Understanding vomiting from the perspective of traditional Chinese medicine
Abstract: Vomiting is a common clinical symptom in which the conditions associated with impaired homeostasis and qi flow ascend reversely within the stomach, resulting in the expulsion of the stomach’s contents through the mouth. The stomach, located in the middle warmer (also known as Zhong Jiao), is primarily responsible for receiving and digesting food and liquid, and its qi typically flows downward. Various unfavorable conditions associated with the environment, food, mental health, or physiological stress can compromise the stomach, thereby leading to a loss of gastric homeostasis, which often triggers vomiting. However, regardless of external factors or internal weaknesses, the direct cause of vomiting is the loss of gastric homeostasis and the ascending qi flow. Traditional Chinese medicine (TCM) built its understanding of vomiting from the long-term accumulation of clinical observations and treatments, which were used to gradually improve and develop relevant theories, diagnoses, and treatments. This review paper presents vomiting from the nonaggressive perspective of TCM; specifically, we summarize TCM’s unique insights with regard to vomiting across various aspects including its etiology, diagnosis, locations, relationships with other organs, dialectical treatment, and drug and medical characteristics. By revealing the abundance of TCM’s theoretical and clinical knowledge concerning vomiting, we attempt to integrate Chinese and western medicines to treat it. In addition, the valuable knowledge that TCM provides with regard to vomiting certainly deserves better understanding to develop and improve modern medicine.
Key words: Traditional Chinese medicine; vomiting; etiology; pathogenesis; dialectical treatment; acupuncture
Introduction
Vomiting is a common clinical symptom that refers to the manifestation of impaired homeostasis and reversed upward qi flow within the stomach, resulting in the expulsion of the stomach’s contents through the mouth. Traditional Chinese medicine (TCM) practitioners generally differentiate nausea/vomiting into several categories. The Chinese word “Ou” (“vomiting” in English) refers to the condition associated with digested food being released and moaning, and the Chinese word “Tu” (“spewing” in English) refers only to the condition of releasing food. Alternatively, the Chinese word “Gan Ou” (“retching” in English) refers to neither condition. Because the definitions of first two words are difficult to distinguish, they are often collectively referred to simply as vomiting. Although retching has clearly distinct manifestations, it shares a similar diagnosis and treatment with the other two; therefore, it is combined into the broad concept of vomiting. The stomach, located in the middle warmer, is primarily responsible for receiving food and liquid, and its qi typically flows downward. Various unfavorable conditions associated with environment factors, food, mental health, or physiological stress can compromise the stomach, thereby leading to the loss of gastric homeostasis, which often triggers vomiting. Although the origin of vomiting lies in the stomach, the etiological root is traced back not only to the stomach but also to the liver and spleen. The balanced and descending flow of the stomach qi depends on the ascending and clearing transportation as well as the transformation of the spleen qi and the venting and free flow of the liver qi. Thus, if the spleen fails at healthy transportation, then the homeostasis of the stomach qi is disrupted and becomes unbalanced; likewise, if the liver fails at dispersion, then its qi exhibits chaotic movements, which also results in the loss of stomach homeostasis. Both scenarios can lead to vomiting. Based on its etiology, vomiting can be divided into two types: physical causes (e.g., environmental factors, diet, phlegm and fluid retention, and qi-stagnation) that affect the stomach, disrupt its homeostasis, and result in inverse qi flow and vomiting and intangible causes (e.g., qi deficiency, Yang deficiency, and Yin deficiency) that deprive the stomach of nurture, moisture, and maintenance, resulting in stomach qi deficiency, reverse flow, and eventually vomiting. In general, if a person has a weak spleen and stomach that are also compromised by an unhealthy diet, he or she will develop phlegm and eventually vomit; this pathway is the transformation from deficiency to excess. Alternatively, a person who is ill and vomits frequently over a long period might injure his or her spleen and stomach, resulting in a shortage of qi in the middle warmer; this pathway is the transformation from excess to deficiency. Individual patients often exhibit complicated and intertwined pathogenesis mechanisms between deficiency and excess. Nevertheless, whether external factors or a weak spleen and stomach affect the stomach, the basic pathogenesis of vomiting is the loss of gastric homeostasis and an inverse qi flow. Although many people intuit vomiting to stem from a compromised stomach and spleen, clinical observations have revealed other mechanisms (i.e., locations in other organs that affect the stomach). As such, although the direct cause of vomiting lies within the stomach, the ultimate root cause varies, as does its clinical manifestations. Hence, to differentiate pathogeneses, organ condition and situation are the keys of diagnosis. If vomiting results from areas in the stomach and spleen per se, then etiology can be determined via pathogenesis tracing to clarify the cold-fever and deficiency-excess conditions and to treat the disease via both eradicating the root cause as well as ameliorating the symptoms from serious to mild. On the other hand, if vomiting results from other damaged organs (i.e., not the stomach), then the pathogenic source and route should be clarified so that the root cause can be treated.
TCM’s definition and diagnosis of vomiting
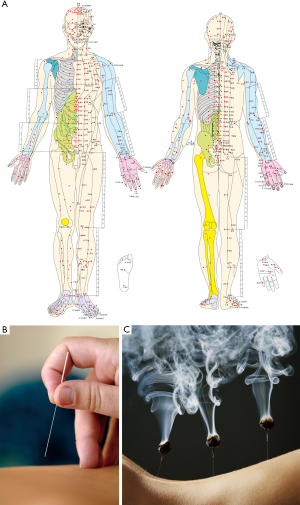
Yellow Emperor’s Inner Classic comprehensively and systematically describes the relationship between humans and nature via theories of human physiology, pathology, diagnosis, treatment, disease prevention, and health maintenance (Figure 1A). Hence, this work lays the foundation for the development of TCM. Yellow Emperor’s Inner Classic presents detailed records of vomiting. In fact, the book is the first medical literature to use the word “vomiting”. As stated in Suwen (Plain Questions: treatise on Pulse Interpretation), vomiting is the condition that occurs after eating in which food fills and overflows from the stomach (1). At the end of the Eastern Han Dynasty of China, Zhang Zhongjing compiled two milestone works: treatise on Cold Pathogenesis and Miscellaneous Diseases and Essential Prescriptions of the Golden Coffer (Figure 1B). These works were based on his inheritance of ancient medical literature, including Inner Classic, and incorporated knowledge of the medical community at the time as well as his personal experience. The former book examines diseases associated with the common cold across six divisions and examines other miscellaneous diseases using organ status. Thus, he comprehensively implemented the diagnosis principle that includes reason, methodology, prescription, and medication. As such, this book marks the formation of the TCM clinical diagnosis system. This book categorizes vomiting into many types including retching, vomiting, the desire to vomit, intense vomiting, vomiting and reverse stomach movement, vomiting and diarrhea, spewing pus and blood, spewing foamy saliva, spewing roundworm, and stomach reversal. These individual conditions are also specified with regard to patients’ feelings, vomiting timing, associated symptoms, and characteristics of the released content. For example, retching refers to the condition that compels a patient to vomit, although they cannot. Stomach reversal refers to patients who eat and then vomit, which persists and results in indigestion. Spewing pus and blood refers to expulsion of blood that contains pus. Spewing foamy saliva refers to a condition in which patients have a tremendous amount of saliva in their mouths or vomit foamy saliva. Spewing roundworm refers to expulsion of parasitic worms. The subsequent TCM community has accepted this classification.

