The advance care planning experiences of people with dementia, family caregivers and professionals: a synthesis of the qualitative literature
Introduction
Recent global dementia policy has placed emphasis upon early diagnosis, better information and support as well as enhanced end-of-life care throughout the condition trajectory (1-3). Advance decision making or advance care planning (ACP) is considered an important part of the process in achieving high quality future care consistent with that of the person’s wishes. ACP or advance decision making exists in a range forms around the globe and often culminates in the expressed wishes of the person with dementia in the form of a statement or transfer of decision making powers. In the UK, supporting people with dementia and family carers to engage with advance decision making at the earliest opportunity is identified as a National Institute for Health & Care Excellence (NICE) quality standard (4). ACP is an important component of the European Association of Palliative Care White Paper on palliative care for people with dementia (5).
Definitions of ACP vary. We have chosen to use the EAPC definition—“Advance care planning (ACP) is a formalized process of communication between patients, relatives and professional caregivers. It is a voluntary process of discussion and review enabling individuals to express, and, if they wish, record views, values and specific treatment choices to inform their future care. ACP promotes the documentation of patients’ preferences in their medical file, the communication of these preferences to family and friends, and the periodic review of preferences as circumstances change” (6), and will use the acronym ACP throughout the remainder of this paper. The policy and professional discourse around ACP, particularly in the field of dementia care, contains an implicit understanding that it is both necessary and in the long term interests to the person with the condition to engage in their future planning. By implication, therefore, ACP can mediate the possibility of hospital admission and inappropriate care (7,8). As such there have been a number of studies seeking to demonstrate ACP effectiveness via the development and testing of novel interventions. ACP counselling demonstrated an increased likelihood to engage in future planning around the medical care for people with dementia and their family carers (9,10). Also, improved engagement with ACP following the provision of video information (11) and raised family member awareness of the impact of dementia (12) has been noted.
Despite intensive efforts to facilitate planning discussions via structured consultations some studies have noted poor take up of ACP, see for example Vandervoort et al. (13). Indeed it is this latter point which appears to be a feature of the ACP planning literature in the field of dementia care. A systematic review of the take up of ACP in a range of conditions has highlighted that, when compared with conditions such as cancer, people with dementia are far less likely to have any form of ACP (14). A number of studies have confirmed this observation (15,16). Quantitative research has gone some way to help in highlighting factors which may contribute to its take up, or indeed prevent its development, within this population of health users. We are aware, however, of a small literature, sourced through qualitative research deigns, which address the complexities and challenges inherent within the field of ACP and dementia. Our aim was to undertake a synthesis of the qualitative research undertaken within the field of ACP and dementia with an emphasis upon experiences, barriers and facilitators.
Methods
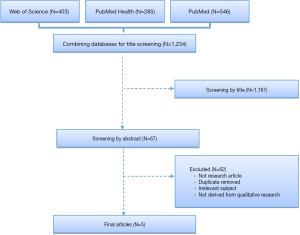
We carried out a search of the literature using the terms: ACP, dementia, Alzheimer’s disease, Lewy body disease, Huntington disease, Frontotemporal dementia, qualitative research, between 2007 and 2017. We searched three databases: Web of Science; PubMed Health; PubMed. Studies were excluded on the basis of: research not derived from qualitative research; opinion pieces and grey literature; non-English language; dissertations and PhD theses; conference proceedings. The flowchart (Figure 1) provides a description of the identification of relevant papers. A 32-item checklist was applied to each of the final selected papers to ensure that all displayed appropriate standards of conduct and reporting (17). An approach to qualitative synthesis described by Thomas and Harden was utilized (18). This involves three stages. Firstly, the authors undertook coding of the findings of original texts, identifying notable material. Following a reading through of each article, this was achieved by means of putting to one side our priori concerns and coding findings as they are presented in the original papers. Thus a range of codes were developed each unique to each of the studies. Secondly, we developed descriptive themes, by bringing together codes which shared similar characteristics. This involved constant comparison of codes, shifting and reordering to produce the themes. Finally, we generated analytical themes through going back to the aims of our work and highlighted those elements of the experience to be most relevant. This involves ‘going beyond’ the content of the original studies (18) and instead returning to our original aims of an exploration of ACP experiences, barriers and facilitators. By taking descriptive themes and merging these with our aims in mind we were thus able to highlight abstract notions within the papers which are helpful in identifying challenges, barriers and facilitators to ACP.
