Questionnaires measuring quality of life and satisfaction of patients and their relatives in a palliative care setting—German translation of FAMCARE-2 and the palliative care subscale of FACIT-Pal
Introduction
The World Health Organization (WHO) defines palliative care as “an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness” (1).
Quality of life (QoL) itself cannot be uniquely defined as it composes for every individual differently depending on unique experiences and expectations. Thus QoL has to be defined individually for every person. Accordingly it remains challenging to transfer the idea of “QoL” to a concrete definition allowing collecting respective data sets for scientific interpretation.
The evaluation of QoL in a palliative care setting is a precondition for the establishment of high qualitative care procedures. Previous studies showed that the attending physicians’ estimation of the patient’s QoL differs from the patient’s self-assessment (2).
In order to evaluate if measures and procedures achieve the goals of palliative care, a direct feedback of the concerned patient group is inevitable.
Several research teams already have composed questionnaires evaluating QoL to allow qualitative and quantitative analyses of different QoL aspects.
Examples are the QLQ-C15-PAL of the EORTC (European Organization for Research on Treatment of Cancer) Quality of Life Group (3), the McGill Quality of Life Questionnaire (MQoL) (4) as well as the FACIT-Pal (5-9) of the Functional Assessment of Chronic Illness Therapy (FACIT) group of questionnaires (10,11).
The respective questionnaires are currently only partially available in German limiting their application field to Anglophone areas.
The FACIT-Pal questionnaire is composed of 46 questions, 19 of those, concerning the palliative care subscale, were first published by Greisinger et al. (5). All FACIT questionnaires include a basic questionnaire assessing physical, social, emotional and functional status. The questionnaires are completed by specific subscales, in this case a palliative care subscale. As a result one receives a comprehensive picture of general aspects, covering a wide patient collective as well as specific aspects addressing selected patient groups. The basic questionnaire is available in German while the specific palliative care part is currently only available in Japanese, Portuguese and Malay.
Concerning the relatives’ satisfaction with the provided care there is a smaller variety of questionnaires available allowing a statistical assessment. Two examples are the Quality of End-of-Life care and Satisfaction with Treatment (QUEST) (12) and the FAMCARE-2 (13). Both questionnaires are currently not available in German. The FAMCARE-2 addresses the satisfaction with several palliative care aspects within 17 questions. Its previous version—FAMCARE—is widely established in surveys among relatives in Anglophone countries (14-17). In contrary to the FAMCARE, the FAMCARE-2 does not ask for the family’s perception of a specific care taker’s performance but for the perception of the care team’s performance (13). It is applicable to inpatient and outpatient settings. The FAMCARE-2 is currently only available in English, Italian and Swedish.
Herein we introduce to the best of our knowledge for the first time in German the two key questionnaires FAMCARE-2 as well as the specific palliative care subscale of FACIT-Pal. The translations to German were performed with a structured methodology and finally authorized by the original scale developers. The questionnaires are currently in use in the PaRoLi study (Palliative Care in Rostock: Focus on Quality of Life) and are now available for scientific research in German speaking areas.
Methods
Initially the consent of the original scale developers was given to translate their questionnaires.
To achieve an adequate and internationally comparable version, the translation was performed according to the FACIT standard translation protocol (Figure 1) including several independent translators having extraordinary skills in English and German.
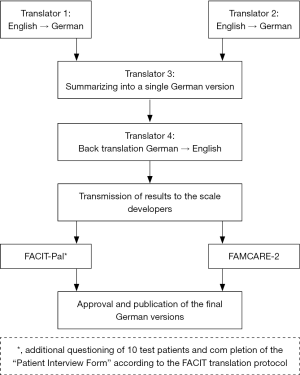
Initially the translation was performed by two individual translators from English to German. In the following a third translator unified both translations resulting in a single version. A fourth translator translated the obtained version back to English without knowing the original English template. The newly generated English version was sent to the developers of the original questionnaires for approval.