Vomiting versus stomach reversal
Both vomiting and stomach reversal are gastric diseases with etiologies of impaired gastric homeostasis and ascending qi flow. Moreover, both conditions display clinical manifestations of food expulsion. However, stomach reversal stems from spleens and stomachs that are weak and cold. Furthermore, there is a deficiency of qi and stomach fire, which renders this organ incapable of digesting food and leads to a persistent condition of eating followed by expulsion. Often, patients do not feel at ease until all of the contents of their stomachs are released (2). In comparison, vomiting is characterized by moaning and content release and is caused by the inversely ascending flow of stomach qi. This disease has roots such as unfavorable environmental factors, diet, mental health, and a weak stomach. These factors are easy to differentially diagnose.
Vomiting versus dysphagia
Vomiting and dysphagia both display symptoms of expulsion. However, the former condition is characterized by normal eating and random expulsion, whereas the latter condition describes intense difficulty with swallowing such that swallowing must be forced or food will not enter the esophagus or will be rapidly expulsed. As a consequence, the patient must give up eating. As stated in Volume IV of Comprehensive Medical Knowledge by Zhao Xianke, “Those who suffer dysphagia are hungry and want to eat; however, they are affected by swallowing difficulties between the throat and diaphragm just above the stomach. Before food can enter the stomach, the patient expulses phlegm and saliva” (2). In addition, vomiting is generally a mild condition with a short course and good prognosis, whereas dysphagia often results from internal injuries; thus, the latter condition has severe symptoms, a long course of disease, and poor prognosis.
Identification of vomit content
Vomiting symptoms can be divided into cold, fever, deficiency, and excess categories that can be verified according to the traits and odor of its content. If the content has high level of acidic, decayed material with an unpleasant smell, the patient likely suffers from stagnant digestion, resulting in rotten food in the stomach. If the vomit is a bitter, yellowish fluid, then the patient likely suffers from bilious fever, which has damaged stomach and resulted in the loss of homeostasis. If the vomit contains acidic, greenish fluid, the patient likely suffers from a liver fever that has compromised the stomach and led to an inverse ascending qi flow. If the vomit comprises turbid phlegm and saliva, then the patient likely suffers from phlegm and fluid retention that blocks food processing and results in qi counter flow. If the vomit contains clear fluid, the patient likely suffers from a weak and deficient stomach qi that cannot successfully process and digest food.
The pathogenesis of vomiting
Inner Classic argues that the pathogenesis of vomiting lies in the excessive heat of an inversely ascending yang qi. As stated in Plain Questions: treatise on Great Theories with Real Importance, “excessive yang heat, compounded by a massive flow of clear qi, results in bitter vomit” (1). The general cause of this symptom is the loss of gastric homeostasis and an inversely ascending qi flow. Its pathogenic manifestation can be either excessive or deficient. Unfavorable external factors, stagnant digestion, phlegm and fluid retention, and a liver qi that damages the stomach and blocks the stomach qi cause the excessive type. This condition leads to a dysregulation of qi, an inversely ascending qi flow, and eventually vomiting. A weak stomach with excessive yin causes the deficient type. Consequently, the stomach suffers from poor functionality and impaired homeostasis. This type can be further divided into yin-deficient and yangdeficient subtypes. In general, excess primarily characterizes the early stages of the disease; however, if the patient subsequently experiences protracted vomiting that damages and weakens the stomach, then its state can be transformed from excessive to deficient. Alternatively, some patients have long histories of deficient, weak stomachs, which can generate mixed symptoms if continually injured by liquids and food.
Inner Classic suggests that both external enervation and internal injuries can lead to vomiting. As such, its causes can include unfavorable environmental factors or inappropriate medications. In addition, vomiting might also be caused by unhealthy diets and poor mental health.
Six excesses (six climatic pathogenic factors: wind, cold, summer heat, dampness, dryness, and fire/heat)
The six factors above can each cause vomiting if they infringe upon the stomach. Specifically, if a person is compromised by any of these factors or breathes an unhealthy atmosphere, his or her stomach and other organs can be affected, resulting in the loss of gastric homeostasis and followed by the inversely ascending qi flow that propels the stomach contents out. Due to seasonal variations, these factors can be different. Nevertheless, the dominant climatic factor for vomiting is cold.
Wind is the leading cause of many diseases and the most common factor that attacks people. TCM theory considers wind to be a yang pathogenic factor that is light and ascending and often strikes yang sites. In addition, wind is fluid and volatile; therefore, it easily damages yang sites because the stomach resides in the middle warmer and is a yang site that accommodates a tremendous flow of qi and blood. Therefore, it is vulnerable to wind attacks in affected people. Vomiting can develop as a consequence. As stated in Plain Questions: treatise on Great Theories with Real Importance, vomiting often follows eating wherever wind prevails (1).
Cold is a yin pathogenic factor and has a tendency to damage yang qi. This factor can harm the yang elements in the stomach. The initial symptoms include vomiting, diarrhea, and abdominal cold and pain. Subsequently, the patient may experience various deficient conditions related to cold such as anorexia, cold extremities, and fatigue. Cold is characterized by its slow and stagnant nature; if cold invades the human body and damages the yang qi, meridian blood is unable to warm the yang qi. As a consequence, patients primarily suffer from pain. Hence, as stated in Plain Questions: treatise on Pain, cold qi can penetrate into the intestines and stomach where it ascends to cause pain and vomiting (1).
Summer heat is a yang pathogenic factor characterized by torridness. This factor has ascending and dispersal properties and easily damages body fluid and consumes qi. In addition, because summer heat is often associated with humidity, if this factor (which injures yang) affects a person, then he or she may develop vomiting and irritability. As stated in Plain Questions: treatise on Great Theories with Real Importance, people may experience vomiting and impatience when a hot summer arrives (1).
Dampness is a yin pathogenic factor that is prone to block qi movement and damage yang qi, thereby wetting and hindering the middle warmer as well as leading to aberrant qi movements in the spleen and stomach. As a consequence, patients lose their appetite and suffer from abdominal swelling and difficult defecations as well as vomit translucent fluid. As stated in Plain Questions: treatise on Great Theories with Real Importance, dampness can cause conditions of obesity and poor digestion, which lead to frequent vomiting and the spewing of translucent saliva (1).
Dryness is associated with rough skin and is prone to damage bodily fluids. This pathogenic factor often harms people via their oral and nasal openings and is most likely to injure “lung fluid”, thereby compromising the descending movement of the lung qi. Because the lungs and stomach share a meridian connection and a downward qi flow, patients may vomit if their bodies are damaged by dryness. As stated in Plain Questions: treatise on Great Theories with Real Importance, people suffer intense vomiting and release bitter contents when dryness dominates (1).
Fire/heat is a yang pathogenic factor with the properties of burning and rising. The diseases caused by this factor often affect the head. As stated in Plain Questions: treatise on Great Theories with Real Importance, internal fire/heat results in oral ulcers and vomiting; when fire/heat strikes, a person becomes ill and vomits. Various conditions of inverse ascending flow are related to fire/heat (1).
