in the last days of life as advanced cancer patients, there is currently no information on changes in the vital signs of non-cancer patients before death. If similar changes in vital signs in last days of life occur in non-cancer patients and terminal cancer patients, the same indicators of prognosis used for cancer patients in the dying phase may be applied to non-cancer patients.
Therefore, the present study was performed to clarify changes in vital signs before impending death in non-cancer patients, and was conducted in accordance with the STROBE reporting checklist (available at http://dx.doi.org/10.21037/apm-20-1054) (14-16).
Method
Study design and participants
The present study involved a secondary analysis of a retrospective study performed to examine survival times following marked decreases in oral intake by non-cancer patients in the dying phase (17). The main retrospective study was a medical chart review of non-cancer patients admitted to the General Medicine Ward of Kamisu Saiseikai Hospital, Ibaraki, Japan. This hospital is a regional core hospital in a medical area serving approximately 250,000 people, and hospitalized patients are mainly acutely ill due to various diseases. We included patients who were older than 20 years and had died between April 2017 and April 2018. Patients diagnosed with cancer, those receiving enteral or parenteral nutrition, or those on a ventilator during hospitalization were excluded. Patients who died within three days of admission were also excluded because they did not meet the purpose of the present study. The need for informed consent from family members was waived by the Institutional Review Board of Kamisu Saiseikai Hospital because this study only involved a retrospective chart review. Information on the study content was presented on a notice board in the hospital before its initiation. The present study was conducted with the approval of the Institutional Review Board of Kamisu Saiseikai Hospital (No. 18-0001), and all procedures were performed in accordance with the Declaration of Helsinki (as revised 2013). The need for informed consent from family members was waived by the Institutional Review Board of Kamisu Saiseikai Hospital because this study only involved a retrospective chart review. Information on the study content was presented on a notice board in the hospital before its initiation. Study outcomes will not affect the future management of patients.
Data collection
The baseline characteristics of age, sex, diagnosis on admission, and the presence of comorbidities categorized by the Charlson Comorbidity Index (CCI) (18) were recorded for all study patients. Vital signs were collected from medical records for up to seven days before the date of death, and included systolic and diastolic blood pressure, heart rate, body temperature, and oxygen saturation (patients received supplemental oxygen depending on their conditions), which were routinely documented at this hospital. Vital signs were measured at least twice daily, and data collected at approximately 9 a.m. and 9 p.m. were used in analyses.
Statistical analysis
Descriptive statistics were used to summarize baseline characteristics. The average value of each vital sign approximately every 12 hours until death was plotted to show the changes that occurred in the last seven days. Data were divided into two periods: from day −7 to day −4 and from day −3 to death. We used a linear mixed model in the two periods, with time as a fixed effect and patient as a random effect, and performed t-tests to assess whether the gradient of the line across the time variable significantly differed from zero. Data were subjected to statistical analyses using SPSS, version 25 (IBM Japan, Ltd., Tokyo, Japan), and a probability (P) value of <0.05 was considered to be significant.
Results
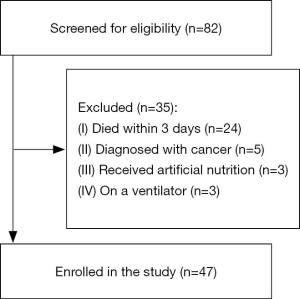
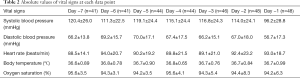
Eighty-two patients died during the study period. Thirty-five patients who did not meet the inclusion criteria were excluded, and, thus, 47 patients were ultimately analyzed (Figure 1). Mean age was 81.0 years and 52.1% were male. The most common disease on admission was respiratory diseases (Table 1). Table 2 summarizes the absolute value of vital signs at each data point. The number of data points at each time differed because the length of hospital stays varied between patients. No significant changes were observed in vital signs from day −7 to day −3. In contrast, significant decreases were noted in systolic blood pressure (P<0.001), diastolic blood pressure (P<0.001), and oxygen saturation (P=0.001) from day −3 to death (Figure 2).

Full table
Full table

Discussion
The present results revealed that blood pressure and oxygen saturation significantly decreased from day −3 to death, whereas no significant changes were observed in vital signs from day −7 to day −3.
Similar changes in vital signs may occur in the last days of life between cancer and non-cancer patients. Hwang et al. investigated changes in vital signs in the last 2 days before death in terminal cancer patients, and reported significant reductions in blood pressure and oxygen saturation (7). Bruera et al. also found significant decreases in blood pressure and oxygen saturation in the three days before death in terminal cancer patients (15). Therefore, similar changes may occur in vital signs before impending death regardless of the disease, and the methods employed to predict impending death in cancer patients may be applicable to non-cancer patients. Hui et al. investigated physical signs and symptoms in the last days of life in cancer patients, and based on the findings obtained, a diagnostic model to predict impending death was developed (9,10,19). Further studies are needed to confirm whether this prognostic tool for impending death may be applied to non-cancer patients.
The present study had some several limitations that need to be addressed. This was a single-center study with a small sample size. We used the Shapiro-Wilk test to confirm the normal distribution of each vital sign, and confirmed that the distributions of vital signs were generally normal. However, this is not a fatal issue in an exploratory study. Further studies are needed to establish whether the changes observed in vital signs in the dying phase are similar in other settings with a large sample. Furthermore, subjects in the present study were acutely ill, and many had received medication that may have affected their vital signs and survival times, including fluid therapy, antipsychotic medication, antiarrhythmic drugs, and steroids. Since the present study was conducted in a general acute care hospital in Japan, the results obtained reflected real-life clinical settings.