Results
Five studies were identified as meeting the criteria. These are summarized in Table 1. Five key analytical themes emerged from our synthesis of this literature. These are outlined below.

Full table
Breadth and scope of future planning
Despite evidence suggesting that people with dementia and their family caregivers do not engage in formal ACP on a large scale, evidence within these studies suggests that planning of a broad nature is undertaken. All five studies point to the active engagement in consideration of the future, the implications of dementia on living arrangements, financial concerns, relationships and services. Hirschman et al. (21) point to both ‘active’ and ‘reactive’ forms of planning which encompass ‘informal conversations’ about issues which exist outside of the parameters of ACP, including financial plans. Dickinson et al. (20) also highlighted a preference for this informal approach and include the reporting of funeral plans and general statements about wishes and future aspirations. Furthermore, the idea that formal plans were advantageous, as a result of the legal status of ACP, is dismissed in this paper, with some participants in the study identifying that people known to them would contribute to end of life decision making via a ‘best interests’ or ‘in the moment’ route based on stated ‘wishes and desires’.
Evidence of involvement in formal ACP procedures was also highlighted. Two papers in particular were undertaken to explore the experience of ACP interventions (19,22). Both papers explored elements of satisfaction and dissatisfaction, some of which will be explored later in this paper. It is notable, however, that both papers highlight a sense of relief in participating in ACP, particularly from a family caregiver’s perspective. Ashton et al. (19) explore the experience following ACP plans being put into place once the person with dementia lacked capacity and is no longer available to contribute. Caregivers report satisfaction in having an opportunity to speak on the person’s behalf and subsequently contribute to the avoidance of distress through ‘futile’ procedures. Poppe et al. (22) note the importance of ACP to people with dementia and their family caregivers. In particular they indicate that ACP processes help to provide a space within which participants can consider important future decisions and provides the opportunity to share ones wishes and thoughts.
Challenges to ACP
The papers included within this qualitative synthesis highlight a number of significant challenges in undertaking ACP. These challenges act as barriers to the completion of ACP in some of the studies. In others these are noted as uncomfortable experiences or dissatisfying aspects on completion of ACP. Four challenges are noted here.
Addressing the end of life
Acknowledging one’s future needs at the end of life is viewed within these studies as a difficult undertaking and the avoidance of distress associated with such planning is viewed as a goal in itself (19). Whilst raising the prospect of future planning relating to financial and property affairs is viewed as relatively straightforward, professionals find the idea of discussing end of life issues extremely challenging (23). Poppe et al. (22) identify this as one or the more problematic aspects in their qualitative evaluation of an ACP intervention. They describe problems in approaching what are perceived by staff to be uncomfortable situations, who question the timing of raising the subject. Staff in the same paper also encounter people with dementia who wish to talk about assisted suicide. Dickinson et al. (20) identify the topic of end of life care as a significant challenge and also a source for concern in relation to the timing of ACP conversations. They note reluctance by people with dementia and their family caregivers to ‘think too far in advance’. Staff in the study undertaken by Robinson et al. (23) developed a sense of timing around end of life care issues, based upon specific cues and a skilled assessment of the person being ready for such conversations. Implicit in this appraisal of the practice encounter is recognition of the sensitivities surrounding the subject.
Preference for the informal
The formalities associated with ACP are noted as a potential obstacle to open discussion in the context of planning for the future. Hirschman et al. (21) noted that people with dementia and their families plan on both a formal and informal basis. Dickinson et al. (20) highlight a preference for the latter and what are perceived as overly formal ACP procedures as one of the primary barriers for a failure to engage with it. Further, participants in the study note a confidence in the unspoken knowledge held by the family, based upon life-long conversations. The potential utility of such knowledge in being able to guide decision making, particularly in relation to significant transitions such as admission to care or end of life. Family caregivers in the same study are also confident that they would be in a position to use this knowledge to help inform decision making at a point of time in the future. Furthermore, the act of formally recording this knowledge is viewed as ‘harsh and inhumane’ with a carer noting that it would be akin to ‘putting him to his death’.