Improper medications or diet (e.g., consuming bitter, cold, and stomach-weakening materials) can also lead to vomiting
Unhealthy dietary habits such as overeating and hyperphagia as well as the frequent consumption of raw, cold, alcoholic, spicy, sweet, fat, and unclean foods cause vomiting because they damage the stomach and slow its contraction. Each of these habits can cause indigestion and ascending (rather than descending) stomach qi flows, which lead to vomiting.
Five flavors can be grouped into yin and yang categories. Those that are pungent and sweet belong to yang, whereas those that are acidic and bitter as well as those that stimulate expulsion and excretion belong to yin (Plain Questions: treatise on Great Theories with Real Importance). Each flavor has distinct functions and yin-yang properties and is necessary for human life. In addition, each of the five flavors individually enters the five organs and has specific effects on them. If a person has a long-term addiction to a drug with a particular flavor, then he or she may suffer from dysfunctions in organs relevant to that flavor. If the condition persists, then it can spread to other organs and cause diseases because of the mutual restrictive nature of the five organs. In addition, bitterness can promote dryness within the body; however, the stomach can only function well with sufficient water content. As such, bitterness often damages the stomach yin, resulting in reversely ascending qi and vomiting. As stated in Miraculous Pivot: treatise on Five Flavors (the 63rd essay), “the Yellow Emperor said, ‘Bitterness can penetrate into bones; if a person consumes too much, then he or she may vomit. Why?’ Shaoyu responded, ‘Bitterness enters the stomach. Because no food ingredient can overcome bitterness, it migrates to the lower abdomen and blocks various passages connected to the triple warmer, which initiates vomiting’.” (3). Hence, if a person takes drugs or consumes improper food, then he or she may suffer from a damaged spleen and stomach and possibly vomit. This internal, harmful factor leads to vomiting.
Emotional maladjustment and post-illness debility
Various mental and physiological events can cause vomiting. For example, when a person experiences intense anger, he or she may also experience impaired liver functionality that subsequently affects the stomach and promotes reversely ascending stomach qi. In addition, when a person experiences sadness and anxiety, he or she may suffer from dysfunctional spleen transportation; subsequently, he or she may suffer from food stagnation and develop digestive difficulties, thereby disrupting gastric homeostasis. Both scenarios can lead to vomiting. Furthermore, food processing becomes poor and stagnant when a person has a deficient spleen and stomach and poor digestion. Occasional anger can propel food to reverse the flow of qi and result in vomiting. In another example, when a person suffers from a long-term spleen and stomach deficiency or exhibits a postillness debility and is tired from excessive labor, the person might develop a deficient stomach that fails to take in food and fluid as well as a weak spleen that cannot perform digestion, thereby damaging the medial qi. Subsequently, the food in the stomach is expelled.
Zhang Zhongjing elucidated the causes of vomiting based on theories from Inner Classic. He argued that the causes of vomiting include unfavorable external factors that infringe on the stomach, excessive heat in the stomach and intestines, a deficient and cold spleen and stomach, hindrance caused by phlegm retention, incorrect or missed treatment, and roundworm infestations. These pathological factors either function individually or together to damage the stomach, which initiates upward counter flow of qi and results in vomiting. If the etiology of vomiting in Treatise on Cold Pathogenesis is analyzed from the perspective of deficiency/excess, vomiting can be examined by dividing cases into those with excessive symptoms and those with deficient symptoms (Table 1).
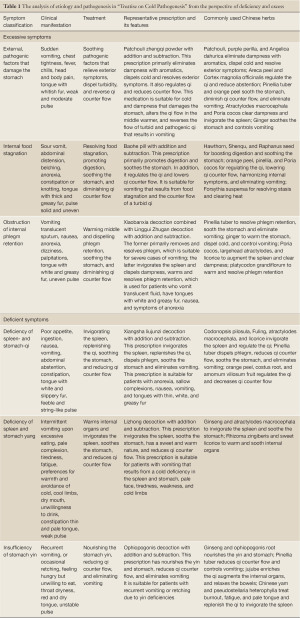
Full table
Origins of vomiting
Inner Classic argues that the primary origins of vomiting are in the spleen and stomach, and these areas are closely associated with other organs including the liver, gallbladder, heart, lungs, kidneys, and large and small intestines.
The spleen and stomach are located in the middle warmer and are connected via a membrane. The meridian of foot-taiyin originates in the spleen and reaches the stomach; conversely, the meridian of foot-yangming stems from the stomach and connects to the spleen. These organs, which are located in the same region, constitute a closely coordinated pair that is responsible for processing food and liquids. External and internal injuries can lead to disorders within these organs and trigger vomiting. Therefore, the major origins of vomiting reside in the spleen and stomach. As stated in Miraculous Pivot: meridians, the meridian of foot-taiyin flanks the throat, connects to root of the tongue, and lies underneath the tongue. Its branches stem from the stomach, pass through the diaphragm, and join the heart. Its dislocation damages the root of the tongue, which can result in vomiting if forced swallowing is attempted. These patients suffer from abdominal pain, distension, and frequent belching (3).
The liver controls material discharge and adjusts qi movement. It also coordinates the vertical movements of the spleen and stomach, supplies ingredients for bile, and assists in delivering bile to the intestines. As such, the liver promotes the digestive mechanisms that absorb beneficial contents and remove harmful compounds. If the spleen qi is robust and functions normally, then nutrients are abundant and can support the generation and transportation of qi and blood. As a consequence, the liver is fully nourished; therefore, the liver qi is mild, in harmony, and well circulated. However, if the liver discharge is clogged, then the liver qi can invade the stomach and disrupt its homeostasis. Vomiting, expulsing acidic fluid, and nausea can follow this event. If the gallbladder is ill, then patients might experience bitter tastes and vomit stomach fluid. As stated in Miraculous Pivot: meridians, “The liver meridian of the foot-jueyin... is the primary site of liver diseases. Patients with this condition have congested chests and may vomit” (3). In addition, Miraculous Pivot: Manifestations of Diseases caused by Evil Qi in the Viscera states, “those who suffer from gallbladder diseases often sigh, experience bitter tastes in their mouths, and vomit stomach fluid” (1).
The heart controls blood flow, whereas both the spleen and stomach are rich in blood and qi. The heart is an organ associated with fire: “When fire strikes, a person becomes ill and vomits” (1). If a stagnant heat characterizes heart activity, then the heart contains an intense fire whose internal spread can promote the yang and brightness of the stomach. As a consequence, the stomach qi reverses and triggers vomiting. As stated in Plain Questions: treatise on Needling Heat Diseases, a patient who suffers from heat in the heart displays anguish and often vomits (1).
The spleen and stomach both belong to the earth. The spleen and kidney are involved in the metabolism of food and liquids. On the one hand, the kidney manages two types of excretion for the stomach. The kidney can only operate properly when it has sufficient qi and a normal qi flow. Subsequently, digestive waste is released from two yin openings. On the other hand, because the spleen belongs to the earth, whereas the kidney belongs to water, spleen earth can restrict the flow of renal water. Hence, if the earth is deficient, then water prevails. Subsequently, the change of contaminated water affects the spleen and stomach, resulting in vomiting. As stated in Plain Questions: treatise on Reversal, a Shaoyin coldness of the extremities signifies a high deficiency; consequently, people may vomit (1).