Conclusions
In non-cancer patients, similar to terminal cancer patients, significant decreases were observed in blood pressure and oxygen saturation from day −3 to death, whereas no significant changes were noted from day −7 to day −3. These changes in blood pressure and oxygen saturation have potential as indicators of prognosis within three days of death. Further studies on clinical signs and their diagnostic characteristics for impending death in non-cancer patients are needed.
Acknowledgments
We would like to thank each of the following contributors: Kazushi Maruo, PhD (Department of Biostatistics, Faculty of Medicine, University of Tsukuba), Mikiya Sato, MD, PhD (Health Services Research and Development Center, University of Tsukuba), Ryohei Goto, PhD (Department of Primary Care and Medical Education, Faculty of Medicine, University of Tsukuba), Minoru Ebihara, MD (Kamisu Saiseikai Hospital), and Hiroki Takahashi, MD (Kamisu Saiseikai Hospital).
Funding: None.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist (available at http://dx.doi.org/10.21037/apm-20-1054)
Data Sharing Statement: Available at http://dx.doi.org/10.21037/apm-20-1054
Peer Review File: Available at http://dx.doi.org/10.21037/apm-20-1054
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/apm-20-1054). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The present study was approved by the Institutional Review Board of Kamisu Saiseikai Hospital (No. 18-0001). The need for informed consent from family members was waived by the Institutional Review Board of Kamisu Saiseikai Hospital because this study only involved a retrospective chart review. Information on the study content was presented on a notice board in the hospital before its initiation. Study outcomes will not affect the future management of patients. All procedures were performed in accordance with the Declaration of Helsinki (as revised 2013).
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Hui D, Con A, Christie G, et al. Goals of care and end-of-life decision making for hospitalized patients at a Canadian tertiary care cancer center. J Pain Symptom Manage 2009;38:871-81. [Crossref] [PubMed]
- Mori M, Morita T, Igarashi N, et al. Communication about the impending death of patients with cancer to the family: a nationwide survey. BMJ Support Palliat Care 2018;8:221-8. [Crossref] [PubMed]
- Otani H, Yoshida S, Morita T, et al. Meaningful Communication Before Death, but Not Present at the Time of Death Itself, Is Associated With Better Outcomes on Measures of Depression and Complicated Grief Among Bereaved Family Members of Cancer Patients. J Pain Symptom Manage 2017;54:273-9. [Crossref] [PubMed]
- Mori M, Yoshida S, Shiozaki M, et al. “What I Did for My Loved One Is More Important than Whether We Talked About Death”: A Nationwide Survey of Bereaved Family Members. J Palliat Med 2018;21:335-41. [Crossref] [PubMed]
- Heyland DK, Dodek P, Rocker G, et al. What matters most in end-of-life care: perceptions of seriously ill patients and their family members. CMAJ 2006;174:627-33. [Crossref] [PubMed]
- Hui D. Unexpected death in palliative care: what to expect when you are not expecting. Curr Opin Support Palliat Care 2015;9:369-74. [Crossref] [PubMed]
- Hwang IC, Ahn HY, Park SM, et al. Clinical changes in terminally ill cancer patients and death within 48 h: when should we refer patients to a separate room? Support Care Cancer 2013;21:835-40. [Crossref] [PubMed]
- Morita T, Ichiki T, Tsunoda J, et al. A prospective study on the dying process in terminally ill cancer patients. Am J Hosp Palliat Care 1998;15:217-22. [Crossref] [PubMed]
- Hui D, dos Santos R, Chisholm G, et al. Clinical signs of impending death in cancer patients. Oncologist 2014;19:681-7. [Crossref] [PubMed]
- Hui D, Hess K, dos Santos R, et al. A diagnostic model for impending death in cancer patients: Preliminary report. Cancer 2015;121:3914-21. [Crossref] [PubMed]
- Matsunami K, Tomita K, Touge H, et al. Physical Signs and Clinical Findings Before Death in Ill Elderly Patients. Am J Hosp Palliat Care 2018;35:712-7. [Crossref] [PubMed]
- Lunney JR, Lynn J, Foley DJ, et al. Patterns of functional decline at the end of life. JAMA 2003;289:2387-92. [Crossref] [PubMed]
- Chen YT, Ho CT, Hsu HS, et al. Objective palliative prognostic score among patients with advanced cancer. J Pain Symptom Manage 2015;49:690-6. [Crossref] [PubMed]
- Sato K, Yokoi H, Tsuneto S. Shock Index and Decreased Level of Consciousness as Terminal Cancer Patients' Survival Time Predictors: A Retrospective Cohort Study. J Pain Symptom Manage 2016;51:220-31.e2. [Crossref] [PubMed]
- Bruera S, Chisholm G, Dos Santos R, et al. Variations in vital signs in the last days of life in patients with advanced cancer. J Pain Symptom Manage 2014;48:510-7. [Crossref] [PubMed]
- Von Ele E, Altman DG, Egger M, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: guidelines for reporting observational studies. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: guidelines for reporting observational studies. Int J Surg 2014;12:1495-9. [Crossref] [PubMed]
- Hosoi T, Ozone S, Hamano J. Survival time after marked reduction in oral intake in terminally ill noncancer patients: A retrospective study. J Gen Fam Med 2020;21:9-14. [Crossref] [PubMed]
- Quan H, Li B, Couris CM, et al. Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol 2011;173:676-82. [Crossref] [PubMed]
- Hui D, Dos Santos R, Chisholm G, et al. Bedside clinical signs associated with impending death in patients with advanced cancer: preliminary findings of a prospective, longitudinal cohort study. Cancer 2015;121:960-7. [Crossref] [PubMed]