Multiple scenarios
The complexity and uncertainty of the future also provides ACP with a significant challenge. Staff confidence in formal ACP is undermined by the reality of being faced with complex care and treatment scenarios that, as they see it, cannot be captured in a comprehensive manner within a written record (23). This perceived limitation is also noted by people with dementia and families. Dickinson et al. (20) identify interview data within which participants view the future as being dependent upon a complex set of variables, relationships and unknowns which would have a major influence upon the decisions likely to be faced. The capacity for ACP to be able to capture such complexity is questioned.
Getting the timing right
Dementia presents particular challenges to the question of timing ACP conversations. Striking a balance between gaining insight into one’s diagnosis of dementia and losing capacity to be involved in the process is at the heart of this challenge. Poppe et al. (22) identify a desire to undertake ACP at the earliest opportunity, but such discussions should not take place directly following a diagnosis. Similarly Robinson et al. (23) note professional viewpoints which aimed to appraise in a skilled way the timing of such conversations, adding that the ‘right time’ is often very unclear. For people with dementia identifying the right timing is of particular concern. Aware of the trajectory of dementia, albeit uncertain, and a requirement to become engaged in ACP participants in the Dickinson et al. study (20) are unclear about timing, citing the length of time it took to coming to terms with a diagnosis and a need for clarity about what the challenges are as presenting a particularly complex backdrop to the issue of timing ACP.
Postponing ACP
The postponement of ACP is a significant feature of the qualitative research undertaken in this field. Two of the papers included in this qualitative synthesis centre firmly on this aspect of the experience. Indeed Hirschman et al. (21) identify two approaches to this postponement: passive avoidance and active avoidance (used below to frame our findings). Dickinson et al. (20) highlighted a range of explanations for a desire to postpone ACP. We identified three components of the literature.
Passive avoidance
Both Hirschman et al. (21) and Dickinson et al. (20) identify approaches to a failure to engage in ACP which can be characterized in this way. Not seeing the significance of ACP is a particular explanation for this approach to ACP. Studies noted an absence of any urgency amongst families to begin to actively consider the formal recording of wishes about future treatment in particular, especially against a backdrop of managing the diagnosis of dementia. There is a sense within both papers that the prospect of formal planning presented a break with the continuity of life itself (22). Just as the contemplation of end of life discussions is viewed as a source of discomfort, so is the notion of future planning. A scenario described as ‘plodding on’ captures what is described as the passive response to the idea of ACP (20). There is a sense in one of the papers that on reflection some participants regretted not taking action, after it was acknowledged that the person with dementia was no longer able to contribute to detailed discussions (22).
Active avoidance
Whilst there is evidence of a passive approach to postponement, there are clear indications within the literature that people with dementia and family caregivers are also engaged in ‘active’ strategies to avoid formal planning. Such strategies are rooted within a set of concerns about future impairment and the implications this holds for the lives of those affected. The word ‘denial’ is used in one of the papers, although this term masks a complexity of a process for people in being able to understand a diagnosis and contemplate its implications. Nonetheless, there is evidence that study participants display an inclination to evade detailed discussion about the consequences of impairment change with one family member participant describing this approach as keeping one’s ‘head in the sand’ (22). Additional evidence of ‘active avoidance’ is presented on the basis of an open appraisal of the situation. It is thought new technology and service options might yield alternative choices in the future (20).
Prognostication
The question of holding enough information to be able to make clear decisions is a significant concern for participants in these studies. Just as new technology and service options may become available, so is there uncertainty about the length of time a person has to be involved in decision making and what their likely contribution might be. ACP in this context could only occur when participants were clear what the likely scenario in terms of disease trajectory might be. Unlike other disease trajectories (such as cancer), participants are aware that the future holds many questions and as such responded by postponing ACP until ‘it was clear what they were facing’ (19).