The lung and stomach are connected via meridians and have several aspects in common. The qi in both organs typically exhibit a descending flow. Both organs prefer moist rather than dry environments. They display physiological interdependence and are synergistic. The lungs primarily control air dispersal to promote circulation and detoxification. Hence, they spread essence, qi, and bodily fluids that nourish the stomach. The stomach is responsible for receiving and processing food, and it cooperates with the spleen in digestion. Subsequently, the stomach produces qi, blood, and bodily fluids that nourish the lungs. Hence, there are many interactions between these organs under pathological conditions. As stated in Plain Questions: treatise on Reversal, if a person displays the coldness of hand-taiyin, then he or she often vomits foamy matter (4).
Hence, the origins of vomiting are not restricted to the spleen and stomach but are closely related to other organs.
Determining a treatment for vomiting based on the Five Viscera (Zang-fu) Theory
The treatment of vomiting is based on the Five Viscera Theory. Historically, TCM practitioners have investigated the mechanism of the visceral origins that cause vomiting and the corresponding treatments and prescriptions. These studies, which are described below, have examined the kidneys, lungs, and liver.
Kidney-based treatments
There are congenital and acquired relationships between the kidneys as one unit and the spleen and stomach as another. When there is inadequate kidney yin, the stomach loses its moist and soothing environment, which results in a persistent qi counter flow and vomiting. If there is insufficient kidney yang, or the kidneys have weak fire, then the spleen becomes cold and is unable to assist proper food processing, which leads to indigestion. The undigested food aggregates to generate sputum, phlegm retention, water, and moisture, each of which can block the middle warmer. Subsequently, the loss of gastric homeostasis and ascending qi can induce vomiting. Xu Huiwu et al. (5) investigated kidney-based vomiting treatments and argued that those who experience long-term recurrent post-illness vomiting should adopt kidney-based methods. This approach has been widely used to treat the vomiting associated with post-chemotherapy side effects, uremia, heart failure, Meniere’s syndrome, postpartum complications, chronic illnesses of the elderly, and those who are pregnant. A kidney-yin deficiency is common among patients with fever, chronic illnesses, yin damage due to postpartum blood loss, and chemotherapy. Kidneyyang deficiency is often found in patients with uremia, heart failure, chronic yang deficiency, and those who are pregnant. Kidney treatments should employ drugs that nourish and recuperate kidney yin and yang. Li Rui (6) treated patients who vomited a clear, thin liquid immediately upon ingestion (including water) and displayed the following symptoms: pale complexion, shortness of breath and fatigue, slight swelling throughout the body, mental malaise, cold hands and feet, pale tongue with whitish fur, and a weak pulse. He achieved a successful outcome by replenishing their kidney yang.
Lung-based treatments
The lungs control qi and purify air; thus, they play a dominant role in adjusting qi flow. The qi throughout the body remains stagnant when the lungs lose their purification ability. As such, treatment of the qi begins by curing the lungs. Hence, lung-based stomach treatments for vomiting aim to adjust qi flow and maintain normal circulation, thereby recovering stomach qi. Li Xincun (7) used symptom differentiation strategies of “nurturing metal to control wood” and “clearing the lungs to satisfy the stomach” to treat patients who developed vomiting due to depression and rage. In addition, he used the approaches of “purging the lungs to remove heat” and “suppressing reverse qi flow to stop vomiting” and achieved impressive efficacy. Similarly, Liu Xiangdong (8) used a lung-based strategy to treat a patient who experienced vomiting, abdominal distention, bowel sounds, and constipation for two months. After changing doctors several times, the patient showed little (if any) improvement. The vomiting worsened such that eating anything would lead to vomiting. The patient also had a dry and bitter mouth, chest tightness, a weak pulse, and slightly greasy white tongue fur. Dr. Liu diagnosed the condition as middle deficiency, stagnant qi, and aberrant qi flow; correspondingly, he decided to ventilate the lungs to adjust the qi flow and invigorate the spleen to promote digestion. The prescription was composed of apricot seeds, fried burdock, desiccated tangerine peel, grilled aster, heterophylla, bighead atractylodes rhizome, fried Fructus aurantii, Poria, Pinellia ternate, and grilled loquat leaves. After three oral administrations, the vomiting lessened; after another two administrations, the disease was fully cured. The turbid qi ascended to trigger vomiting because the patient had middle deficiency, impaired circulation, and constipation. As such, the lung-ventilation method was used to clear the organs and reduce turbidity. This method resulted in a recovery of qi, although this outcome was not specifically targeted.
Liver-based treatments
The liver is a bold and firm organ that tends to stagnate and culminate in a fire that spreads to the stomach. Alternatively, the gallbladder qi attacks the stomach and disrupts its homeostasis. Either case can cause vomiting. Thus, an important principle of treating vomiting is to start at the liver to reach the stomach, thereby recuperating the liver and diminishing the qi counter flow in the stomach. This treatment is particularly suitable for patients with known internal injuries. For example, Cao Huibo (9) treated a patient with strong liver activity and excessive liver qi in the spring. This patient had a history of a deficient and cold middle warmer. As a consequence, cold air in the jue yin mixes with moisture and stimulates vomiting. Correspondingly, Evodia rutaecarpa liquid extract was used to warm the liver, soothe the stomach, and diminish the qi counter flow. The following prescription has resulted in satisfactory outcomes for those whose vomiting is accompanied by a throat sound resulting from liver qi stagnation and ascending moisture and heat: low doses of coptis and Chinese thorowax root (bupleurum) to disperse stagnant (Yu) fire, sweet basil, and schizonepetae (the last two are both pungent, sweet, and aromatic) to clear the lung qi to facilitate circulation of the liver qi and balance the stomach qi. In addition, Zhang Zhengxue (10) argued that many clinical cases of vomiting have resulted from ascending qi flow in the liver and gallbladder, which causes a counter flow of stomach qi and triggers vomiting; thus, liver-based treatments are prescribed. As such, he used a base prescription that consisted of Chinese thorowax root, red ochre, Chinese yam, chicken gizzard membrane, and magnolia bark. These ingredients were supplemented and subtracted to treat 30 vomiting patients and generated successful outcomes.
Other treatments
Other treatments of vomiting include phlegm-based treatments, stomach-qi-based treatments, and bitter and sweet ingredients to diminish and sooth symptoms, respectively, as well as augmenting the gallbladder to soothe the stomach and boosting clearness to curb turbidity. These methods enrich the therapeutic content of vomiting treatments.
Chinese herbal vomiting treatments
Single-herb drugs to treat vomiting
Single-herb drugs are simple, convenient, have specific activities, and generate potent effects. Thus, TCM professionals often use them. Studies have been performed on the drugs used to treat vomiting and symptom-oriented drug compatibility techniques (Figure 2A).
Pseudo-ginseng
Pseudo-ginseng refers to the desiccated roots of the araliaceae plant, Panax notoginseng (Burk), also known as notoginseng. This plant has a variety of effects including nourishment, invigoration, blood enrichment, swelling reduction, pain alleviation, hemostasis, and weakness removal. Yin Wenxu et al. (11) used this herb to treat concussion-induced vomiting. The drug was orally administered with a water decoction of 10 g of pseudoginseng; it consistently achieved outstanding efficacy. On the other hand, if this decoction was applied to those with other symptoms, no effects were found among many patients. These results indicate that pseudo-ginseng is only effective for concussion-resulted vomiting.