During the course of translation of FACIT-Pal the scale developers required an additional testing of the translated questionnaires of ten test patients. After the patients completed the questionnaire an additional “Patient Interview Form” was filled in by the participants. This additional form asked for personal perceptions concerning questions, key words and understanding of the questionnaire. Further, some sentences had to be paraphrased. With special interest statements were analyzed, whether they were misunderstandable or inadequate. The completed translated questionnaires and the additional evaluating datasets were sent to the original FACIT-Pal developers.
As FAMCARE-2 does not require a standard translation protocol the questionnaire was translated as described for FACIT-Pal. The translation was not followed by an additional questioning of 10 persons. The final translated questionnaire was finally approved by the developers of the original questionnaire.
Results
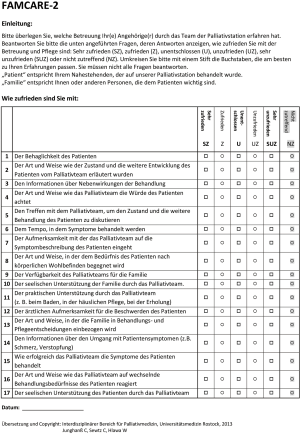
The translation was performed between March and May 2013. The German translations are displayed in the Figure 2 (FACIT-Pal—German translation) and Figure 3 (FAMCARE-2—German translation). For the full German version of the FACIT-PAL including the general FACIT questions which had been translated earlier, see supplement material (Figure S1). The original sense of the questions was not altered. The original scale developers did not find significant discrepancies between their original questionnaire and the newly generated back translated version.

Discussion
Herein we report the translation of two important questionnaires in palliative care and the trial versions authorized by the original questionnaire developers.
The utilization of questionnaires is key when complex trails as palliative care are to be evaluated in evidence based research approaches. Several international versions of the FACIT-Pal (8,18) and the FAMCARE-2 (19,20) proved as useful tools to evaluate and measure QoL of palliative care patients as well as the procedural care satisfaction of the accompanying relatives.
The translation of an established questionnaire requires more than simple direct wording translation. An additional adaption of the phrasing must be performed to ensure the conservation of the original meaning and structure.
Currently the QoL of inpatient and outpatient patients and their relatives is being evaluated within the PaRoLi study (21). Patients and relatives using the German questionnaire translation feel that the questionnaires are easily understandable and easily to be completed. The questionnaires were well accepted by the majority of the asked people.
Conclusions
The translated versions of FACIT-Pal and FAMCARE-2 can now be introduced in studies performed in German speaking areas.
Acknowledgements
We would like to thank Jason Bredle for his excellent help and cooperation during the course of translation of the FACIT-Pal. Furthermore we would like to thank all staff of the Palliative Care Unit of the University of Rostock for their dedicated work and their ongoing willingness to help within this project. We would also like to thank all patients, who participated, for sharing a part of their precious time with us.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: Prior to translation, the study protocol and data collection plan were approved by the institutional review boards and ethical committee of Rostock University Medical Center (No. A 2013-0028). The patients provided informed written consent.