Confidence in systems
Despite efforts to engage in ACP activity, the confidence that health and social care systems would be in a position to be able to respond to expressed wishes is questioned in these studies. Two particular concerns are discerned within the qualitative research included here.
Delivering choice?
Professional unease about the potential to enact detailed recorded plans in an ACP document is expressed in these studies. Robinson et al. (23) note this as a significant source of concern in terms of professional standards and the viability of ACP. Indeed participants in this study report feeling that they had ‘let down’ patients when unable to provide a level of service to meet with their expressed wishes. Constraints placed upon professionals by resources available to them at a particular time, and the tension between their own training and the expressed wishes of a patient, exposes ACP to the risk of being undermined. Expressed wishes are further challenged when alternative preferences by relatives are introduced (23).
Constraints on future services
The confidence to deliver services and care consistent with the expressed wishes of people with dementia and their families is further undermined in considering the changes which might occur to the healthcare landscape in the future. This fear is addressed in two of the papers. Robinson et al. (23) again drawing on the views of professionals highlight this as a concern. From the perspective of the person with dementia and their family, a shortage of confidence about the potential for those plans to be put into place existed. This is a particular concern for those expressing a wish to remain at home, even in an end of life context. Participants here describe their own wishes as being undermined by an awareness of scarcity of resources available, professionals in being able to execute these plans (20).
Making ACP happen for people with dementia
Despite the challenges and potential threats to ACP outlined above, all five papers included in this synthesis can help in gaining a fuller understanding of what might be required to enable ACP to become more fully established within the population of people affected by dementia. We have discerned three important aspects of the literature.
Taking responsibility, starting the conversation
Notwithstanding our earlier discussion about the nature of timing, a particular aspect of the papers included in this qualitative synthesis note the importance of responsibility and leadership. Some confusion exists here, with professionals being unsure about who should initiate and facilitate ACP and people with dementia and their families equally unclear. Papers alluded to uncertainty and doubt as a feature of the service landscape. Robinson et al. (23) note professional responsibilities as being unclear with little guidance on where in the care pathway conversations about ACP should be located, particularly given the broad range of future planning to be addressed. The two intervention studies, which concluded relative satisfaction with the process, did not suffer from this problem as they were embedded in a framework of clearly defined protocol and lines of responsibility (19,21).
The skills to enable ACP to flourish
The capacity of professionals, as well as people with dementia and families, to understand and practice formal future planning is identified throughout this literature as being important if it is to develop. Professionals view the capacity issues as being at the heart of their own safe practice. In their evaluation of an ACP intervention in care homes Ashton et al. (19) identify the skills used to provide families with assurance, direction and peace of mind when addressing hugely sensitive topics such as the potential withdrawal of medical treatment. The significance of ‘person-centred’ approaches to this undertaking is also stressed. The confidence that staff require to embark upon ACP work, and the skills required to enter into such conversations is also noted in the literature. Poppe et al. (22) highlight this in their evaluation of a novel ACP intervention, noting knowledge of dementia, resources, skilled facilitation and an understanding of ‘one’s own limitations’ as being essential in being able to carry out safe practice.
Relational aspects of ACP
Positive experiences of ACP are linked within these studies with trusting relationships between all involved, underpinned by continuity and positive relationships. Hirschman et al. (21) note the importance of professional and family prompts as being important in beginning the ACP process. Implicit here is the existence of a network of people who can advise the person with dementia and facilitate the process in a sensitive and informed manner. Conversely an absence of a trusting advisor is viewed as a substantial barrier to beginning the process. Dickinson et al. (20) cite an absence of support in the form of legal advisors, charity and professional networks, which might help people with dementia and their families when navigating the ACP process, as a noteworthy obstacle to ACP. Additionally the space and time to discuss a range of very complex issues is also highlighted, particularly when family caregivers are struggling to balance very difficult demands whilst also striving to plan for the future.