Ginger
Ginger refers to the fresh rhizomes of the ginger plant (zingiber of officinale rosc) that is cultivated in most regions of China. This herb has pungent and warm properties and relieves exterior symptoms, dispels cold, warms internal organs, cures vomiting, promotes water movement and detoxification, removes phlegm, and resolves coughing. Numerous experiments have demonstrated that ginger has significant antiemetic effects. For example, Zhang Laiyin (12) applied acetone-ginger extract to rats to investigate its antiemetic activity. He found that this herb is particularly effective at curing motion sickness. Thus, ginger has remarkable success at treating sports-related vomiting. Using a mink model, Zhao Dexue et al. (13) examined the effect of ginger extract on vomiting. He found that ginger juice and alcohol extract have antiemetic effects on the vomiting caused by cisplatin, copper sulfate, and motion sickness. This result suggests that ginger is a valid reagent for chemotherapy and motion-sickness-resulted vomiting. Its mechanism may be associated with 5-HT3 receptors and Substance P.
Acorus gramineus rhizome
Acorus gramineus rhizome is the desiccated rhizome of the araceae plant, Acorus gramineus (schott). It has pungent and mild warmth properties and is absorbed by meridians of the heart, liver, and spleen. This herb has the effects of resuscitation, phlegm elimination, qi regulation, and moisture removal. It is commonly used in the clinical treatment of various conditions including epilepsy, phlegm stagnation fainting, coma fever, amnesia, and pain in the heart and chest. Zhang Zesheng (14) used the Acorus gramineus rhizome to treat 21 patients with nervous vomiting. The results showed that 15 patients displayed improvement, five patients were cured, and one was an invalid. One patient suffered for two months from upper abdominal discomfort and vomiting after eating. This patient was admitted to the hospital and diagnosed with “nervous vomiting”. Two months ago, this patient experienced poor mental health, anxiety, and insomnia and subsequently developed a tight chest and upper abdominal distension. The patient had extreme difficulty swallowing when eating and complained that his throat was being clogged. This patient displayed vomiting after eating, and other symptoms appeared after vomiting. The patient was diagnosed with disharmony of the liver and stomach, entrapment of moisture, and turbidity. Thus, the patient was prescribed 15 g of Acorus gramineus rhizome, which was twice decocted with water to create a 500-mL water extract. Ten aliquots of the water extract were orally administered within one day. The symptom eased three days into the treatment. After another two days of the regimen, the vomiting completely stopped, and the accompanying symptoms mostly disappeared. The symptoms did not reoccur after two weeks of post-withdrawal observation. The specific decoction procedure is as follows: 10-20 g/day of Acorus gramineus rhizome is ground and covered with gauze. Approximately 500 mL of water is added, and the preparation is boiled over a small flame for 15 minutes to generate the water extract. The regimen employs small aliquots and 10-30 daily oral administrations to prevent drug denial and vomiting as well as promote its slow absorption in the stomach. It is important to be cautious when prescribing this drug to those who have deficient yin, excessive fire, or dissipative heart qi.
Pinellia tuber
This herb is the tuber of the araceae plant, Pinellia ternata (Thunb) Briet. It is warm in nature, has a pungent flavor, and is toxic. This herb is absorbed by the meridians of the spleen, stomach, and lungs and removes moisture, clears phlegm, suppresses qi counter flow, eliminates vomiting, dissolves distension, and removes stagnation. Studies (15) have shown that the Pinellia tuber can activate the efferent activities of the vagus nerve, thereby suppressing vomiting. In addition, this herb can significantly increase the minimum emetic dose of apomorphine in cats and inhibit the emetic effects of copper sulfate and apomorphine in dogs. Its active ingredients are water-soluble glycoside and water-soluble glucuronic acid derivatives. Several animals, including pigeons, dogs, and cats, were orally or subcutaneously administered with various Pinellia tuber preparations in a study of the herb’s effects. The results showed that these herbs effectively suppress the vomiting induced by apomorphine, digitalis, and copper sulfate, and its active ingredients are the alkaloids phytosterols and L-ephedrine (16). Wu Hao et al. (17) examined the effects of the Pinellia tuber on gastrointestinal movement and found that preparations of ginger, alum, and Pinellia tuber as well as boiled ginger and Pinellia tuber slowed gastrointestinal motility when administered via gavage, although they had no noticeable influence on the contents of pepsin and PGEZ nor did they significantly damage the gastric mucosa. This result indicates that incorporations of ginger in Pinellia tuber preparations not only eliminate the stimulation of the Pinellia tuber on the gastrointestinal mucosa but also antagonize the accelerated gastrointestinal motility induced by this herb that leads to vomiting and diarrhea. As such, these preparations pacify the stomach, reverse qi counter flow, and stop vomiting.
Forsythia fruit
This herb is the desiccated fruit of the oleaceae plant, Forsythia suspensa (Thunb) Vah1. It has a bitter taste and a slightly cold nature. Forsythia fruit is absorbed by the meridians of the lungs, heart, and small intestine. It has effects of heat reduction, detoxification, and detumescence. Modern pharmacological studies (18) have shown that forsythia fruit decoctions exhibit similar antiemetic effect to that of chlorpromazine injections (2 hours after the injection). This herb inhibits the vomiting in dogs caused by the subcutaneous injection of apomorphine. These results prompted speculation that its antiemetic mechanisms are associated with the inhibition of the central chemoreceptive area in the medulla oblongata. He Yunqiang (19) found that forsythia fruit positively treats all types of vomiting when its administration followed the clinical practice of treatment with symptom differentiation. For patients with neurogenic vomiting, the water decoction of 60-g forsythia fruit produced a significant antiemetic effect. If symptomdifferentiation- based treatments fail to deliver the desired outcome among patients who vomit after eating, then the original prescriptions should be supplemented with forsythia fruit to achieve the desired effect that is consistent with its antiemetic pharmacological role.
Lemon
This herb refers to the fruit of the woody rutaceae plant, lemon (Citrus burm), which is cultured in Guangdong. It tastes extremely sour. This herb generates fluid, soothes thirst, alleviates summer heat, and calms fetuses. Long Shuzhen et al. (20) investigated the antiemetic effects of lemon by randomly dividing 180 vomiting patients into three groups that each contained 60 individuals and equal numbers of males and females. The control group was intramuscularly injected with metoclopramide, the lemonpeel group was treated with the smell of the peel fluid produced by cutting the peel and squeezing it, and the lemon-juice group received either a buccal treatment or an oral administration of the juice. The results showed that the smell of lemon peel generated the best antiemetic effects among the three treatments. Chen Weiyue (21) randomly sampled 50 patients who had undergone Caesarean sections and vaginal deliveries and treated them with lemon to prevent postoperative nausea and vomiting. In addition, another 50 cases were randomly chosen to form the control group, thereby creating a comparison to the postoperative nausea and vomiting of the study group. The results revealed that the study group exhibited significantly reduced vomiting symptoms, which were different from those of the control group (P<0.05). This result indicates that lemon can combat postoperative nausea and vomiting.