References
- WHO. WHO Definition of Palliative Care. WHO (Internet). World Health Organization; 2012 (cited 2017 Nov 20); Available online: http://www.who.int/cancer/palliative/definition/en/
- Petersen MA, Larsen H, Pedersen L, et al. Assessing health-related quality of life in palliative care: Comparing patient and physician assessments. Eur J Cancer 2006;42:1159-66. [Crossref] [PubMed]
- Groenvold M, Petersen MA, Aaronson NK, et al. The development of the EORTC QLQ-C15-PAL: A shortened questionnaire for cancer patients in palliative care. Eur J Cancer 2006;42:55-64. [Crossref] [PubMed]
- Cohen SR, Mount BM, Strobel MG, et al. The McGill Quality of Life Questionnaire: a measure of quality of life appropriate for people with advanced disease. A preliminary study of validity and acceptability. Palliat Med 1995;9:207-19. [Crossref] [PubMed]
- Greisinger AJ, Lorimor RJ, Aday LA, et al. Terminally ill cancer patients. Their most important concerns. Cancer Pract 1997;5:147-54. [PubMed]
- Lyons KD, Bakitas M, Hegel MT, et al. Reliability and Validity of the Functional Assessment of Chronic Illness Therapy-Palliative Care (FACIT-Pal) Scale. J Pain Symptom Manage 2009;37:23-32. [Crossref] [PubMed]
- Khan L, Zeng L, Cella D, et al. Patients’ and health care providers' evaluation of quality of life issues in advanced cancer using Functional Assessment Of Chronic Illness Therapy - Palliative Care Module (FACIT-pal) scale. World J Oncol 2012;3:210-6. [PubMed]
- Harding R, Selman L, Ali Z, et al. Wellbeing among sub-Saharan African patients with advanced HIV and/or cancer: an international multicentred comparison study of two outcome measures. Health Qual Life Outcomes 2014;12:80. [Crossref] [PubMed]
- Lien K, Zeng L, Nguyen J, et al. Comparison of the EORTC QLQ-C15-PAL and the FACIT-Pal for assessment of quality of life in patients with advanced cancer. Expert Rev Pharmacoecon Outcomes Res 2011;11:541-7. [Crossref] [PubMed]
- Cella DF, Tulsky DS, Gray G, et al. The functional assessment of cancer therapy scale: Development and validation of the general measure. J Clin Oncol 1993;11:570-9. [Crossref] [PubMed]
- Webster K, Cella D, Yost K. The Functional Assessment of Chronic Illness Therapy (FACIT) Measurement System: properties, applications, and interpretation. Health Qual Life Outcomes 2003;1:79. [Crossref] [PubMed]
- Sulmasy DP, McIlvane JM, Pasley PM, et al. A scale for measuring patient perceptions of the Quality of End-of-life care and Satisfaction with Treatment: The reliability and validity of QUEST. J Pain Symptom Manage 2002;23:458-70. [Crossref] [PubMed]
- Aoun S, Bird S, Kristjanson LJ, et al. Reliability testing of the FAMCARE-2 scale: measuring family carer satisfaction with palliative care. Palliat Med 2010;24:674-81. [Crossref] [PubMed]
- Kristjanson LJ. Validity and reliability testing of the FAMCARE Scale: Measuring family satisfaction witg advanced cancer care. Soc Sci Med 1993;36:693-701. [Crossref] [PubMed]
- Follwell M, Burman D, Le LW, Wakimoto K, et al. Phase II study of an outpatient palliative care intervention in patients with metastatic cancer. J Clin Oncol 2009;27:206-13. [Crossref] [PubMed]
- Ringdal GI, Jordhøy MS, Kaasa S. Family satisfaction with end-of-life care for cancer patients in a cluster randomized trial. J Pain Symptom Manage 2002;24:53-63. [Crossref] [PubMed]
- Grunfeld E, Coyle D, Whelan T, et al. Family caregiver burden: results of a longitudinal study of breast cancer patients and their principal caregivers. CMAJ 2004;170:1795-801. [Crossref] [PubMed]
- Bakitas M, Lyons KD, Hegel MT, et al. Effects of a Palliative Care Intervention on Clinical Outcomes in Patients With Advanced Cancer. JAMA 2009;302:741. [Crossref] [PubMed]
- Ullrich A, Ascherfeld L, Marx G, et al. Quality of life, psychological burden, needs, and satisfaction during specialized inpatient palliative care in family caregivers of advanced cancer patients. BMC Palliat Care 2017;16:31. [Crossref] [PubMed]
- Pidgeon TM, Johnson CE, Lester L, et al. Perceptions of the care received from Australian palliative care services: A caregiver perspective. Palliat Support Care 2018;16:198-208. [PubMed]
- Sewtz C, Hlawa W, Kragl B, et al. Übersetzung eines geeigneten Instruments zur Messung der Lebensqualität und Symptomkontrolle von stationär und ambulant betreuten Palliativpatienten (FACIT-Pal) sowie eines Fragebogens zur Betreuungszufriedenheit ihrer Angehörigen (FAMCARE-2). Palliativmedizin 2014;15:V106. [Crossref]