Discussion
Concern has for some time been expressed about the relative low take up of ACP by people with dementia and their families (24,25). Quantitative research has gone some way to help in highlighting factors which may contribute to its take up or indeed prevent its development within this population. These include family characteristics (age; carer burden; preparedness and knowledge of the person with dementia), professional characteristics (attitudes, education and training) as well as the capacity of the person with dementia themselves (16).
We feel that whilst useful, such research has limitations in that it fails to fully explore the ways in which ACP is perceived and experienced by this population. This qualitative synthesis of the experiences of people with dementia, family caregivers and professionals and the barriers and facilitators to ACP has identified additional material aimed at enabling further insight into the ways in which future planning is lived and viewed. We identified five qualitative research studies from within this field of work. As a result of synthesis of the data from each of the five studies five key themes are identified: breadth and scope of future planning; challenges to ACP; postponing ACP; Confidence in Systems and Making ACP happen for people with dementia. The synthesized findings shed light on the ongoing challenges of the use and further development of ACP. These challenges do, to some extent, replicate aspects of the literature from other diseases and disorders. Challenges in relation to the sensitivity to end of life discussions amongst patients have been detected elsewhere in the ACP literature, as it is here. Barclay et al. (26) highlighted a range of responses and focus on the reluctance to openly discuss end of life plans amongst heart failure patients, whilst Bernacki et al. (27) also point to physician distress. In this sense the dementia population may be no different. The uncertainty around time from diagnosis to end of life is, however, something particularly appropriate to dementia (28). The qualitative research included in this synthesis has drawn attention to the degree of informal discussion around future care and the extent to which formal procedures are viewed as interruptive of the natural conversations within families. In an evaluation of nurse involvement in initiation of ACP in the community Seymour et al highlighted what participants viewed as the ‘policy focus on instructional directives which related poorly to patients’ concerns (29). There is clearly a tension here between the need for formal recording and the preference for people with dementia and their families to rely on more ‘informal’ mechanisms and not just written documentation alone (7,30).
As a result of this review we can now begin to understand more fully those particular aspects of the experience that are related firmly to the diagnosis of dementia. Notably, the studies included in this paper highlight specific concerns about the timing of ACP discussions. The issue of timing was of direct concern to van der Steen et al. in undertaking a systematic review (31). The inconclusive nature of the question of timing in the review adds credence to the notion that initiation is both variable and complex, meaning that the skills of professionals in being able to appraise pre-disposition to ACP all the more important. The potential postponement of ACP forms part of this and is also highlighted here. Again this is not new to the wider ACP literature (29). A number of explanations have been presented here. This reluctance to engage in ACP does, however, present a challenge to policy makers and opens up new debates about the motivations for such an approach (32). Again we can detect within the qualitative research presented here a preference, amongst some people with dementia and their family members, for reliance on implicit knowledge based on family relationships and values to help guide end of life decision, centred upon a best interests model. It may well be, however, that a relative absence of formal knowledge about ACP contributes to this preference. Quantitative research has demonstrated that awareness raising interventions contribute to improved outcomes (9-12). A clearer understanding of the exact nature of this knowledge exchange and how it is used within families would contribute to the development of the field. Further research aimed at exploring this aspect of ACP planning within families is required.
What emerges very clearly here is the insight gained from qualitative endeavours to reflect upon the infrastructure required for ACP to occur in a timely, safe and reliable manner. The two qualitative studies addressing ACP interventions demonstrate the extent to which preparation, leadership, protocol and an ACP culture may lead to more satisfying outcomes. Successful ACP interventions are also able to boast such characteristics from outside of the field of dementia (33), but work within the field would validate our findings here that clearly defined interventions may have more success (34). Further to this, it might be suggested that such clarity and leadership provides professionals with a clear framework within which to work. Professional practice in the field of ACP should be undertaken with confidence that the timing is appropriate and that one has the skills to provide the appropriate support (19,23). More research focusing on the barriers to ACP work among professional groups is required. Importantly the relational aspects of planning allude to a part of the process that is reliant on the people involved as opposed to the method of recording. This commitment of ongoing attention to ACP in dementia has already been noted (35). Indeed work around high quality end of life care in dementia already highlights the significance of intensity and trust in physician and patient relationships in dementia (36).