Katsumada seed
This herb is the seed mass of the zingiberaceae plant, Alpinia katsumadai Hayata. It removes moisture, augments the spleen, warms the stomach, and suppresses fluid generation. Correspondingly, it is used to treat various internal conditions including the retention of cold/ dampness, abdominal distension, cold pain, belching, vomiting, and anorexia. A study (22) examined the antiemetic ingredients of katsumada seeds that were separated into five compounds. Specifically, katsumada seeds were extracted successively using hexane, chloroform, and methanol. The resulting extracts were tested for antiemetic effects via intraperitoneal injection and subsequent oral administrations of copper sulfate, an emetic agent. Retching was induced within 10 min after administration. This result was compared with that of the control group. The results showed that the chloroform and methanol extracts of katsumada seeds reduced the frequency of retching; the five antiemetic active compounds were tentatively designated SOUZUKU-3, 4, 5, 6, and 7.
Chinese clematis
Chinese clematis refers to the roots and rhizomes of several plants, namely Clematis chinensis Osbeck, Clematis hexapetala Pall, and Clematis mand-shurica Rupr. This herb counters wind/ dampness, clears meridians, eliminates sputum, and removes weakness. Correspondingly, it is used to treat gout, obstinate arthralgia, and cold/pain in the waist and knees. Zhang Jiaoke et al. (23) used Chinese clematis to treat the vomiting induced by radiotherapy and chemotherapy. Specifically, 50 g of Chinese clematis and 300 mL of water were mixed to produce a 150-mL decoction of mild fire after the dregs were removed. This process was repeated to produce another 150-mL decoction, which was combined with the previous one. The 150-mL preparation was orally administered in the morning and evening on an empty stomach. One or two administrations sufficiently relieved symptoms. Of the 120 patients treated, the efficacy rate was over 90%.
Rhizoma alpiniae officinarum
This herb, also known as the galangal rhizome, refers to the desiccated rhizomes of the alpinia plant, Alpinia officinarum Hance. It has a hot and pungent taste. This herb is absorbed by the meridians of the spleen and stomach and warms the stomach, dispels cold, digests food, and relieves pain. Therefore, clinical galangal rhizome is often used to treat conditions that include abdominal cold/pain, gastrofrigid vomiting, belching, and acid reflux. Based on the therapeutic effects of the galangal rhizome, Chen Dian (24) established an analgesic mouse model and an antiemetic pigeon model through which various galangal rhizome chemical extracts (e.g., aqueous, alcohol, volatile oil, and water extractions of the ethyl acetate extract, and alcohol extraction of ethyl acetate extract) were screened. The results showed that all galangal rhizome extracts displayed the dual analgesic and antiemetic pharmacological effects and that its primary active ingredients are galangin and kaempferol.
Chili pepper
Chili pepper refers to the ripened fruits of the solanaceae plant, Capsicum frutescens L. It is pungent and hot and is absorbed by the meridians of the heart and spleen. This herb has pharmacological effects of warming the internal organs, dispelling cold, stimulating appetite, and boosting digestion. Correspondently, it is used to treat the abdominal pain resulting from cold accumulation, vomiting, diarrhea, frostbite, and scabies. The major antiemetic component in chili peppers is capsaicin. Yang Zhihong et al. (25) investigated the antiemetic effects of chili pepper and showed that extract of capsaicin (Ec) suppresses cisplatin-induced allotriophagic vomiting in rats (P<0.05). This effect was sustained for a long duration, and its antiemetic mechanism most likely lies in the blockage of Substance P and its cognate receptors. In addition, Ec also effectively inhibits the vomiting in rats caused by apomorphine and mechanical rotation (P<0.05), which indicates that it fundamentally achieves an antiemetic effect by inhibiting the central CTZ. Furthermore, their study also revealed that the rats of the Ec Group displayed a substantial increase in food intake (P<0.05), which suggests that Ec can alleviate gastrointestinal discomforts such as anorexia and nausea in rats.
Patchouli
Patchouli refers to the whole herb of the labiatae plant, Pogostemon cablin Blanco. It is pungent and mildly warm and is absorbed by the meridians of the spleen, stomach, and lungs. This herb is aromatic, dispels turbidity, boosts appetite, eliminates vomiting, boosts sweat, and relieves summer heat. As such, it is used to treat various conditions including the stagnation of cold/damp in the middle warmer, the removal of uncomfortable fullness in the stomach, vomiting, heat- and moisture-induced lassitude, chest tightness disorder, cold/dampness resulting from heatstroke, abdominal pain, diarrhea, nasosinusitis, and headache. An experiment (26) found that hexane, chloroform, and methanol extracts of patchouli diminished the frequency of retching in pigeons. In addition, antiemetic activity indicated that silica-gel-column chromatography (hexane-acetic acid ethyl ester) refined the hexane extract. One of the active substances of patchouli is alcohol.
Ancient prescriptions to treat vomiting
In Treatise on Cold Pathogenesis and Essential Prescriptions of the Golden Coffer, Zhang Zhongjing listed 29 prescriptions associated with vomiting: mahuang (ephedra) decoction to boost sweat and relieve exterior symptoms; cassia twig decoction to harmonize yingfen and weifen, sooth muscles, and relieve exterior symptoms; decoction of kudzu root and Pinellia tuber to boost sweat, relieve exterior symptoms, suppress qi counter flow, and eliminate vomiting; xiaoqinglong decoction to warm and clear fluid retention; wuling powder to clear qi and induce diuresis; poria and alisma decoction to fortify the spleen and induce diuresis; shizao decoction to purge excessive fluid retention; zhenwu decoction to warm the kidneys and induce diuresis; evodia decoction to warm the liver and stomach, suppress qi counter flow, and eliminate vomiting; sini, tongmai sini, baitong, and baitong with porcine bile decoctions to warm the yang to dispel cold and revive the yang to resuscitate; lizhong decoction to warm internal organs, fortify the spleen, and eliminate vomiting; gardenia, ginger, and bean decoctions to expel heat to stop vomiting; tiaowei chengqi, xiao-chengqi, and da-chengqi decoctions to discharge heat and free the bowels; zhuye shigao decoction to clear stomach heat; xiao-chaihu decoction to harmonize shaoyang; da-chaihu decoction to develop pivot and clear evil heat; zhuling (Polyporus umbellatus) decoction to clear heat, induce diuresis, nourish the yin, and moisten dryness; Pinellia tuber xiexin, ginger xiexin, and licorice xiexin decoctions to clear heat, induce diuresis, acrid opening, and bitter descending (all of which are suitable for cold and warm conditions); ganjiang (Rhizoma zingiberis)-sulian-ginseng decoction to clear upper and warm lower organs as well as reconcile cold and dryness; Coptis chinensis decoction to clear upper and warm lower organs as well as reconcile internal organs and regulate the stomach; scutellaria decoction combined with Pinellia tuber and ginger to clear heat and control vomiting; and wumei pill to treat ascariasis-related biliary tract syndrome. These prescriptions are precise and appropriate and have reliable curative effects; thus, TCM professionals have preferred them through the ages, and they currently have tremendous clinical importance (Figure 2B,C).
External treatments and vomiting
Acupuncture and moxibustion
Acupuncture and moxibustion treatments of vomiting have a long history. Over the past centuries, Western medicine has been developed and extensively integrated with TCM in China. As a consequence, the theories and technologies of acupuncture and moxibustion have been validated and developed as well as rapidly expanded internationally. In addition to traditional acupuncture therapies, novel derivatives that incorporate a variety of modern technologies and devices have been developed such as scalp, auricular, electro-, and wrist-ankle acupunctures, the application of which have made impressive achievements with regard to treating vomiting (Figure 3A,B,C).
(I) Symptom-differentiation-based treatments
Huang Dianjun (27) divided vomiting patients into four groups to apply a symptom-differentiation-based treatment. The treatment protocol is described below. The major acupoints included Zhongkui, Zhongwan, Zusanli, Neiguan, and Gongsun; the needling treatment adopted the even reinforcing and reducing method with 20-30 minutes of retention. After inserting the needle to facilitate the arrival of qi, a moxa-stick moxibustion was always performed. (i) For patients who suffered from stomach heat, thirst, and bad breath, the additional acupoints of Neiting, Quchi, and Hegu were treated using a needling treatment that adopted the reducing method or the reinforcing and reducing method. (ii) For patients who suffered from stomach cold, fear of wind and cold, and preference for warmth, the additional acupoints of Baihui, Shenwang, and Guanyuan were treated using the tonifying method (Shenque without acupuncture) with enhanced moxibustion. (iii) For patients who suffered from deficient spleens, profuse sputum, anorexia, or who vomited translucent phlegm, the additional acupoints of Sanyinjiao and Fonglong were treated using the combined tonifying and reducing method. Specifically, after lifting the needle, a moving cupping was applied to the Beiyu acupoints where the cup stayed for 10 minutes. (iv) For patients who suffered from liver qi that damaged the stomach, acid reflux, and sternocostal pain, the additional acupoints of Taichong and Qimen were included using the even reinforcing and reducing method. One course of treatment contained ten such manipulations and was followed by a 3-day break. In general, one to two additional courses of acupuncture and moxibustion were still required after a patient stopped vomiting and his or her symptoms completely disappeared to regulate and reinforce the stomach qi and consolidate the curative effect. The results showed that 80 patients were cured (95.24%), and four patients displayed improvements (4.76%) after the aforementioned procedures were applied. The total efficacy rate was 100%. A 1-year follow-up was conducted for the 80 cured patients and did not reveal any recurrent cases.
(II) Acupoint application study
The most frequently employed acupoint to treat vomiting is Neiguan followed by Zusanli. These acupoints are the most frequently reported by clinical studies of vomiting. The related literature has reported methods involving Neiguan including single-point needling, matching acupoints, drug injections, and acupoint blocks. Zusanli manipulations mainly involve acupoint injections, acupoint blocks, and matching acupoints; however, single-point needling has not been reported for this site. The other employed acupoints include Zhongkui, Zhongwan, Gongsun, Juque, Dazhui, Baihui, Neiting, Jinjin, and Yuye. The applied ear acupoints primarily include the Wei (stomach), Ge (diaphragm), Shenmen, Shenshangxian (suprarenal gland), and Jiaogan (sympathetic nervous system) acupoints.
(i) Neiguan acupoint
This acupoint is a hand-jueyin pericardium and one of the eight confluence points. It has the therapeutic effects of channeling the yin and maintaining pulse and is particularly effective at curing stomach diseases because it can harmonize the stomach, reduce qi counter flow, relieve spasms, and stop vomiting. Although this acupoint is not associated with the foot-yangming meridian or the foot-taiyin spleen meridian, it is the clinically preferred treatment site for vomiting. For example, Neiguan acupuncture (28) was used to treat 13 patients with nervous vomiting. Specifically, 2-3 needling times were performed each day, which (in general) leads to recovery within 2-3 days. The results showed that 11 patients stopped vomiting after the first treatment, and the remaining two patients experienced slight nausea but showed no vomiting after the needling was withdrawn. None of the cases exhibited a recurrence of vomiting at their 6-month follow-up visit. In another report (29), single-point needling at Neiguan was performed to treat 35 patients whose vomiting resulted from drug-induced abortions. These patients were compared with a control group of 69 people. The results revealed that 30 individuals in the Neiguan-needling group were cured of vomiting, whereas five patients still displayed vomiting. Moreover, in the control group, 45 patients were cured of vomiting, and 24 patients were still vomiting. A between-group comparison yielded significant differences.
(ii) Zusanli acupoint
The Zusanli is a confluent acupoint of the Wei (stomach) meridian of foot-yangming and has invigorating effects. In fact, it is a crucial point with regard to health protection; acupuncture at this site can regulate the middle warmer, harmonize the stomach, reduce qi counter flow, eliminate distension, and control vomiting. It is also one of the most commonly addressed acupoints to treat vomiting. Liang Dongyun et al. (30) used a metoclopramide injection to perform a Zusanli acupoint block in 34 patients who suffered from chemotherapy-induced vomiting. The results showed that 28 patients showed improvements after the first administration and that 6 were effectively cured, yielding a total efficacy rate of 100%. TCM professionals often use the Neiguan and Zusanli acupoints to treat various cases of vomiting and subsequently generate successful outcomes. Cui Meiqing et al. (31) used a metoclopramide preparation with vitamin B6 to perform acupoint injections at the Neiguan and Zusanli acupoints in 44 patients with acute leukemia who were undergoing chemotherapy and displayed vomiting. These patients were compared with a control group of 22 patients treated with metoclopramide. The results showed that the former group had significantly better outcomes than did the control group (P<0.01). Cheng Cuihua et al. (32) used a vitamin B1 and metoclopramide preparation to perform acupoint injections at the Neiguan and Zusanli acupoints to treat 30 patients with vomiting due to various causes, including 8 patients with deficiencyresultant vomiting. The results revealed that this method led to a satisfactory efficacy for patients with deficiencyresultant vomiting and had an efficacy rate of 100%.
Acupoint application
The acupoint application of TCM takes advantage of the direct and indirect effects of drugs to produce certain acupoint stimulations. Subsequently, specific active ingredients pass through the skin to reach deep into the acupoints where they are transported via meridians to either treat the origins or circulate in the body. As such, these ingredients regulate meridians and organs to generate pharmacological effects and systemic outcomes, thereby achieving the therapeutic goal of strengthening the vital qi to eliminate pathogenic factors, reinforce deficiencies, and reduce excessiveness. Chinese medicine patching or magnetic patching can facilitate this approach. The former treatment uses an herbal application to treat vomiting. The latter involves the adoption of magnetic discs in which a magnetic field produces a lasting positive stimulation to a specific acupoint. The magnetic approach can yield similar curative effects to those of needling but avoids the pain and labor-intensiveness of acupuncture. In other words, it has satisfactory efficacy, a low cost, and is easy to administer; thus, it is a classical model of treating internal diseases with external methods.