The study brings together research of a qualitative nature and as such it is difficult to generalize findings on a larger scale. The study focused on those approaches to planning regarded as ACP only. As such other practices to the planning of end of life and palliative care were omitted from the search and analysis. Both of the above points might be regarded as limitations to the study.
This qualitative synthesis of a small number of studies reveals considerable complexity in undertaking ACP in a context of dementia, not least of which is the question of timing. The challenges of ACP for people with dementia, families and professionals are highlighted. It is suggested that the preference for informal approaches be considered and that the skills of those involved in initiating discussions should be given primacy.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Department of Health. Living well with dementia: a national dementia strategy. Accessed 27th March 2017. Available online: https://www.gov.uk/government/publications/living-well-with-dementia-a-national-dementia-strategy
- National Framework for Action on Dementia. Australian Government, Department of Health. Accessed 27th March 2017. Available online: https://agedcare.health.gov.au/ageing-and-aged-care-older-people-their-families-and-carers-dementia/national-framework-for-action-on-dementia-2015-2019
- National Plan to Address Alzheimer’s disease: 2016 Update. US Department of Health & Human Services. Accessed 27th March 2017. Available online: https://aspe.hhs.gov/report/national-plan-address-alzheimers-disease-2016-update
- National Institute for Clinical Excellence. Dementia Quality Standard. London: National Institute for Clinical Excellence, 2010.
- van der Steen JT, Radbruch L, Hertogh CM, et al. White paper defining optimal palliative care in older people with dementia: a Delphi study and recommendations from the European Association for Palliative Care. Palliat Med 2014;28:197-209. [Crossref] [PubMed]
- European Association of Palliative Care. White paper on advance care planning. Accessed 8th July 2017. Available online: http://www.eapcnet.eu/Themes/ClinicalCare/AdvancedCarePlanning.aspx
- Brinkman-Stoppelenburg A, Rietjens J, van der Heide A. The effects of advance care planning on end-of-life care: a systematic review. Palliat Med 2014;28:1000-25. [Crossref] [PubMed]
- Robinson L, Dickinson C, Rousseau N, et al. A systematic review of the effectiveness of advance care planning interventions for people with cognitive impairment and dementia. Age Ageing 2012;41:263-9. [Crossref] [PubMed]
- Binte Ali N, Chan M, Anthony P, et al. Advance care planning for subjects with early dementia – a pilot study. BMC Palliat Care 2012;2:197.
- Awan K, Clark E, Leon L, et al. An Advance Care Planning Initiative to Improve Documentation of Health Care Preferences among Patients with and without Dementia. J Am Geriatr Soc 2010;58:S150.
- Volandes AE, Lehmann LS, Cook EF, et al. Using video images of dementia in advance care planning. Arch Intern Med 2007;167:828-33. [Crossref] [PubMed]
- Riva M, Caratozzolo S, Cerea E, et al. Diagnosis disclosure and advance care planning in Alzheimer disease: opinions of a sample of Italian citizens. Aging Clin Exp Res 2014;26:427-34. [Crossref] [PubMed]
- Vandervoort A, van den Block L, van der Steen JT, et al. Advance directives and physicians' orders in nursing home residents with dementia in Flanders, Belgium: prevalence and associated outcomes. Int Psychogeriatr 2012;24:1133-43. [Crossref] [PubMed]
- Lovell A, Yates P. Advance Care Planning in palliative care: A systematic literature review of the contextual factors influencing its uptake 2008-2012. Palliat Med 2014;28:1026-35. [Crossref] [PubMed]
- Laakkonen ML, Raivio M, Eloniemi U, et al. Disclosure of Dementia Diagnosis and the Need for Advance Care Planning in Individuals with Alzheimer’s Disease. J Am Geriatr Soc 2008;56:2156-7. [Crossref] [PubMed]