Nursing and prevention
An appropriate diet serves to increase patients’ appetites, diminish their gastrointestinal reactions, and ensure an adequate nutritional supply. Designing personalized recipes to improve overall patient condition is recommended. Medicated diets belong to a treatment method that integrates food and medicine in which meals not only supply nutrients but also facilitate a cure. The use of medicated diets should follow the principle of symptom-differentiation-based treatment (33). Hence, implementing a clinical diet and managing food is necessary. Importantly, the treatment of certain diseases should not only focus on drugs; rather, it ought to choose safer as well as more effective and useful ways to achieve greater outcomes at a small cost. In this regard, diet management (e.g., reasonable eating times, food adjustments, and medicated diets) creates an alternative clinical treatment of vomiting. In addition, it is important to monitor the patient’s disease and other conditions so that they can be advised to rest when appropriate. This practice should be combined with diet measures such as eating easily digestible and nutritious foods and consuming multiple small meals. Likewise, it is better to eat several small meals when taking antiemetics. Frequent vomiting necessitates the identification of its cause and the replenishment of bodily fluids, the latter of which to prevent an electrolyte imbalance. Furthermore, it is important to prevent the damage caused by unfavorable environmental factors, assume healthy daily routines and diets (i.e., avoiding binge eating, the excessive consumption of raw, cold, fatty, and sweet foods as well as alcohol), be aware of the need to relax and regulate emotions, and participate in cultural and sports activities at the proper intensity.
Conclusions
TCM argues that vomiting has a complex etiology; therefore, it involves a variety of therapeutic techniques. Nevertheless, the key to treatment lies in harmonizing the stomach and diminishing qi counter flow. In addition, based on different etiologies and pathogeneses, vomiting treatment strategies can be divided into four types: direct antiemetic treatments, approaches based on eliminating pathogenic factors, approaches based on strengthening the vital qi, and approaches that target sites other than the origin. As such, the properties of cold/heat and deficiency/excess should be elucidated. The application of syndrome-differentiation-based treatments lie mostly in harmonizing the stomach and reducing qi counter flow, but the application should also account for the spleen, kidneys, liver, and gallbladder to provide the proper treatment. TCM is a great treasure because its theories have guided the clinical practices of various medical branches for thousands of years. TCM continues to be enriched and developed.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Wang B, eds. Yellow Emperor’s Inner Classic. Plain questions. Beijing: People’s Medical Publishing House, 1963.
- Zhao XK, eds. Comprehensive Medical Knowledge. Beijing: Academe publishing house, 2005.
- Shang ZJ, eds. Collation and annotation of Shen Nong’s Herbal Classic. Beijing: Academe publishing house, 2008.
- Sun SM. eds. Thousand-Golden-Prescriptions. Beijing: People’s Medical Publishing House, 1982.
- Xu HW, Zhang H. Study on Kidney-based treatments for vomiting. Shan Xi Zhong Yi Xue Yuan Xue Bao 1997;20:16-7.
- Li R. Understanding of Kidney-based treatments for vomiting. Zhen Jiu Lin Chuang Za Zhi 1996;12:8-9.
- Li XC. Synecdoche of Lung-based treatments of vomiting. Guang Ming Zhong Yi 1998;13:38-9.
- Liu XD. Three Lung-based treatments of vomiting and hiccup. Jiang Xi Zhong Yi Yao 1998;29:26.
- Cao HB, Zhou MS. Understanding of liver-based treatments for vomiting. Shan Xi Zhong Yi 1992;8:35.
- Zhang ZX. Analysis on 30 case of liver-based treatments for vomiting. Gan Su Zhong Yi 2006;19:30.
- Yin WX, Yin KW. Antiemetic effects of Panax notoginseng on vomiting caused by brain concussion. Zhong Yi Za Zhi 1994;35:135.
- Zhang LY. Antiemetic effects of extract of ginger (EG) in rats of kaolin pica models. Zhong Guo Yi Yao Zhi Nan 2008;6:23-5.
- Zhao DX, Yang ZH, Li M, et al. Anti-emetic effects of ginger on a nausea model of mink. Chin Pharm Affairs (Chin) 2006;10:601-4.
- Zhang ZS, Zhang SW, Cui C. Effect of Rhizoma Acori Graminei on treatment of neural vomiting. Zhong Yi Za Zhi 1996,37:711-2.
- Wang GD, Yang XD. Pharmacology of Pinellia ternata. Guo Wai Yi Xue Zhong Yi Zhong Yao Feng Ce 1985;7:24-5.
- Xiao PG. Modern Chinese Material Medica. China: Chemical Industry Press, 2002.
- Wu H, Cai BY, Rong GX, et al. Impact of Pinellia ternata prepared with ginger on function of gastrointestinal tract. Zhong Guo Zhong Yao Za Zhi 1994;19:535-7.
- Li JW, Yu YA, Cai JF, et al. Dictionary of Traditional Chinese Medicine. China: People’s Medical Publishing House, 1995.
- He YQ. The usage of Fructus forsythia for treatment of vomiting. Shan Xi Yi Yao 2001;17:41.
- Long SZ, Zheng MZ, Lin MJ. Clinical Study of Lemon for Relieving a Vomit after Operation. She Zhi 2007;19:116-7.
- Chen WY. Clinical observation of lemon for prophylaxis and treatment of postoperative nausea. Nan Fang Hu Li Za Zhi 1996;3:32.
- He YZ. The active component screening of Alpinia Kasumadai using for arresting vomiting. Guo Wai Yi Xue Zhong Yi Zhong Yao Fen Ce 1999;21:61.
- Zhang XK, Li JM, Zhang XX, et al. Therapeutic efficacy of Radix clematidis for nausea and vomitting after chemotherapy. Shan Xi Yi Yao Za Zhi 1989;18:283.
- Chen Di, He R, Li CJ. Study of active components of Galangal on analgesia and arresting vomiting. Guang Zhou Zhong Yi Yao Da Xue Xue Bao 2001;18:240-2.
- Yang ZH, Zhao DX, Hou HY, et al. Antiemetic effects of extract of capsicum on emesis in three rat models of kaolin pica. Zhong Guo Xin Yao Za Zhi. 2007;16:1682-4.
- Yang H. Study of active components of Lanxiang (a kind of herb) on arresting vomiting. Guo Wai Yi Xue Zhong Yi Zhong Yao Fen Ce 1998;20:61.
- Huang DJ, Sun ZC. Acupuncture therapy featuring zhongkui acupoint on 84 cases of neural vomiting. Zhen Jiu Lin Chuang Za Zhi 2000;16:49-50.
- Fan BC. An observation on acupuncture treatment of 13 cases of psychogenic vomiting. Shang Hai Zhen Jiu Za Zhi 2004;23:44-5.
- Qin XJ. The clinical observation on acupuncture Neiguan point of 104 cases of vomiting caused by drug abortion. Bei Jing Zhen Jiu Gu Shang Xue Yuan Xue Bao 1997;4:21.
- Liang DY, Li Z. Metoclopramide acupoint treatment of 34 cases of vomiting after radiotherapy. Qi Lu Zhong Liu Za Zhi 1994;3:76-7.
- Cui MQ, Yang XJ. Effect of point injection of Metoclopramide plus Vitamin B6 on chemotherapy induced nausea and vomiting. Guang Dong Yi Xue Yuan Xue Bao 2001;19:312.
- Cheng CH, Wu JD, Yao WZ. Curative effect observation of injection therapy for vomiting in Bilateral Zusanli points and Neiguan points. Zhong Yi Yao Yan Jiu 2001;17:33.
- Shi XJ. The opsonization and treatment effect of medicined diet on gastrointestinal reaction after chemotherapy for tumor. Gan Su Zhong Yi 2009;22:36-7.