- Dening KH, Jones L, Sampson EL. Advance care planning for people with dementia: a review. Int Psychogeriatr 2011;23:1535-51. [Crossref] [PubMed]
- Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32 item checklist for interviews and focus groups. Int J Qual Health Care 2007;19:349-357. [Crossref] [PubMed]
- Thomas J, Harden A. Methods for the Systematic Synthesis of Qualitative Research in Systematic Reviews. BMC Med Res Methodol 2008;8:45. [Crossref] [PubMed]
- Ashton S, Roe B, Jack B, et al. A study to explore the experience of advanced care planning among family caregivers and relatives of people with advanced dementia. BMJ Supportive & Palliative Care 2011;1:91. [Crossref]
- Dickinson C, Bamford C, Exley C, et al. Julian Hughes and Louise Robinson Planning for tomorrow whilst living for today: the views of people with dementia and their families on advance care planning. Int Psychogeriatr 2013;25:2011-21. [Crossref] [PubMed]
- Hirschman KB, Kapo JM, Karlawish JH. Identifying the factors that facilitate or hinder advance planning by persons with dementia. Alzheimer Dis Assoc Disord 2008;22:293-8. [Crossref] [PubMed]
- Poppe M, Burleigh S, Banerjee S. Qualitative Evaluation of Advanced Care Planning in Early Dementia (ACP-ED). PLoS One 2013;8:e60412. [Crossref] [PubMed]
- Robinson L, Dickinson C, Bamford C, et al. A qualitative study: professionals' experiences of advance care planning in dementia and palliative care, 'a good idea in theory but ...'. Palliat Med. 2013;27:401-8. [Crossref] [PubMed]
- Lewis M, Rand E, Mullaly E, et al. Uptake of a newly implemented advance care planning program in a dementia diagnostic service. Age Ageing 2015;44:1045-9. [Crossref] [PubMed]
- Garand L, Dew M, Lingler J, et al. Incidence and Predictors of Advance Care Planning Among Persons with Cognitive Impairment. Am J Geriatr Psychiatry 2011;19:712-20. [Crossref] [PubMed]
- Barclay S, Momen N, Case-Upton S, et al. End-of-life care conversations with heart failure patients: a systematic literature review and narrative synthesis. Br J Gen Pract 2011;61:e49-e62. [Crossref] [PubMed]
- Bernacki RE, Block SD. American College of Physicians High Value Care Task Force. Communication about serious illness care goals: a review and synthesis of best practices. JAMA Intern Med 2014;174:1994-2003. [Crossref] [PubMed]
- Brodaty H, Seeher K, Gibson L. Dementia time to death: a systematic literature review on survival time and years of life lost in people with dementia. Int Psychogeriatr 2012;24:1034-45. [Crossref] [PubMed]
- Seymour J, Almack K, Kennedy S. Implementing advance care planning: a qualitative study of community nurses’ views and experiences. BMC Palliat Care 2010;9:4. [Crossref] [PubMed]
- McMahan RD, Knight SJ, Fried TR, et al. Advance care planning beyond advance directives: perspectives from patients and surrogates. J Pain Symptom Manage 2013;46:355-65. [Crossref] [PubMed]
- van der Steen JT, van Soest-Poortvliet MC, Hallie-Heierman M, et al. Factors associated with initiation of advance care planning in dementia: a systematic review. J Alzheimers Dis 2014;40:743-57. [PubMed]
- Russell S. Advance Care Planning: Whose agenda is it anyway? Palliat Med 2014;28:997-9. [Crossref] [PubMed]
- Detering KM, Hancock AD, Reade MC, et al. The impact of advance care planning on end of life care in elderly patients: randomised controlled trial. BMJ 2010;340:c1345. [Crossref] [PubMed]
- McGlade C, Daly E, McCarthy J, et al. Challenges in implementing an advance care planning programme in long-term care. Nurs Ethics 2017;24:87-99. [Crossref] [PubMed]
- Sinclair JB, Oyebode JR, Owens RG. Consensus views on advance care planning for dementia: a Delphi study. Health Soc Care Community 2016;24:165-74. [Crossref] [PubMed]
- Caron CD, Griffith J, Arcand M. Decision Making at the End of Life in Dementia: How Family Caregivers Perceive Their Interactions With Health Care Providers in Long-Term-Care Settings. J App Gerontol 2005;24:231-47. [Crossref]